Hospital revenue cycle management represents one of the most critical operational functions for healthcare institutions today. From the moment a patient schedules an appointment to the final payment collection, every touchpoint impacts financial health and operational efficiency. Healthcare providers face mounting pressure to optimize their revenue cycles while managing complex regulatory requirements, evolving payer policies, and patient satisfaction expectations. Understanding how to implement effective hospital RCM strategies separates financially stable institutions from those struggling with cash flow challenges and mounting accounts receivable.
Understanding the Core Components of Hospital RCM
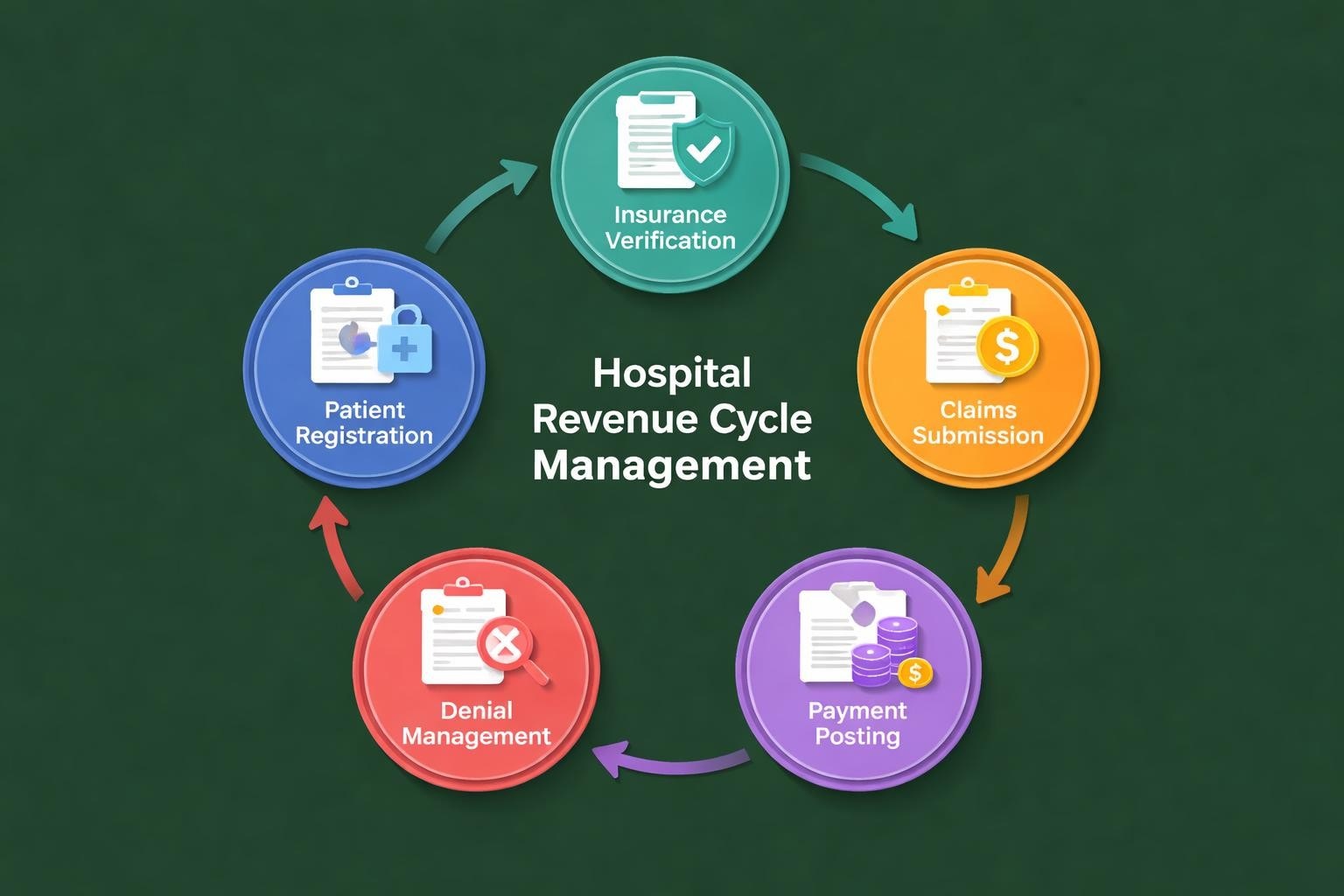
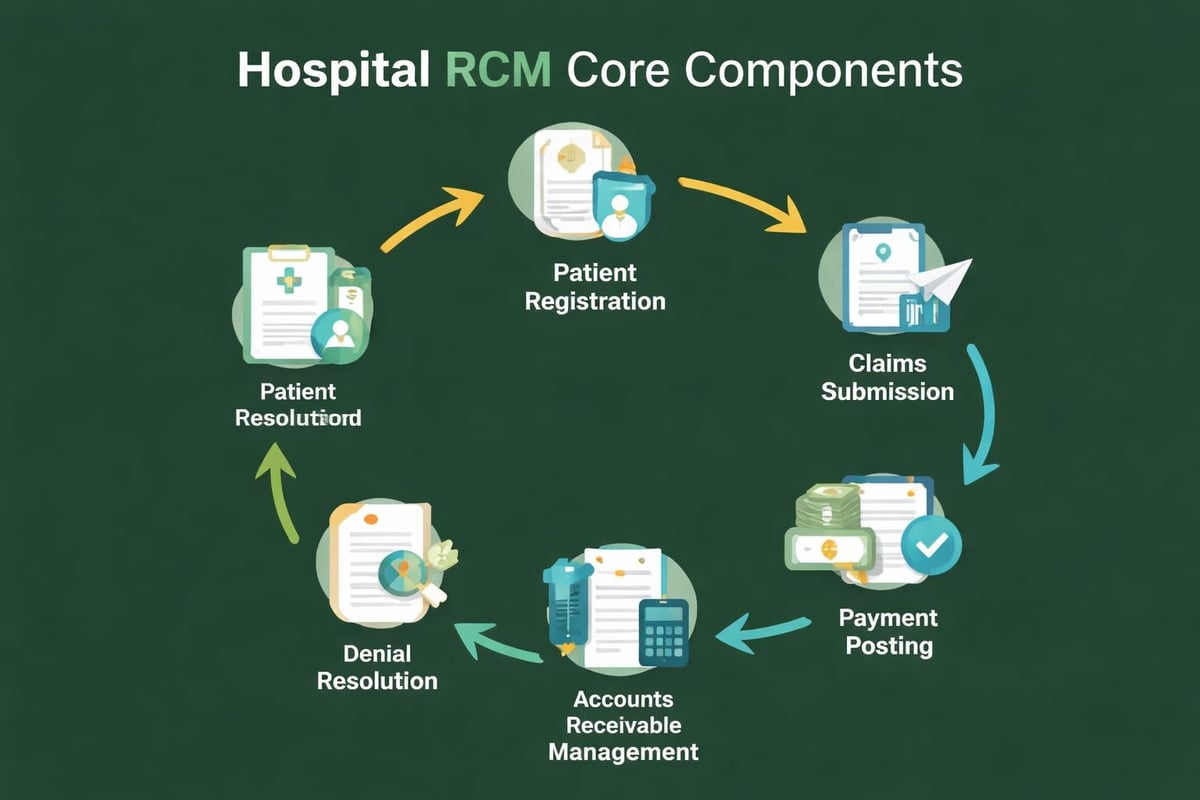
Hospital RCM encompasses the entire financial lifecycle of a patient encounter. This comprehensive process begins with patient access and extends through final payment reconciliation, touching every department within a healthcare facility.
The patient registration process establishes the foundation for successful revenue capture. Accurate demographic information, insurance details, and eligibility verification prevent downstream denials and payment delays. When registration staff collect complete and correct information upfront, they eliminate costly rework and reduce claim rejections.
Pre-Service Activities That Drive Revenue Success
Insurance verification and authorization represent critical pre-service functions. These activities confirm coverage, identify patient financial responsibility, and secure necessary approvals before services occur. Many healthcare providers streamline their eligibility verification processes to reduce claim denials and improve patient satisfaction.
Pre-registration systems allow hospitals to:
- Verify insurance eligibility in real-time
- Identify coverage limitations and exclusions
- Calculate patient financial responsibility accurately
- Secure pre-authorizations for planned procedures
- Collect upfront payments when appropriate
Financial counseling during pre-service activities improves collection rates and reduces bad debt. When patients understand their financial obligations before receiving care, they make informed decisions and arrange payment plans that work within their budgets.
Charge Capture and Clinical Documentation Excellence
Accurate charge capture directly impacts revenue integrity. Every service, procedure, medication, and supply must be documented and captured appropriately to ensure proper reimbursement. Hospitals lose significant revenue annually due to missed charges and inadequate documentation.
Clinical documentation improvement (CDI) programs bridge the gap between clinical care and accurate coding. CDI specialists work alongside physicians and clinical staff to ensure documentation supports the complexity and intensity of services provided. This collaboration produces more accurate diagnosis-related groups (DRGs) and higher case mix indices when clinically appropriate.
