Medical billing involves countless codes and identifiers that ensure healthcare providers receive appropriate reimbursement for their services. Among these, j codes in medical billing represent a specialized subset dedicated to injectable medications, chemotherapy drugs, and other administered pharmaceuticals. Understanding these codes is essential for healthcare practices that regularly administer medications, as even minor coding errors can result in claim denials, delayed payments, or compliance issues. For revenue cycle management professionals, mastering J codes means the difference between optimized reimbursement and preventable revenue loss.
What Are J Codes in Medical Billing
J codes are specific alphanumeric identifiers within the Healthcare Common Procedure Coding System (HCPCS) Level II classification. These codes always begin with the letter “J” and are followed by four numeric digits, such as J1234. The American Medical Association provides comprehensive resources on CPT and HCPCS codes, including detailed guidance on proper J code application.
The primary purpose of j codes in medical billing is to identify non-orally administered medications, including injectable drugs, chemotherapy agents, and certain infusion therapies. Unlike oral medications that patients typically self-administer at home, these drugs require professional administration in clinical settings. This distinction is critical because it affects both reimbursement rates and documentation requirements.
The Structure and Components of J Codes
Each J code represents a specific medication, dosage, and unit of measurement. For example, one code might represent 10 mg of a particular drug, while another represents 50 mg of the same medication. This granular approach ensures precise billing that reflects the actual quantity administered to the patient.
Key characteristics of J codes include:
- Specific drug identification with exact chemical names
- Defined dosage amounts per billable unit
- Administration route specifications (intramuscular, intravenous, subcutaneous)
- National Drug Code (NDC) linkage for tracking and verification
The Centers for Medicare & Medicaid Services (CMS) maintains and updates these codes quarterly, adding new medications and discontinuing outdated ones as pharmaceutical markets evolve.

Why J Codes Matter for Healthcare Providers
Revenue cycle efficiency depends heavily on accurate coding practices, and j codes in medical billing play a substantial role in that ecosystem. Understanding common billing identifiers helps practices avoid the costly mistakes that lead to claim rejections.
Practices that specialize in oncology, rheumatology, ophthalmology, or pain management frequently encounter J codes in their daily operations. These specialties routinely administer high-cost medications that require precise documentation and coding.
Financial Impact of Accurate J Code Billing
The financial stakes surrounding J codes are considerable. Injectable medications often represent significant expenses for healthcare practices, particularly specialty drugs that can cost thousands of dollars per dose. When providers bill these medications incorrectly, they risk:
- Complete claim denial requiring time-intensive appeals
- Partial payment that doesn’t cover medication acquisition costs
- Audit triggers that scrutinize past billing patterns
- Cash flow disruption while resolving coding disputes
Conversely, accurate J code billing ensures timely reimbursement at appropriate rates, maintaining healthy revenue cycles. Many practices work with specialized medical billing services to ensure their J code submissions meet payer requirements consistently.
| Common Specialty | Typical J Code Volume | Primary Drug Types |
|---|---|---|
| Oncology | Very High | Chemotherapy agents, immunotherapy |
| Rheumatology | High | Biologics, disease-modifying drugs |
| Ophthalmology | Moderate | Anti-VEGF injections, antibiotics |
| Pain Management | Moderate to High | Nerve blocks, trigger point injections |
How to Find and Verify the Correct J Code
Identifying the appropriate J code requires methodical research and cross-referencing. Healthcare providers cannot simply guess or approximate these codes, as precision is mandatory for both compliance and reimbursement.
