Selecting the right revenue cycle management partner represents one of the most critical decisions healthcare providers face in maintaining financial stability and operational efficiency. As reimbursement models grow increasingly complex and administrative burdens continue to mount, identifying the best revenue cycle management companies becomes essential for practices seeking to optimize cash flow, reduce claim denials, and focus on patient care. The landscape of RCM providers has evolved significantly, with numerous companies offering specialized services ranging from end-to-end billing solutions to targeted support in specific areas like denial management or credentialing.
What Defines the Best Revenue Cycle Management Companies
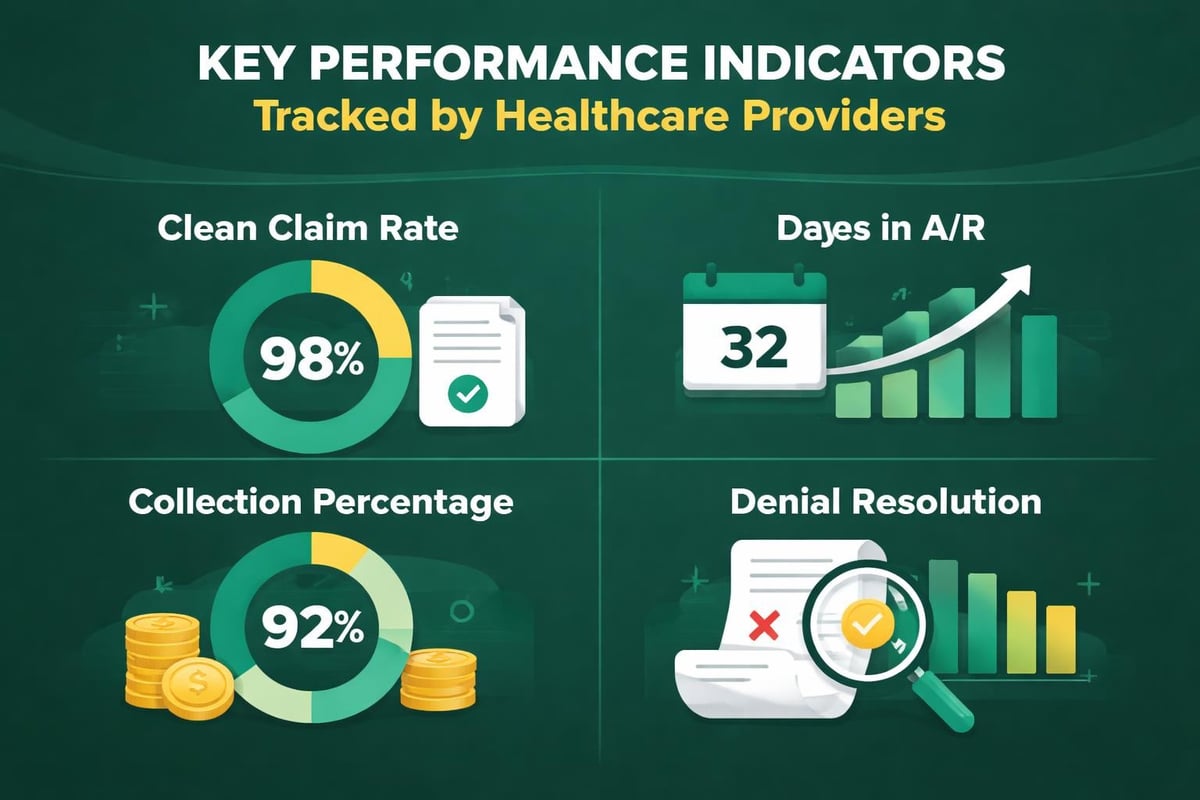
Top-tier revenue cycle management partners distinguish themselves through several measurable criteria that directly impact provider financial performance. These organizations demonstrate consistent results in clean claim rates, days in accounts receivable, and collection percentages while maintaining full HIPAA compliance and transparent communication protocols.
Performance Metrics That Matter
The best revenue cycle management companies consistently achieve clean claim rates exceeding 95%, meaning fewer rejections and faster reimbursements for healthcare providers. Days in accounts receivable (A/R) typically remain below industry averages, with leading companies maintaining A/R periods of 30-40 days compared to the industry standard of 50-60 days.
