Healthcare providers face increasing administrative complexity when managing credentialing requirements across multiple insurance networks. The process of verifying qualifications, maintaining accurate provider data, and ensuring proper enrollment with payers directly impacts a practice's ability to receive reimbursements. Provider credentialing services offer specialized support to navigate these challenges, allowing practices to focus on patient care while ensuring compliance with payer requirements and industry standards. Understanding how these services work and their impact on revenue cycle management helps healthcare organizations make informed decisions about outsourcing versus managing credentialing internally.
What Provider Credentialing Services Include
Provider credentialing services encompass a comprehensive range of activities designed to verify, document, and maintain healthcare professionals' qualifications with insurance carriers and healthcare networks. These services handle the entire lifecycle of credentialing from initial application through ongoing monitoring and re-credentialing.
The core function involves collecting and verifying provider information including education, training, board certifications, work history, malpractice insurance, and state licensure. Professional credentialing specialists validate this information against primary sources such as medical schools, residency programs, and state licensing boards.
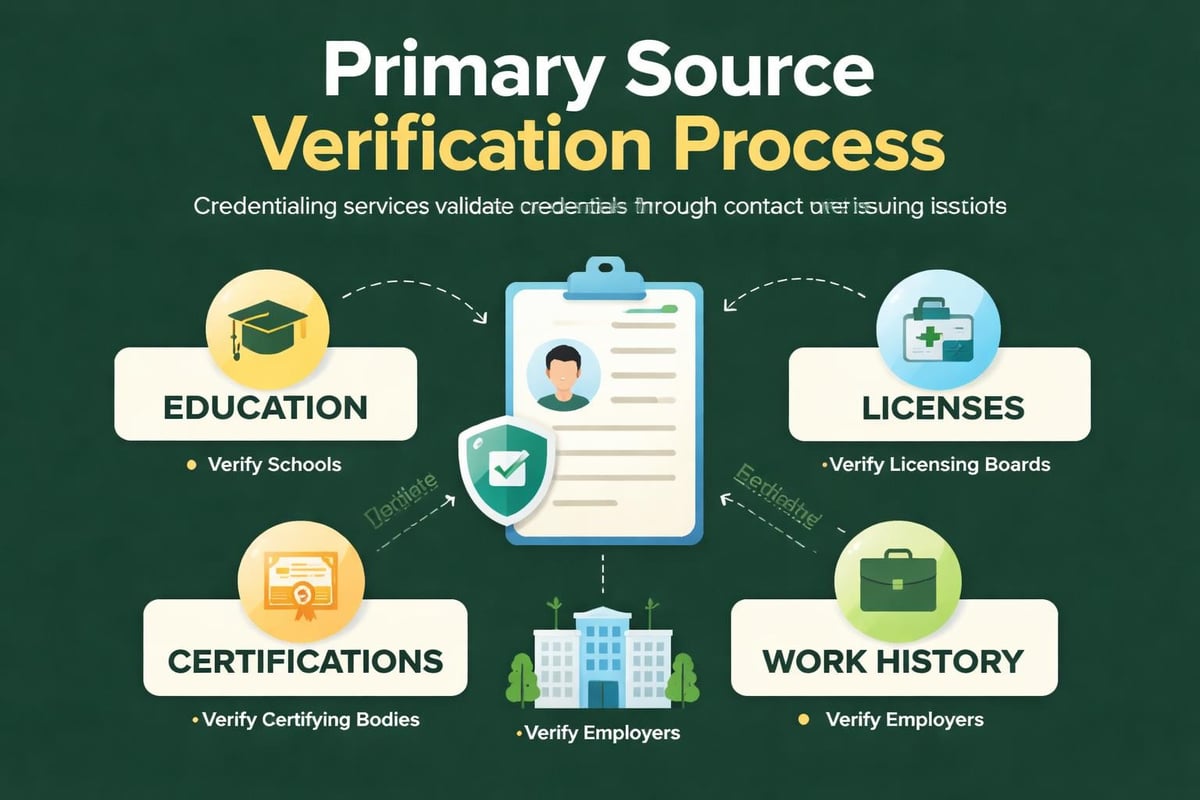
Initial Credentialing Process
The initial credentialing process typically requires 90 to 120 days for completion, though timelines vary by payer and specialty. This extended timeframe makes professional management essential for new practices or providers joining established groups.