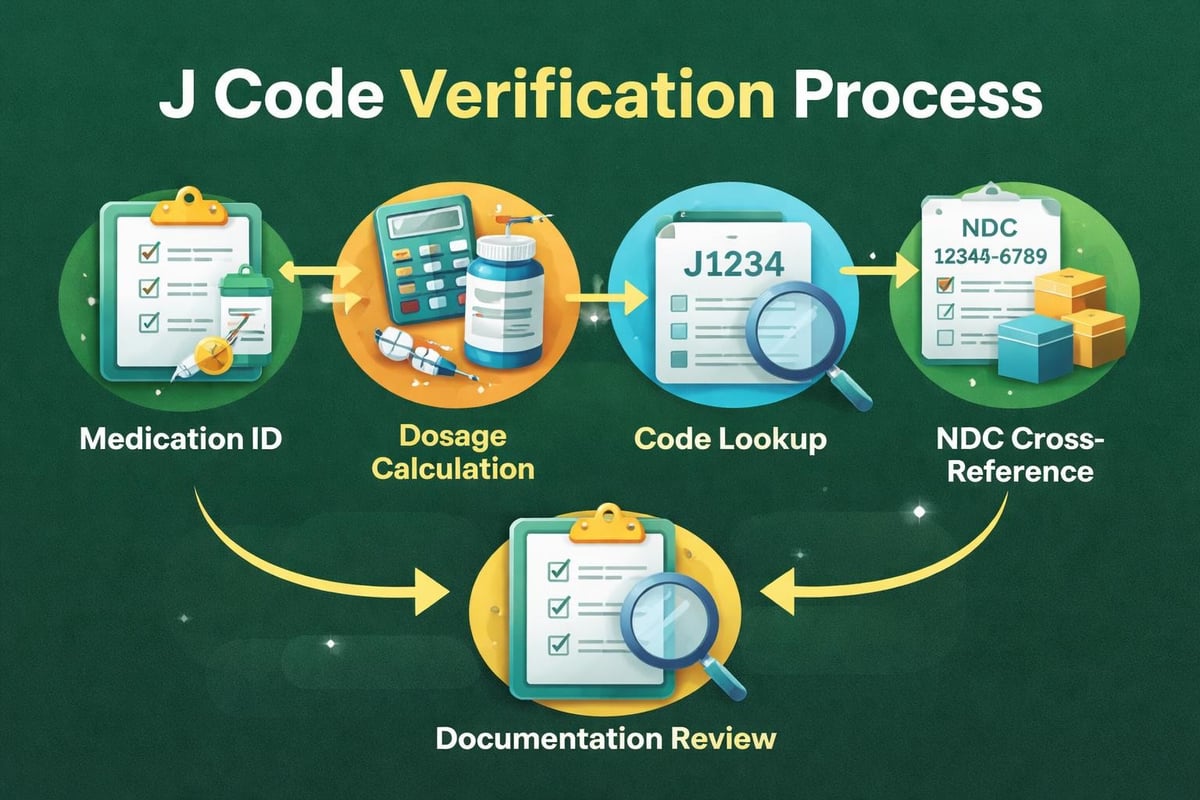
Step-by-Step J Code Identification Process
Step 1: Identify the exact medication administered, including brand name and generic chemical name.
Step 2: Determine the total dosage amount given to the patient during the encounter.
Step 3: Consult the current HCPCS Level II codebook or online database for the corresponding J code.
Step 4: Verify the code’s dosage unit matches your administered amount, calculating multiple units if necessary.
Step 5: Cross-reference with the National Drug Code (NDC) to ensure medication and code alignment.
Resources from specialty coding professionals provide detailed guidance on navigating complex pharmaceutical coding scenarios.
Many revenue cycle management teams maintain internal databases that map frequently administered medications to their corresponding J codes. This reference system reduces lookup time and minimizes coding errors during high-volume periods.
Common J Code Documentation Requirements
Proper documentation supports every J code claim. Payers expect medical records to include specific details that justify the medication administration:
- Complete medication name and strength
- Precise dosage amount administered
- Administration route and method
- Medical necessity justification
- Time and date of administration
- Ordering provider information
Without comprehensive documentation, even correctly coded claims may face denials during payer audits. Effective denial management services often track J code denials separately to identify systemic documentation gaps.
Common J Code Billing Challenges
Healthcare practices encounter recurring obstacles when managing j codes in medical billing. Recognizing these challenges allows organizations to implement preventive measures before problems escalate.
Dosage Calculation Errors
One of the most frequent mistakes involves miscalculating billable units. Since J codes represent specific quantities, providers must convert the administered dose into the appropriate number of units. For instance, if a J code represents 10 mg and the patient receives 35 mg, the provider should bill 3.5 units (or follow payer-specific rounding guidelines).
Common calculation pitfalls include:
- Failing to account for medication wastage policies
- Misreading concentration versus total volume
- Ignoring payer-specific rounding rules
- Incorrectly converting between measurement units
Many practices implement double-check protocols where both clinical and billing staff verify dosage calculations before claim submission.
Code Updates and Discontinued Medications
The pharmaceutical landscape changes constantly, with new medications entering the market and older drugs becoming obsolete. Understanding what CPT codes are for insurance helps contextualize how frequently coding systems evolve.
CMS releases quarterly updates that can add, delete, or modify J codes. Practices that fail to monitor these changes may continue billing discontinued codes or miss opportunities to use newly established identifiers. Subscription to official CMS listservs and participation in professional coding organizations helps teams stay current.