Collection rates serve as another critical benchmark. Elite RCM providers regularly achieve collection rates above 97% for in-network claims, demonstrating their expertise in denial management services and follow-up processes.
Key performance indicators include:
- First-pass claim acceptance rates
- Average reimbursement timelines
- Denial overturn percentages
- Patient satisfaction scores
- Compliance audit results
According to industry rankings of top RCM vendors, market leaders demonstrate sustained performance across these metrics over multiple fiscal quarters, proving their systems and processes deliver reliable results.
Comprehensive Service Offerings
The most effective revenue cycle management companies provide integrated services that address every stage of the revenue cycle, from patient registration through final payment posting and reconciliation. This comprehensive approach ensures continuity and reduces the risk of revenue leakage at any point in the billing process.
Front-End Revenue Cycle Services
Excellence in front-end operations sets the foundation for successful revenue capture. Leading providers offer robust eligibility verification services that confirm insurance coverage before services are rendered, dramatically reducing the incidence of claim denials due to coverage issues.
Prior authorization management represents another critical front-end function. The best companies maintain dedicated teams familiar with payer-specific requirements, ensuring timely approvals and preventing service delays. This proactive approach protects providers from revenue loss while maintaining patient satisfaction.
Essential front-end services include:
- Real-time insurance verification
- Prior authorization coordination
- Patient demographic accuracy validation
- Financial counseling support
- Registration quality assurance
Mid-cycle operations focus on accurate charge capture and coding precision. Top providers employ certified coders with specialty-specific expertise, ensuring codes accurately reflect services rendered while maximizing appropriate reimbursement.
Back-End Revenue Cycle Excellence
The back-end revenue cycle encompasses medical claim submission services, payment posting, and accounts receivable management. Superior RCM companies leverage technology to automate routine tasks while maintaining human oversight for complex cases requiring specialized attention.
Denial management capabilities particularly distinguish leading providers. These organizations maintain detailed denial tracking systems, identifying patterns and implementing preventive measures to reduce future rejections. Their teams understand payer-specific appeal processes and successfully overturn a high percentage of initial denials.
| Service Category | Leading Companies | Average Providers |
|---|---|---|
| Clean Claim Rate | 95-98% | 85-90% |
| A/R Days | 30-40 | 50-60 |
| Collection Rate | 97%+ | 92-95% |
| Denial Overturn | 65-75% | 40-50% |
Technology Integration and Adaptability
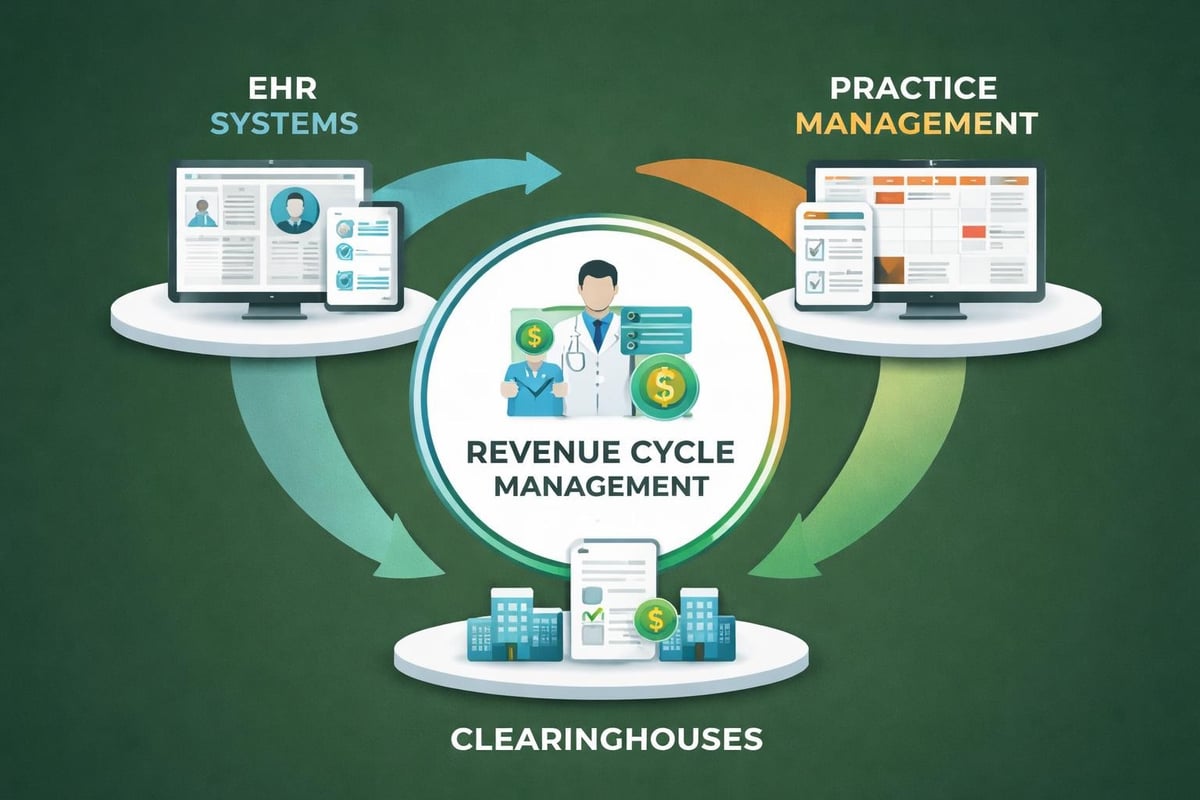
Distinguished revenue cycle management providers demonstrate exceptional technological capabilities while maintaining the flexibility to work within existing practice management systems. Rather than forcing clients onto proprietary platforms, the best companies adapt their workflows to complement client-owned software.
This adaptability proves particularly valuable for healthcare organizations that have invested significantly in their current technology infrastructure. Skilled RCM teams work seamlessly with various electronic health record (EHR) systems, practice management software, and clearinghouse platforms, ensuring continuity and minimizing disruption.