Key steps in initial credentialing include:
- Application preparation – Gathering all required documentation and completing payer-specific applications
- Primary source verification – Contacting educational institutions, licensing boards, and certification bodies
- Database registration – Enrolling providers in CAQH ProView and other credentialing databases
- Submission and follow-up – Filing applications with each payer and tracking progress
- Enrollment completion – Obtaining approval letters and effective dates
Many healthcare organizations leverage credentialing solutions to streamline data management across multiple payers. These systems reduce redundant data entry and improve accuracy throughout the process.
Re-Credentialing and Ongoing Maintenance
Provider credentialing services extend beyond initial enrollment. Insurance carriers require periodic re-credentialing, typically every 24 to 36 months, to verify that providers maintain current qualifications and meet ongoing standards.
Re-credentialing involves updating provider information, renewing expiring credentials, and submitting updated applications before deadlines. Missing re-credentialing deadlines can result in termination from insurance networks, creating gaps in coverage that prevent claim submission and delay revenue.
| Credential Type | Typical Renewal Period | Verification Required |
|---|---|---|
| State Medical License | 1-2 years | Primary source verification |
| DEA Registration | 3 years | Federal database check |
| Board Certification | 10 years (varies) | Specialty board confirmation |
| Malpractice Insurance | 1 year | Certificate of coverage |
| Hospital Privileges | 2 years | Facility verification |
Benefits of Professional Provider Credentialing Services
Healthcare practices that partner with specialized provider credentialing services gain significant operational advantages. These benefits extend across revenue cycle performance, compliance management, and administrative efficiency.
Accelerated Revenue Recognition
Delays in credentialing directly impact cash flow. Every day a provider remains uncredentialed represents lost revenue from services that cannot be billed to insurance carriers. Professional credentialing services expedite this process through established relationships with payers and systematic follow-up procedures.
Experienced credentialing specialists understand payer-specific requirements and common pitfalls that cause application delays. They prepare complete, accurate applications on the first submission, avoiding the rejections and requests for additional information that extend timelines.
Financial impact of credentialing delays:
- Average provider generates $50,000 to $100,000 monthly in billable services
- 30-day credentialing delay equals one month of lost revenue
- Retroactive billing policies vary by payer and are not guaranteed
- Claims submitted before effective credentialing dates face automatic denial
Reduced Administrative Burden
Managing credentialing internally requires dedicated staff time to track requirements, communicate with payers, and maintain documentation. For small to mid-sized practices, this workload often falls on office managers or billing staff who must balance credentialing with their primary responsibilities.
Provider credentialing services eliminate this burden by handling all aspects of the process. This allows practice staff to focus on revenue cycle management activities that directly support operations and patient care.
The administrative complexity multiplies with each additional provider and payer contract. A practice with five providers participating in ten insurance networks manages 50 unique credentialing relationships, each with different requirements and renewal schedules.

Enhanced Compliance and Risk Management
Credentialing errors expose practices to significant compliance risks. Billing for services provided by uncredentialed or improperly credentialed providers constitutes fraud, potentially triggering audits, recoupment demands, and penalties.
Professional services maintain detailed audit trails documenting all verification activities and source confirmations. This documentation protects practices during payer audits and demonstrates compliance with credentialing standards established by accrediting organizations.
Credentialing specialists also monitor expiring credentials and initiate renewal processes proactively. This prevents lapses in licensure or certification that would require suspension from insurance networks and halt claim processing.
Common Credentialing Challenges and Solutions
Healthcare organizations encounter predictable obstacles during credentialing regardless of size or specialty. Understanding these challenges helps practices evaluate whether provider credentialing services offer appropriate solutions for their specific situations.
Application Errors and Incomplete Documentation
Insurance carriers reject credentialing applications for missing information, inconsistent data, or failure to include required supporting documents. Each rejection adds weeks to the credentialing timeline while the practice gathers additional materials and resubmits.
Common application errors include:
- Gaps in employment history without explanation
- Mismatched names across different documents
- Missing attestations or required signatures
- Expired malpractice certificates
- Incomplete CME documentation
Professional credentialing services implement quality control processes that catch these errors before submission. They maintain comprehensive checklists for each payer's requirements and verify completeness before filing applications.
Payer Communication Delays
Insurance carriers often take weeks to respond to credentialing inquiries or requests for status updates. Practices managing credentialing internally struggle to maintain consistent follow-up while handling their regular workload.