Payer-Specific J Code Requirements
Different insurance companies maintain unique policies regarding J code billing. While Medicare sets baseline standards, commercial payers often implement additional requirements:
- Prior authorization for specific high-cost medications
- Preferred drug lists that limit covered J codes
- Medical necessity documentation beyond standard requirements
- Alternative billing methods for certain drug categories
Revenue cycle teams must maintain payer-specific billing guidelines and update them regularly as contracts and policies change.
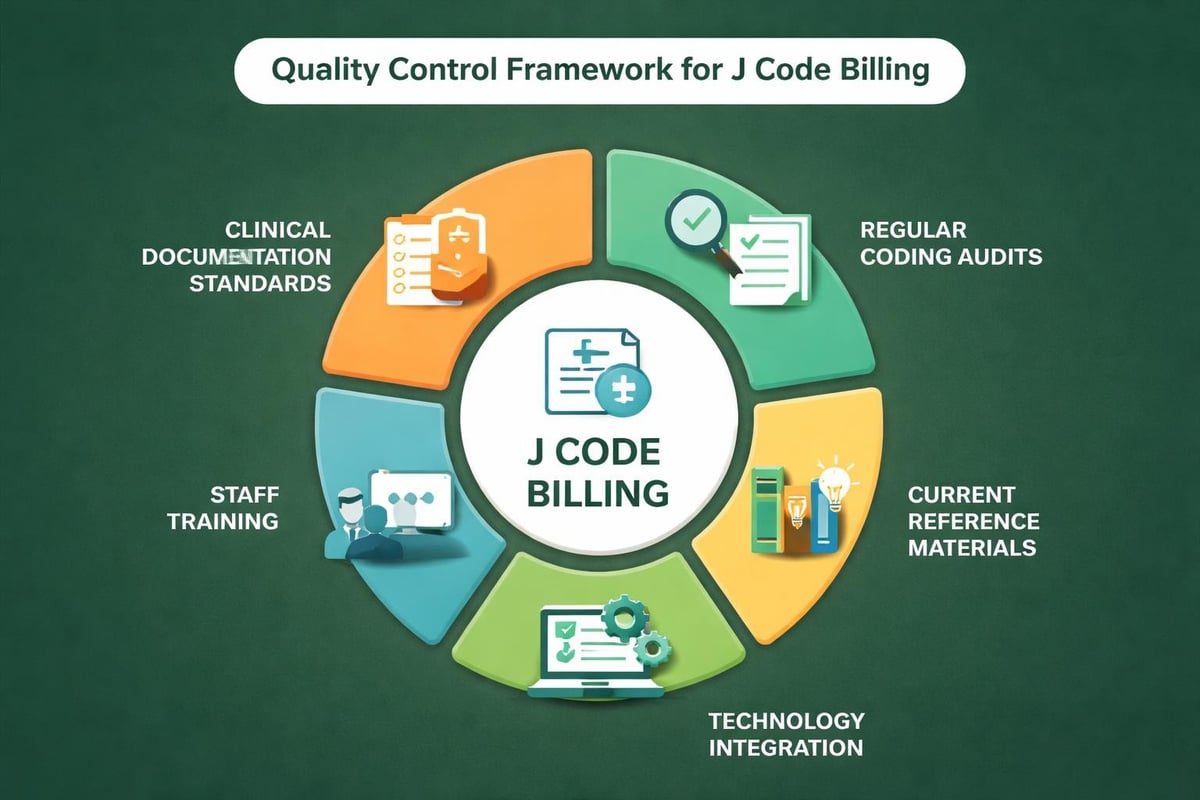
Best Practices for J Code Management
Successful j codes in medical billing implementation requires systematic processes that span clinical, administrative, and financial departments. Organizations that excel in this area typically embed quality controls throughout their revenue cycle.
Establish Clear Clinical Documentation Standards
Clinicians must understand that their documentation directly impacts billing accuracy. Standardized templates for medication administration should prompt providers to record all necessary details in consistent formats. Medical coding services often work with practices to develop documentation tools that satisfy both clinical and billing requirements.
Electronic health record (EHR) systems can include smart fields that automatically capture required J code information, reducing manual data entry and associated errors.
Implement Regular Coding Audits
Periodic internal audits identify coding patterns and potential compliance risks before they trigger external scrutiny. Effective audit programs examine:
- J code selection accuracy against medication records
- Dosage calculation correctness and unit billing
- Documentation completeness and medical necessity support
- Modifier usage when required for specific scenarios
- NDC reporting compliance where mandated
Medical coding audit services provide objective assessment of coding practices and highlight improvement opportunities.