Advanced Analytics and Reporting
Top performers in the RCM industry provide sophisticated reporting capabilities that offer actionable insights into practice financial performance. These analytics extend beyond basic collection reports to include payer mix analysis, procedure profitability assessment, and trending data that informs strategic decision-making.
Research on leading RCM companies highlights how advanced data analytics separate industry leaders from average providers. The ability to identify revenue opportunities, predict cash flow patterns, and highlight areas requiring attention adds substantial value beyond transactional billing services.
Transparency in reporting builds trust and enables healthcare providers to maintain visibility into their revenue cycle operations. The best revenue cycle management companies provide real-time dashboard access, customized reports, and regular performance reviews that demonstrate accountability and continuous improvement.
Specialty-Specific Expertise
Healthcare specialties present unique billing challenges requiring specialized knowledge of procedure codes, documentation requirements, and payer policies. The most effective RCM partners maintain teams with deep expertise in specific medical specialties, ensuring accurate coding and maximized reimbursement for specialized services.
Understanding Specialty Nuances
Cardiology practices face distinct billing complexities compared to dermatology or orthopedic practices. Procedure bundling rules, modifier requirements, and documentation standards vary significantly across specialties. Elite RCM companies assign dedicated teams familiar with these nuances, reducing coding errors and claim rejections.
For example, medical coding services for cardiology must account for complex bundling rules around diagnostic testing and interventional procedures. Coders require specific training in cardiovascular CPT codes, appropriate use of modifiers, and documentation requirements supporting medical necessity.
Specialty-specific considerations include:
- Procedure code knowledge and updates
- Modifier application expertise
- Documentation requirement familiarity
- Payer policy understanding by specialty
- Compliance with specialty-specific regulations
Practices benefit significantly when RCM partners maintain certification and continuing education programs ensuring their teams stay current with evolving coding standards and regulatory requirements. This investment in ongoing training directly translates to improved claim acceptance rates and reduced compliance risk.
Compliance and Security Standards
Healthcare data security and regulatory compliance represent non-negotiable requirements for any revenue cycle management partnership. The best companies demonstrate rigorous adherence to HIPAA regulations, implementing comprehensive security measures protecting patient information throughout the billing process.
HIPAA Compliance Framework
Leading RCM providers maintain documented policies and procedures addressing all aspects of HIPAA compliance, from workforce training to breach response protocols. Regular security audits, both internal and third-party, verify the effectiveness of protective measures and identify potential vulnerabilities.
Business associate agreements (BAAs) clearly define responsibilities and liabilities, providing legal protection for healthcare providers partnering with external RCM companies. These agreements specify data handling procedures, security requirements, and notification processes in the event of any security incident.