Credentialing services dedicate staff specifically to payer outreach and follow-up. Their higher volume of applications often provides access to dedicated payer representatives who can expedite processing and resolve issues more quickly than individual practices can achieve.
| Challenge | Internal Management | Professional Service |
|---|---|---|
| Application tracking | Manual spreadsheets | Automated systems with alerts |
| Payer follow-up | Occasional calls | Daily systematic outreach |
| Error resolution | Learning by trial | Established payer relationships |
| Documentation storage | Paper files or basic scanning | Secure digital credential files |
Understanding the Difference Between Credentialing and Enrollment
Many healthcare providers confuse credentialing with payer enrollment, though these represent distinct processes within the broader revenue cycle. Credentialing versus enrollment differences impact how practices approach each activity.
Credentialing verifies provider qualifications and eligibility to deliver healthcare services. Payer enrollment establishes the business relationship allowing claim submission and reimbursement. Both must be complete before a provider can bill insurance for services rendered.
Provider credentialing services typically handle both processes as integrated activities, ensuring seamless progression from qualification verification through final enrollment. This coordination prevents gaps where credentialing completes but enrollment remains pending, a common scenario when processes are managed separately.
Selecting Provider Credentialing Services for Your Practice
Healthcare organizations evaluating credentialing partners should assess specific capabilities that align with their practice needs. Not all provider credentialing services offer identical support levels or specialized expertise relevant to every specialty and practice type.
Evaluating Service Scope and Capabilities
Comprehensive provider credentialing services should offer end-to-end support including initial credentialing, payer enrollment, re-credentialing, ongoing monitoring, and credential verification organization (CVO) services for hospital privileges.
Essential service components include:
- CAQH ProView profile creation and maintenance
- Individual payer application completion and submission
- Primary source verification documentation
- Medicare and Medicaid enrollment (PECOS, state Medicaid)
- Hospital medical staff credentialing
- Expiration tracking and renewal management
- Sanction screening and exclusion monitoring
Practices should verify that credentialing services maintain current knowledge of common credentialing practices and evolving payer requirements. Regulatory changes in healthcare credentialing occur regularly, and outdated processes can delay approvals or result in non-compliance.
Technology and Reporting Capabilities
Modern credentialing management relies on technology platforms that track application status, store documentation, and alert practices to upcoming expirations. Provider credentialing services should offer client access to real-time status dashboards and detailed reporting.
Look for partners who provide:
- Secure online portals for document submission and status checking
- Automated alerts for credential expirations and renewal deadlines
- Detailed progress reports showing where each application stands in the approval process
- Integration capabilities with practice management systems
- Digital credential storage meeting HIPAA security requirements
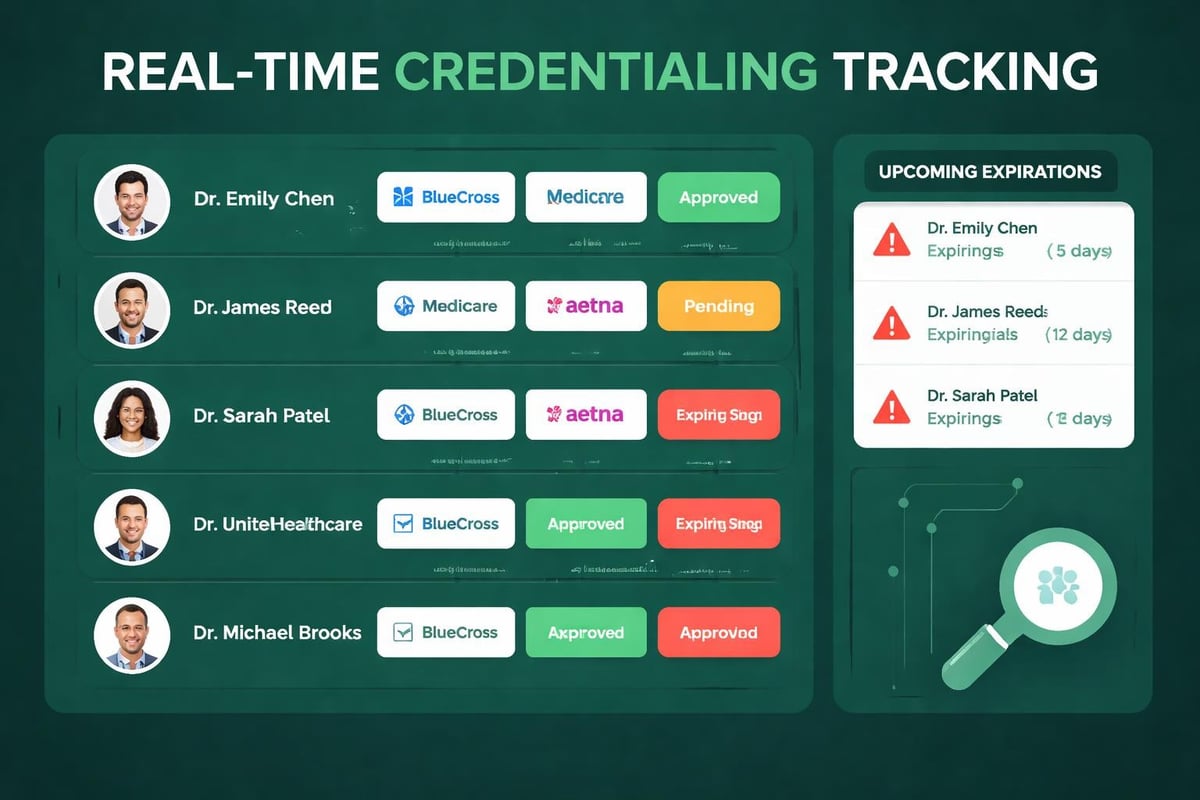
Technology integration becomes particularly important for practices working with comprehensive revenue cycle management services where credentialing data must flow seamlessly to billing systems for accurate claim submission.