Maintain Current Reference Materials
Coding accuracy depends on access to updated resources. Practices should invest in:
- Current year HCPCS Level II codebooks (updated annually)
- Quarterly update bulletins from CMS
- Payer-specific coverage policies and local coverage determinations
- Drug reference databases with J code cross-references
- Specialty-specific coding newsletters and publications
Many revenue cycle management professionals bookmark essential medical coding resources for quick reference during complex billing scenarios.
Training Staff on J Code Billing
Human expertise remains the cornerstone of accurate medical billing, regardless of technological advances. Comprehensive staff training programs ensure team members understand both the technical aspects of j codes in medical billing and the broader context of revenue cycle management.
Core Competencies for Billing Staff
Billing professionals handling J codes should demonstrate proficiency in several key areas:
| Competency Area | Required Knowledge | Assessment Method |
|---|---|---|
| Code Structure | J code format, dosage units, administration routes | Written exam, practical coding exercises |
| Drug Knowledge | Common medications, generic/brand names, therapeutic classes | Drug identification quizzes, case studies |
| Documentation | Required elements, medical necessity, compliance standards | Chart review assignments, audit participation |
| Payer Policies | Coverage rules, prior authorization, appeals processes | Policy interpretation tests, scenario practice |
Regular continuing education keeps staff current as pharmaceutical markets and coding guidelines evolve. Many organizations schedule quarterly training sessions coinciding with CMS update releases.
Cross-Department Collaboration
Effective J code billing requires coordination between clinical, pharmacy, and billing departments. Nurses and medical assistants who administer medications must understand how their documentation affects downstream billing processes. Pharmacists can provide valuable input on drug classifications and appropriate code selection.
Regular interdisciplinary meetings create opportunities to discuss recurring challenges, share updates, and align processes across departments. This collaborative approach reduces errors and improves overall revenue cycle performance.
Technology Solutions for J Code Management
While Greenhive Billing Solutions does not provide software products, the company’s experienced professionals utilize industry-standard technology platforms to optimize J code billing for clients. Understanding available technological solutions helps healthcare providers appreciate the tools that skilled revenue cycle management teams employ.
EHR Integration and Automated Code Suggestions
Modern electronic health record systems can integrate J code databases that suggest appropriate codes based on medication orders. When a provider documents medication administration, the system can automatically populate the corresponding J code, reducing manual lookup time and potential selection errors.
These integrations typically include:
- Real-time drug-to-code matching algorithms
- Dosage calculators that convert administered amounts to billable units
- Documentation prompts that ensure required elements are captured
- Alert systems that flag potential coding issues before claim submission
Revenue cycle management specialists configure these systems according to specialty-specific needs and payer requirements.
Claims Scrubbing Technology
Before claims reach payers, sophisticated scrubbing software examines J code submissions for common errors. These systems check for:
- Valid code formats and current code status
- Logical dosage amounts and unit calculations
- Required modifier presence when applicable
- NDC reporting compliance
- Documentation attachment completeness
Claim submission services leverage these technologies to maximize clean claim rates and accelerate reimbursement timelines.
Analytics and Reporting Tools
Data analytics platforms track J code utilization patterns, denial rates, and reimbursement trends. These insights help practices identify:
- High-denial J codes requiring process improvements
- Medications with consistently delayed payments
- Training needs based on error patterns
- Opportunities for prior authorization automation
- Payer-specific performance variations
Regular reporting keeps stakeholders informed about J code billing performance and guides strategic decisions about staff allocation, technology investments, and process refinements.
J Code Billing for Different Specialties
The application of j codes in medical billing varies significantly across medical specialties. Each practice area encounters unique challenges and opportunities related to pharmaceutical coding.
Oncology and Chemotherapy Administration
Oncology practices deal with some of the most complex and high-value J code scenarios. Chemotherapy regimens often involve multiple drugs administered during single encounters, each requiring separate J codes. These medications frequently cost thousands of dollars per dose, making coding accuracy financially critical.
Oncology billing teams must navigate:
- Buy-and-bill inventory management and wastage documentation
- Combination therapy coding with multiple J codes per encounter
- Clinical trial medications with special coding requirements
- Supportive care medications (anti-nausea, growth factors) billed separately
Many oncology practices partner with specialized revenue cycle management providers who understand the nuances of cancer treatment billing.
Rheumatology and Biologic Therapies
Rheumatology practices routinely administer expensive biologic medications for conditions like rheumatoid arthritis and psoriatic arthritis. These drugs require careful J code selection because similar medications may have different codes based on biosimilar status or specific formulations.