Technology's Role in Charge Capture
Modern charge capture systems integrate with electronic health records (EHRs) to automate routine charging processes. These integrations reduce manual data entry, minimize human error, and ensure charges flow seamlessly from clinical documentation to the billing system.
| Charge Capture Method | Accuracy Rate | Processing Time | Error Prevention |
|---|---|---|---|
| Manual Entry | 85-90% | 4-6 hours | Limited |
| Semi-Automated | 92-95% | 2-3 hours | Moderate |
| Fully Integrated | 97-99% | 30-60 minutes | Comprehensive |
Implementing automated charge capture mechanisms requires careful planning and ongoing monitoring. Regular charge audits identify patterns of missed charges, coding errors, and documentation deficiencies that require corrective action.
Claims Processing and Submission Best Practices
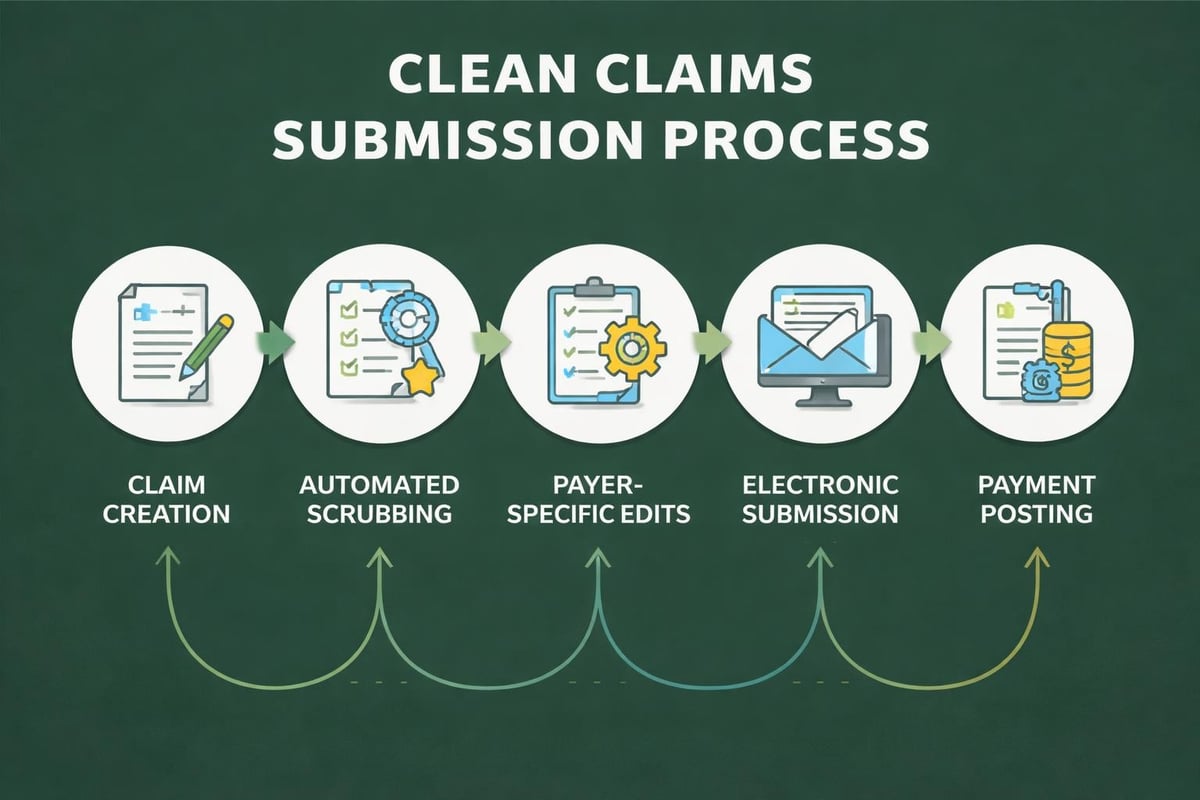
Clean claims submission represents the cornerstone of efficient hospital RCM. A clean claim contains all necessary information, follows payer-specific guidelines, and passes initial edits without requiring additional information or correction. Industry leaders achieve clean claim rates exceeding 95%, while struggling organizations may submit claims with 30-40% error rates.
Pre-submission claim scrubbing technology identifies potential errors before transmission to payers. These systems check for:
- Missing or invalid patient demographic information
- Incorrect or outdated insurance policy numbers
- Coding errors and missing modifiers
- Medical necessity documentation gaps
- Billing rule violations specific to each payer
Healthcare organizations implementing robust revenue cycle management strategies experience faster payment cycles and reduced administrative burden. The relationship between claim accuracy and days in accounts receivable remains undeniable.