Specialty-Specific Experience
Certain medical specialties face unique credentialing requirements or work with specialized insurance products. Provider credentialing services with relevant specialty experience navigate these nuances more effectively than generalist vendors.
Behavioral health providers, for example, encounter distinct credentialing pathways and payer relationships compared to surgical specialties. Similarly, practices offering behavioral health services benefit from credentialing partners familiar with mental health payer networks and telehealth credentialing requirements.
Ask potential credentialing partners about:
- Their experience with your specific specialty
- Volume of providers they credential in your field
- Relationships with payers common to your specialty
- Understanding of specialty-specific certification requirements
- Track record with specialty hospital credentialing
Impact on Revenue Cycle Performance
Provider credentialing services influence multiple aspects of revenue cycle performance beyond the obvious impact of enabling claim submission. The quality and timeliness of credentialing affects denial rates, payment speed, and long-term payer relationships.
Connection to Denial Management
Credentialing errors represent a preventable cause of claim denials. When billing staff submit claims before credentialing completes, with incorrect provider identifiers, or after credentials lapse, payers deny payment automatically.
These denials in medical billing require significant time to research and appeal, often with low success rates. Practices must either write off the revenue or pursue patient responsibility, damaging patient relationships and creating collection challenges.
Effective provider credentialing services reduce payer denials through accurate data management and proactive credential monitoring. This prevention-focused approach proves more efficient than managing denials after they occur.
Common credentialing-related denial codes:
- CO-16: Claim lacks information needed for adjudication
- CO-27: Services not covered for this provider
- CO-197: Provider not on file or not participating
- CO-234: Provider information not found for included provider
Provider Data Accuracy Across Systems
Insurance carriers, clearinghouses, and healthcare organizations maintain separate provider databases that must contain consistent information. Discrepancies between NPI records, CAQH data, and payer files cause claim processing delays and denials.
Provider credentialing services serve as a central point for maintaining accurate provider information across all platforms. When a provider's address changes, their license renews, or group affiliations update, credentialing specialists ensure all relevant databases reflect these changes.
This data stewardship function verifies healthcare professionals’ expertise and ensures that payer systems contain current information for claim routing and reimbursement processing.
Optimizing Network Participation Strategy
Not all insurance contracts offer equal reimbursement rates or patient volume. Strategic practices evaluate which payer networks justify the time and cost of credentialing based on their patient population and revenue goals.
Provider credentialing services support this strategic approach by offering insights into credentialing timelines, network requirements, and relative value of different payer relationships. Their experience across multiple practices provides benchmarking data that informs network participation decisions.
For practices entering new markets or adding providers, credentialing services help prioritize payer applications based on regional insurance coverage patterns and estimated patient revenue potential.
Internal Credentialing Versus Outsourced Services
Healthcare organizations must decide whether to manage credentialing internally or partner with provider credentialing services. This decision depends on practice size, staff capabilities, and strategic priorities.
When Internal Credentialing Makes Sense
Small practices with one or two providers participating in limited insurance networks may successfully manage credentialing internally. The workload remains manageable, and practices gain direct control over the process and timeline.