Key considerations for rheumatology J code billing:
- Prior authorization requirements for nearly all biologic agents
- Step therapy documentation showing less expensive alternatives were tried
- Administration method coding (infusion versus injection)
- Loading dose versus maintenance dose documentation
Ophthalmology and Intravitreal Injections
Ophthalmology practices frequently perform intravitreal injections for conditions like macular degeneration and diabetic retinopathy. These procedures involve both a J code for the medication (such as anti-VEGF agents) and a procedure code for the injection itself.
Common billing combinations include the J code for the drug plus CPT codes for the injection procedure. Understanding different types of modifiers becomes important when bilateral procedures are performed or multiple medications are administered.
Compliance Considerations for J Code Billing
Healthcare compliance extends beyond simple coding accuracy. Practices must ensure their J code billing practices align with federal regulations, payer contracts, and professional standards.
Medicare and Medicaid Requirements
Government payers maintain specific J code billing rules that differ from commercial insurance standards. Medicare requires NDC reporting for certain medications, while Medicaid programs vary by state regarding documentation and prior authorization.
Critical compliance elements include:
- Accurate reporting of drug acquisition costs for Average Sales Price calculations
- Proper use of KX modifiers when applicable for medical necessity exceptions
- Compliance with National Coverage Determinations and Local Coverage Determinations
- Timely filing within payer-specific deadlines
Anti-Kickback and Stark Law Implications
Practices must ensure their medication purchasing and administration arrangements don’t violate federal anti-kickback statutes or Stark Law prohibitions. This becomes particularly relevant when practices participate in specialty pharmacy arrangements or manufacturer discount programs.
Proper compliance programs include regular legal reviews of pharmaceutical vendor relationships and transparent documentation of all financial arrangements related to administered medications.
Documentation Retention Requirements
J code claims require extensive documentation that must be retained according to federal and state regulations. Most jurisdictions require minimum seven-year retention periods, though practices may maintain records longer to protect against potential audits.
Proper documentation systems should organize records to facilitate rapid retrieval during payer audits or compliance reviews. Many practices implement electronic document management systems that link medication administration records directly to submitted claims.
Optimizing Reimbursement Through Strategic J Code Management
Beyond basic accuracy, strategic approaches to j codes in medical billing can enhance overall reimbursement and practice profitability. Understanding how effective denial management improves cash flow demonstrates the financial impact of proactive coding strategies.
Negotiating Payer Contracts
Healthcare practices should review payer contracts specifically for medication reimbursement terms. Some contracts base J code reimbursement on percentage of Average Wholesale Price, while others use Average Sales Price plus percentage markup. Understanding these formulas helps practices negotiate more favorable terms during contract renewals.
Key negotiation points include:
- Reimbursement methodology (AWP versus ASP versus WAC)
- Percentage add-ons for acquisition cost coverage
- Bundling versus separate billing allowances
- Prior authorization timelines and exceptions
- Appeal rights for denied J code claims
Inventory Management and Financial Planning
Practices that maintain medication inventory must balance clinical needs against financial risk. High-cost medications represent significant capital investment, and coding errors that delay reimbursement can create cash flow challenges.
Effective inventory management systems track:
- Medication expiration dates to minimize waste
- Patient-specific ordering to reduce excess inventory
- Payer approval status before medication acquisition
- Reimbursement timelines by payer and medication type
- Wastage documentation requirements and billing opportunities
Appeals and Denial Resolution
Even well-coded J code claims sometimes face denials. Systematic appeal processes recover otherwise lost revenue and identify systemic issues requiring correction.
Successful appeal programs include:
| Appeal Stage | Key Activities | Timeline |
|---|---|---|
| Initial Review | Identify denial reason, gather documentation | 1-3 days |
| Payer Contact | Clarify denial rationale, determine requirements | 3-5 days |
| Documentation Assembly | Compile medical records, administration logs, medical necessity support | 5-10 days |
| Appeal Submission | Submit formal appeal with complete documentation package | Within payer deadline |
| Follow-up | Track appeal status, escalate if needed | Ongoing until resolution |
Specialized denial management services bring expertise in J code appeals, often achieving higher overturn rates than internal teams lacking pharmaceutical billing experience.
Mastering j codes in medical billing requires ongoing attention to regulatory updates, payer requirements, and clinical documentation practices. Healthcare providers who implement systematic processes, invest in staff training, and leverage experienced revenue cycle management support position themselves for optimal reimbursement and compliance. Greenhive Billing Solutions specializes in comprehensive revenue cycle management tailored for practices that regularly bill J codes, offering expertise in pharmaceutical coding, denial management, and payer negotiations. Our team of skilled professionals works within your existing systems to improve coding accuracy, accelerate reimbursement, and maximize revenue from administered medications.