According to user reviews of top RCM vendors, security and compliance consistently rank among the highest priorities for healthcare organizations selecting revenue cycle partners. Providers cannot afford to compromise patient data security regardless of other performance benefits.
| Compliance Area | Best Practice Standard |
|---|---|
| Staff Training | Annual HIPAA certification required |
| Data Encryption | 256-bit encryption for data at rest and in transit |
| Access Controls | Role-based access with multi-factor authentication |
| Audit Logs | Comprehensive tracking of all PHI access |
| Incident Response | Documented protocols with 24-hour notification |
Client Communication and Support
Responsive communication distinguishes exceptional revenue cycle management companies from adequate providers. The best organizations assign dedicated account managers who serve as primary contacts, ensuring consistent communication and deep familiarity with each client's unique needs and preferences.
Regular performance reviews provide opportunities to discuss metrics, address concerns, and identify improvement opportunities. These meetings demonstrate accountability while fostering collaborative relationships between RCM partners and healthcare providers.
Accessibility and Problem Resolution
When issues arise, immediate access to knowledgeable support staff becomes critical. Top RCM companies maintain multiple communication channels including phone, email, and secure messaging platforms, ensuring providers can quickly obtain assistance when needed.
Problem resolution processes distinguish superior providers. Rather than simply addressing symptoms, the best companies conduct root cause analysis to prevent recurring issues. This systematic approach to quality improvement creates lasting value beyond individual problem resolution.
The top healthcare revenue cycle management partners emphasize relationship building alongside technical expertise, recognizing that successful partnerships require trust, transparency, and mutual respect.
Scalability and Growth Support
Healthcare practices evolve over time, expanding services, adding providers, or opening new locations. The best revenue cycle management companies demonstrate the capacity to scale services in alignment with client growth, maintaining performance levels regardless of volume increases.
Flexible Service Models
Rather than one-size-fits-all approaches, leading providers offer customizable service packages addressing specific client needs and budgets. Some practices require comprehensive end-to-end billing support while others seek targeted assistance with particular aspects of the revenue cycle.
This flexibility extends to pricing models as well. The best companies offer transparent fee structures, whether percentage-based, per-claim, or hybrid models, ensuring alignment between provider success and RCM partner compensation.
Service scalability features include:
- Rapid onboarding for new providers
- Multi-location coordination capabilities
- Specialty expansion support
- Volume surge management
- Technology upgrade transitions
Organizations planning growth appreciate RCM partners with proven track records supporting practice expansion. This experience proves invaluable during critical transition periods when billing consistency directly impacts cash flow stability.

Industry Recognition and Track Record
Established reputation and industry recognition provide valuable indicators when evaluating potential revenue cycle management partners. Awards from respected healthcare publications, high rankings in comparative analyses, and positive client testimonials all contribute to building confidence in a provider's capabilities.
Evaluating Provider Credentials
Years in business demonstrate staying power and accumulated expertise. While newer companies may offer innovative approaches, established providers bring tested processes and proven results across diverse client scenarios and market conditions.
Client retention rates reveal satisfaction levels more accurately than marketing materials. The best revenue cycle management companies maintain long-term relationships with the majority of their clients, demonstrating consistent value delivery that justifies ongoing partnership.
Certification and accreditation from recognized industry organizations verify commitment to professional standards. Organizations like AAPC (American Academy of Professional Coders) and HFMA (Healthcare Financial Management Association) provide certification programs validating expertise and ethical practices.
Analysis from market intelligence reports on RCM companies helps healthcare providers understand market positioning and competitive advantages of various service providers. These independent assessments offer objective perspectives complementing vendor-provided information.
Cost-Effectiveness and ROI
While pricing naturally influences provider decisions, the lowest-cost option rarely delivers optimal value. The best revenue cycle management companies demonstrate clear return on investment through improved collections, reduced denials, faster reimbursements, and decreased administrative burden on internal staff.
Calculating True Value
Comprehensive cost analysis must account for both direct fees and indirect benefits. When an RCM partner reduces A/R days from 55 to 35, the improved cash flow creates tangible financial benefits beyond the service fees paid. Similarly, increased clean claim rates reduce staff time spent on rework and appeals.