Internal credentialing works best when:
- The practice has dedicated administrative staff with credentialing expertise
- Provider roster and payer participation remain relatively stable
- The organization maintains organized systems for tracking renewals
- Staff have established relationships with local payer representatives
Even practices managing credentialing internally often benefit from professional support during growth phases, such as adding new providers or expanding into additional insurance networks.
Advantages of Outsourcing to Provider Credentialing Services
Most multi-provider practices find that outsourcing credentialing delivers better results at lower overall cost than internal management. The specialized expertise, established payer relationships, and systematic processes of provider credentialing services produce faster credentialing with fewer errors.
Outsourcing proves particularly valuable for:
- Rapidly growing practices adding providers frequently
- Organizations expanding into new geographic markets
- Practices with high provider turnover requiring continuous credentialing
- Healthcare systems managing credentialing across multiple locations
- Specialties with complex credentialing requirements
The cost of provider credentialing services typically represents a fraction of the revenue loss from credentialing delays. A one-month delay in credentialing a provider who generates $75,000 monthly in collections far exceeds the annual cost of professional credentialing support.
Credentialing for Different Provider Types
Provider credentialing services must adapt their approach based on the type of healthcare professional seeking enrollment. Physicians, nurse practitioners, physician assistants, and other providers face different credentialing pathways and requirements.
Physician Credentialing Requirements
Physicians complete the most extensive credentialing process, reflecting their independent practice authority and broad scope of services. Payers verify medical school graduation, residency completion, board certification status, and detailed practice history.
Primary care physicians often find credentialing relatively straightforward, while specialists may encounter additional requirements related to procedure-specific competencies or facility-based privileges. Surgical specialists, for example, must document training and experience with specific procedures.
Mid-Level Provider Credentialing
Nurse practitioners, physician assistants, and other advanced practice providers face credentialing requirements similar to physicians but adapted to their scope of practice and supervisory relationships. Some payers credential mid-level providers independently, while others require association with a supervising physician.
Provider credentialing services must understand state-specific scope of practice regulations that affect how mid-level providers are credentialed and enrolled. These regulations vary significantly across states and impact billing procedures and reimbursement structures.
Allied Health Professional Credentialing
Physical therapists, occupational therapists, speech-language pathologists, and other allied health professionals pursue credentialing through specialized pathways relevant to their disciplines. Requirements focus on professional licensure, specialty certifications, and facility-based privileges where applicable.
The complexity of allied health credentialing depends on whether providers work in independent practice settings or as part of hospital or clinic-based services. Provider credentialing services adjust their approach based on these practice arrangements and associated payer requirements.
Measuring Credentialing Service Performance
Healthcare organizations partnering with provider credentialing services should establish clear performance metrics to evaluate service quality and return on investment. Objective measurement ensures accountability and identifies opportunities for process improvement.
Key Performance Indicators
Track these credentialing metrics:
- Average time from application initiation to payer approval
- Percentage of applications approved on first submission
- Number of credentialing-related claim denials
- Provider revenue recognition timeline for new hires
- Credential expiration incidents requiring emergency processing
- Cost per provider credentialed compared to internal benchmarks
Leading provider credentialing services provide regular reporting on these metrics and demonstrate continuous improvement over time. They should also benchmark your practice's performance against industry standards and similar organizations.
Financial Impact Assessment
Calculate the financial value of credentialing services by comparing revenue recognition timelines and denial rates before and after outsourcing. Include both direct costs (service fees) and indirect benefits (staff time reallocation, reduced denials, faster provider onboarding).
A comprehensive financial analysis accounts for:
- Reduction in credentialing timeline measured in days
- Daily revenue value per provider based on average collections
- Denial recovery rate for credentialing-related denials
- Administrative staff hours redirected to revenue-generating activities
- Risk mitigation value from improved compliance and audit readiness
This data-driven approach demonstrates whether provider credentialing services deliver measurable value beyond their cost, supporting informed decisions about continuing or adjusting the partnership.
Effective provider credentialing services streamline the complex verification and enrollment processes that enable healthcare organizations to receive timely reimbursement for services rendered. By managing credentialing professionally, practices reduce administrative burden, minimize revenue delays, and maintain compliance with evolving payer requirements. Greenhive Billing Solutions offers comprehensive credentialing support integrated with complete revenue cycle management services, ensuring your providers achieve enrollment efficiently while your practice maintains focus on delivering quality patient care. Our experienced team handles every aspect of credentialing, from initial applications through ongoing maintenance, delivering the expertise and systematic approach that maximizes your reimbursement potential.