Payer-Specific Requirements and Compliance
Each insurance company maintains unique billing requirements, coverage policies, and claim submission protocols. Hospital RCM teams must maintain current knowledge of these variations to prevent unnecessary denials. Many providers partner with specialized billing services that maintain expertise across multiple payer contracts and regulatory frameworks.
Understanding common denial management challenges helps organizations develop proactive prevention strategies. Rather than focusing solely on appealing denied claims, successful hospitals invest in root cause analysis and prevention.
Payment Posting and Reconciliation Processes
Timely and accurate payment posting provides essential visibility into revenue cycle performance. When payments arrive from insurance companies and patients, they must be applied correctly to outstanding accounts. This process requires careful attention to detail and thorough understanding of explanation of benefits (EOB) statements.
Payment posting staff must identify and address various scenarios including partial payments, denials, adjustments, and overpayments. Each transaction type requires specific handling to maintain accurate accounts receivable balances and identify trends requiring management attention.
Reconciliation activities ensure posted payments match bank deposits and payer remittance advices. Daily reconciliation prevents revenue leakage and identifies posting errors quickly. Organizations that delay reconciliation often discover significant discrepancies that prove difficult to resolve after time passes.
Electronic Remittance Advice Automation
Electronic remittance advice (ERA) files automate payment posting and reduce manual data entry. When hospitals receive ERA files from payers, specialized software can auto-post payments according to predefined business rules. This automation accelerates the posting process and improves accuracy.
However, automation requires careful setup and ongoing monitoring. Business rules must account for the nuances of different payer contracts, fee schedules, and adjustment reason codes. Regular audits of auto-posted payments ensure the system functions correctly and catches posting errors before they accumulate.
Denial Management and Appeals Strategy
Denials represent one of the most significant challenges in hospital RCM. Every denied claim requires additional resources to research, correct, and resubmit or appeal. The costs associated with denial management extend far beyond the claim value itself when considering labor, overhead, and delayed cash flow.
Effective denial management encompasses both prevention and resolution. Leading healthcare organizations invest heavily in understanding denial patterns and implementing targeted prevention initiatives. Prevention activities deliver substantially higher return on investment compared to appeals processing.
Common Denial Categories and Prevention Strategies
| Denial Category | Percentage of Total | Primary Prevention Strategy |
|---|---|---|
| Registration/Eligibility | 25-30% | Real-time verification systems |
| Authorization | 20-25% | Automated tracking and follow-up |
| Coding/Documentation | 20-25% | CDI programs and coder education |
| Timely Filing | 10-15% | Workflow management systems |
| Medical Necessity | 10-15% | Clinical decision support tools |
Building an effective appeals process requires detailed knowledge of payer-specific appeal procedures, documentation requirements, and filing deadlines. Many denials can be overturned through well-prepared appeals that include supporting clinical documentation and clear explanation of medical necessity.
Tracking denial metrics provides actionable intelligence for process improvement. Key performance indicators include denial rate by payer, denial reason code frequency, overturn rate by denial type, and time from denial to resolution.
Accounts Receivable Management and Collections
Managing accounts receivable requires disciplined follow-up processes and clear escalation protocols. Outstanding claims age rapidly, and collection probability decreases significantly after specific timeframes. Hospital RCM teams must prioritize aging accounts strategically to maximize cash collection.
Segmentation strategies divide accounts receivable into manageable categories based on payer type, account age, balance amount, and collection probability. This segmentation allows staff to focus efforts on accounts most likely to yield results.
Patient collections present unique challenges compared to insurance follow-up. Healthcare providers must balance aggressive collection practices with patient satisfaction and community relations. Many hospitals offer financial assistance programs, payment plans, and charity care options for patients experiencing financial hardship.

Technology Solutions for AR Management
Automated work queues distribute follow-up tasks to staff members based on workload balancing and specialization. These systems ensure no accounts fall through the cracks and provide management visibility into productivity and results.
Predictive analytics identify accounts requiring immediate attention and those unlikely to yield payment despite additional effort. Healthcare organizations using advanced analytics make data-driven decisions about resource allocation and collection strategy.
Performance Metrics and Continuous Improvement
Hospital RCM success requires measurement through key performance indicators that provide insight into operational efficiency and financial health. Organizations cannot improve what they do not measure, making robust reporting and analytics essential.