Many practices discover that partnering with a professional RCM company actually costs less than maintaining internal billing departments when accounting for salaries, benefits, training, technology, and overhead. This proves particularly true for medical billing services for small practices where economies of scale favor external partnerships.
| Cost Consideration | Internal Billing | External RCM Partner |
|---|---|---|
| Staff Salaries | $120,000-180,000 annually | Included in service fee |
| Benefits/Payroll Tax | 25-30% of salaries | None |
| Software Licenses | $800-1,500 monthly | Included |
| Training/Education | $2,000-5,000 annually | Included |
| Overhead Allocation | Office space, equipment | None |
Making the Selection Decision
Choosing among the best revenue cycle management companies requires systematic evaluation aligned with specific practice needs, culture, and strategic objectives. Healthcare providers should develop clear selection criteria, conduct thorough due diligence, and engage multiple stakeholders in the decision process.
Structured Evaluation Process
Request for proposal (RFP) processes help standardize comparisons across potential partners. Well-structured RFPs should address service scope, technology requirements, reporting expectations, communication protocols, and pricing models while inviting vendors to demonstrate their unique capabilities.
Reference checks provide invaluable insights into real-world performance and partnership experiences. Speaking with current clients in similar specialties and practice sizes reveals information that proposals and presentations cannot convey. Asking specific questions about challenges, responsiveness, and long-term satisfaction yields particularly useful feedback.
Trial periods or pilot programs allow providers to assess performance before committing to long-term contracts. The best companies often welcome these arrangements, confident that demonstrated results will lead to expanded partnerships.
Selection criteria checklist:
- Demonstrated performance metrics in similar specialties
- Technology compatibility with existing systems
- HIPAA compliance documentation and security protocols
- Communication processes and account management structure
- Pricing transparency and contract terms
- Client references and industry reputation
- Scalability to support practice growth
- Staff qualifications and training programs
Comprehensive comparisons of RCM software and service providers offer starting points for evaluation, though providers should customize assessments based on individual circumstances and priorities.
Regional and Specialty Considerations
Location-specific regulatory requirements and payer environments influence RCM effectiveness. The best revenue cycle management companies maintain knowledge of state-specific Medicaid programs, regional commercial payers, and local compliance requirements affecting billing practices.
State-Specific Expertise
Practices operating in states with unique regulatory environments benefit from RCM partners familiar with local requirements. For example, medical billing services in California must navigate different workers' compensation billing rules than practices in other states.
Regional payer concentration also matters. An RCM company with strong relationships and deep knowledge of dominant payers in a specific geographic area delivers advantages through familiarity with those payers' specific requirements, payment timelines, and appeal processes.
Specialty-focused providers should prioritize RCM companies with demonstrated expertise in their specific field. The coding, documentation, and billing nuances of ophthalmology differ substantially from those of behavioral health or emergency medicine. Partnering with specialists in relevant areas reduces errors and maximizes appropriate reimbursement.
Future-Ready Revenue Cycle Partners
Healthcare continues evolving with new payment models, regulatory requirements, and technological advances. The best revenue cycle management companies demonstrate commitment to innovation and adaptation, positioning their clients for success regardless of industry changes.
Preparing for Industry Transitions
Value-based care models require different approaches to revenue capture and performance measurement than traditional fee-for-service billing. Forward-thinking RCM partners develop capabilities supporting quality metric reporting, risk-based contracting, and bundled payment models alongside conventional billing services.
Regulatory changes demand ongoing attention and rapid adaptation. Whether responding to new CPT codes, modifier requirements, or payer policy updates, elite RCM companies maintain processes ensuring immediate compliance while minimizing disruption to client operations.
Emerging technologies including artificial intelligence and machine learning increasingly influence revenue cycle operations. While service-based RCM companies rely primarily on skilled professionals rather than proprietary software, the best organizations leverage available technologies to enhance efficiency and accuracy in their service delivery.
According to profiles of top revenue cycle management companies, market leaders invest continuously in staff development, process improvement, and technology adoption to maintain competitive advantages and deliver superior client outcomes.
Selecting the right revenue cycle management partner fundamentally impacts healthcare practice financial performance and operational efficiency. By carefully evaluating potential partners against the criteria outlined above, providers can identify organizations delivering measurable results, responsive support, and long-term value. Greenhive Billing Solutions combines comprehensive RCM services with specialty-specific expertise, helping healthcare providers across the United States maximize reimbursements while maintaining compliance and transparency throughout the revenue cycle. Our experienced team works within your existing systems to deliver improved cash flow, reduced denials, and the financial clarity you need to focus on exceptional patient care.