Critical metrics include:
- Days in accounts receivable measuring collection speed
- Clean claim rate indicating submission quality
- Denial rate showing prevention effectiveness
- Net collection rate revealing overall revenue capture
- Cost to collect demonstrating operational efficiency
- Point-of-service collections reflecting patient access performance
Benchmarking against industry standards helps organizations identify performance gaps and improvement opportunities. Resources from healthcare finance organizations provide valuable comparison data across facility types and sizes.
Building a Culture of Financial Accountability
Successful hospital RCM extends beyond the business office to engage clinical and operational staff throughout the organization. When physicians, nurses, and ancillary departments understand their role in revenue cycle success, they modify behaviors that impact financial performance.
Regular education sessions keep all stakeholders informed about documentation requirements, coding updates, and payer policy changes. Creating feedback loops between clinical and revenue cycle teams fosters collaboration and continuous improvement.
Regulatory Compliance and Risk Management
Hospital RCM operations must navigate complex regulatory requirements including HIPAA privacy and security rules, Medicare conditions of participation, state-specific billing regulations, and anti-kickback statutes. Non-compliance carries severe penalties including fines, exclusion from government programs, and reputational damage.
Compliance programs should address:
- Regular staff training on billing regulations and fraud prevention
- Internal audits of coding accuracy and billing practices
- Monitoring of government program participation requirements
- Documentation standards ensuring medical necessity support
- Third-party vendor compliance when outsourcing functions
Risk management activities identify vulnerabilities in revenue cycle processes before they result in compliance violations or financial losses. Regular internal audits, external compliance reviews, and participation in industry associations keep organizations informed of emerging risks and best practices.
Understanding common billing errors and prevention strategies helps hospital RCM teams avoid costly mistakes. Proactive compliance efforts cost far less than remediation after violations occur.
Outsourcing Considerations for Hospital RCM Functions
Many healthcare organizations partner with specialized revenue cycle management service providers to improve performance and reduce costs. These partnerships allow hospitals to access expertise, technology, and best practices without significant capital investment. When evaluating potential partners, hospitals should assess experience with similar facility types, technology capabilities, compliance track records, and cultural fit.
Outsourcing models range from comprehensive end-to-end management to focused solutions addressing specific challenges. Common outsourced functions include medical coding, denial management, patient access services, and back-end collections. Organizations must carefully define scope, performance expectations, and transition plans when engaging external partners.
Successful outsourcing relationships require clear communication, defined metrics, and regular performance reviews. Service level agreements should specify turnaround times, quality standards, and reporting requirements. Transparency in operations and financial results builds trust and enables continuous improvement.
Staff Training and Professional Development
Investment in revenue cycle staff development directly impacts hospital RCM performance. The complexity of billing regulations, payer policies, and technology systems requires ongoing education and skill development. Organizations with comprehensive training programs experience lower turnover, higher productivity, and better financial results.
Professional certifications validate expertise in specialized areas including medical coding, revenue cycle management, and compliance. Encouraging staff to pursue certifications through organizations like AAPC and HFMA demonstrates commitment to professional excellence.
Cross-training initiatives build organizational resilience by ensuring critical functions can continue despite staff absences. When multiple team members understand each role within the revenue cycle, they collaborate more effectively and identify process improvement opportunities.
Addressing the top challenges in healthcare revenue cycle operations requires skilled professionals who adapt to changing requirements. Retention strategies that emphasize career development, competitive compensation, and work-life balance protect organizational knowledge and reduce costly turnover.
Technology Integration and System Optimization
Modern hospital RCM relies heavily on integrated technology systems that automate routine tasks and provide decision support. Electronic health records, practice management systems, clearinghouses, and analytics platforms must work together seamlessly to support efficient operations.
System integration challenges arise when multiple vendors provide different components of the technology infrastructure. Data must flow accurately between systems without manual intervention, duplicate entry, or information loss. Interface monitoring and testing ensure reliability and data integrity.
Organizations implementing new systems or upgrading existing technology should follow structured methodologies including requirements definition, vendor selection, configuration, testing, training, and go-live support. Inadequate planning and rushed implementations often result in workflow disruptions and user frustration that persist long after launch.
Optimizing hospital RCM requires strategic focus, operational discipline, and continuous improvement across all revenue cycle functions. Healthcare organizations that master these principles achieve superior financial performance while maintaining high-quality patient care and satisfaction. Greenhive Billing Solutions partners with healthcare providers to enhance revenue cycle efficiency through comprehensive services including medical billing, claims processing, denial management, and insurance verification, all delivered with transparent communication and HIPAA compliance to maximize reimbursements and improve financial outcomes.