Healthcare providers face mounting pressure to maintain financial stability while delivering exceptional patient care. The path to sustainable revenue requires more than basic billing practices. It demands a revenue cycle pro approach that integrates strategic planning, operational excellence, and continuous improvement across every touchpoint in the financial workflow. Organizations that elevate their revenue cycle management capabilities position themselves for long-term success in an increasingly complex reimbursement landscape.
Understanding the Revenue Cycle Pro Framework
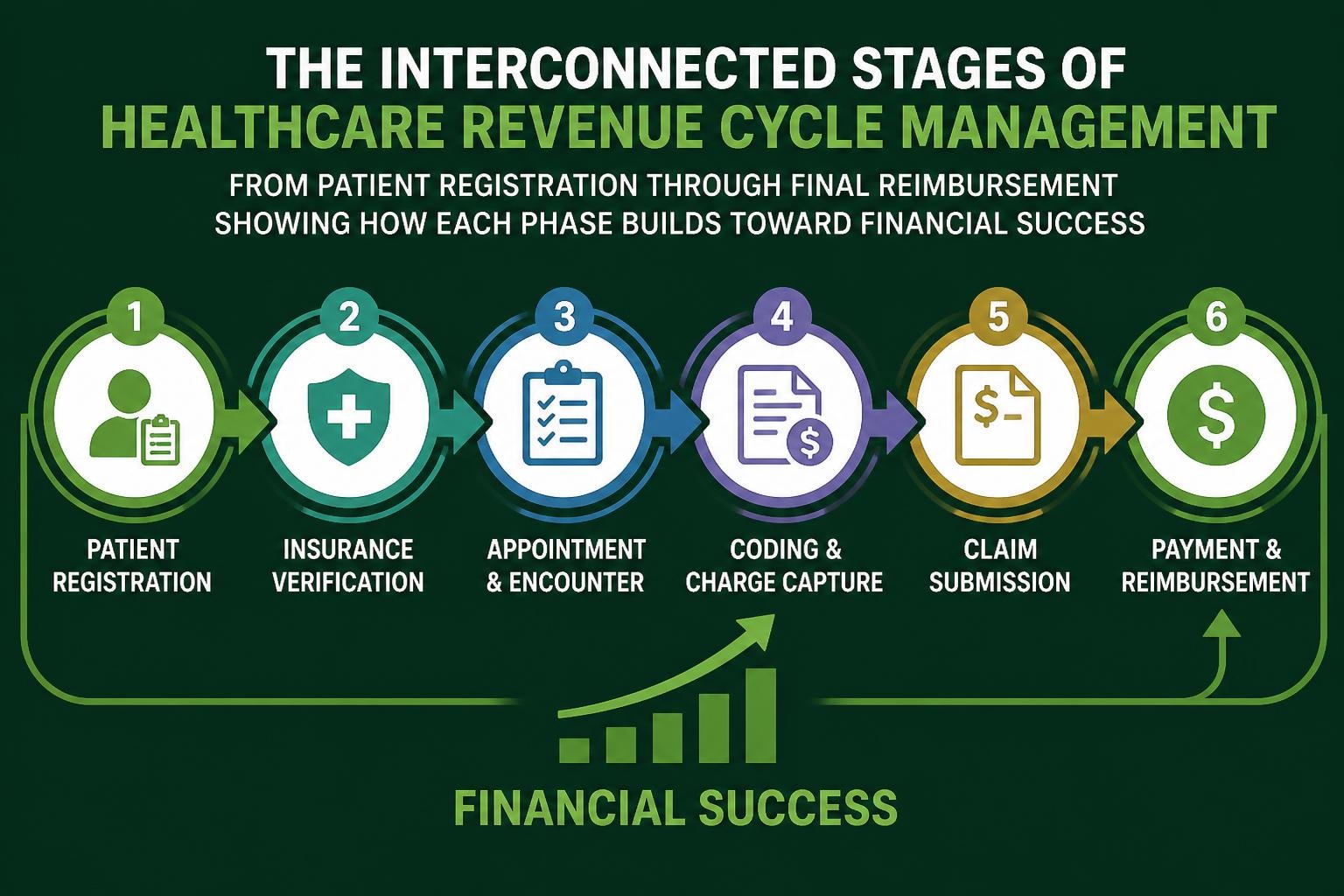
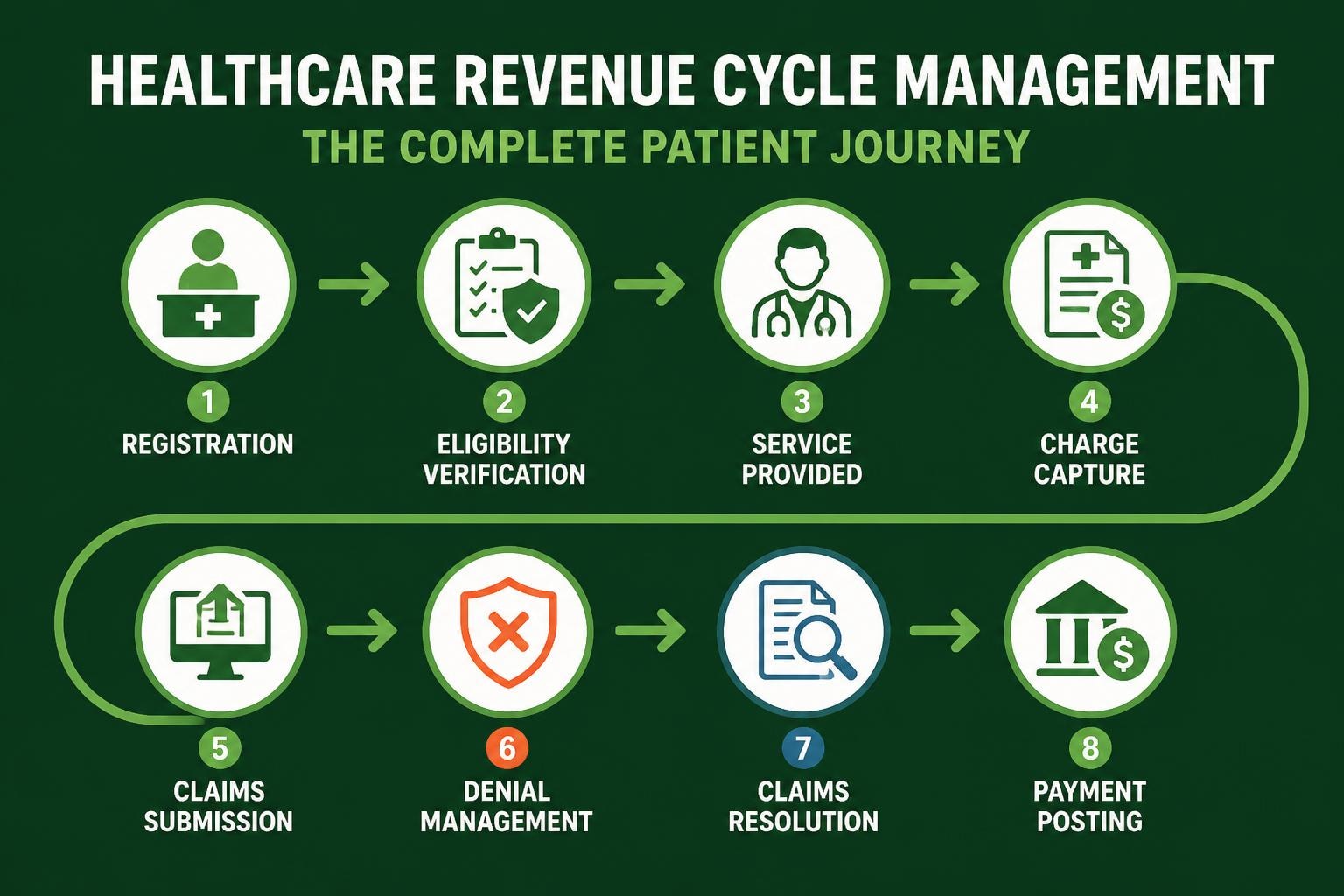
A revenue cycle pro operates with a comprehensive understanding of how each process component impacts overall financial performance. This framework extends beyond simple transaction processing to encompass strategic oversight, data-driven decision-making, and proactive problem-solving. The distinction between basic billing operations and professional revenue cycle management lies in the depth of expertise, systematic approach, and commitment to measurable outcomes.
Healthcare organizations implementing a revenue cycle pro methodology focus on three critical pillars: accuracy, efficiency, and optimization. Each pillar supports the others, creating a robust system that minimizes revenue leakage and maximizes reimbursement. When practices adopt these principles, they experience fewer claim denials, shorter collection cycles, and improved cash flow.
Core Competencies of Revenue Cycle Excellence
The revenue cycle pro approach requires mastery across multiple disciplines. Professionals in this field develop expertise in coding accuracy, payer requirements, regulatory compliance, and financial analytics. These competencies work together to create seamless operations.
| Competency Area | Impact on Revenue | Key Performance Indicator |
|---|---|---|
| Accurate Coding | Reduces denials by 30-40% | First-pass acceptance rate |
| Eligibility Verification | Prevents registration errors | Pre-service verification rate |
| Claims Submission | Accelerates payment cycles | Days in accounts receivable |
| Denial Management | Recovers lost revenue | Denial overturn percentage |
| Patient Communication | Improves collections | Patient payment collection rate |
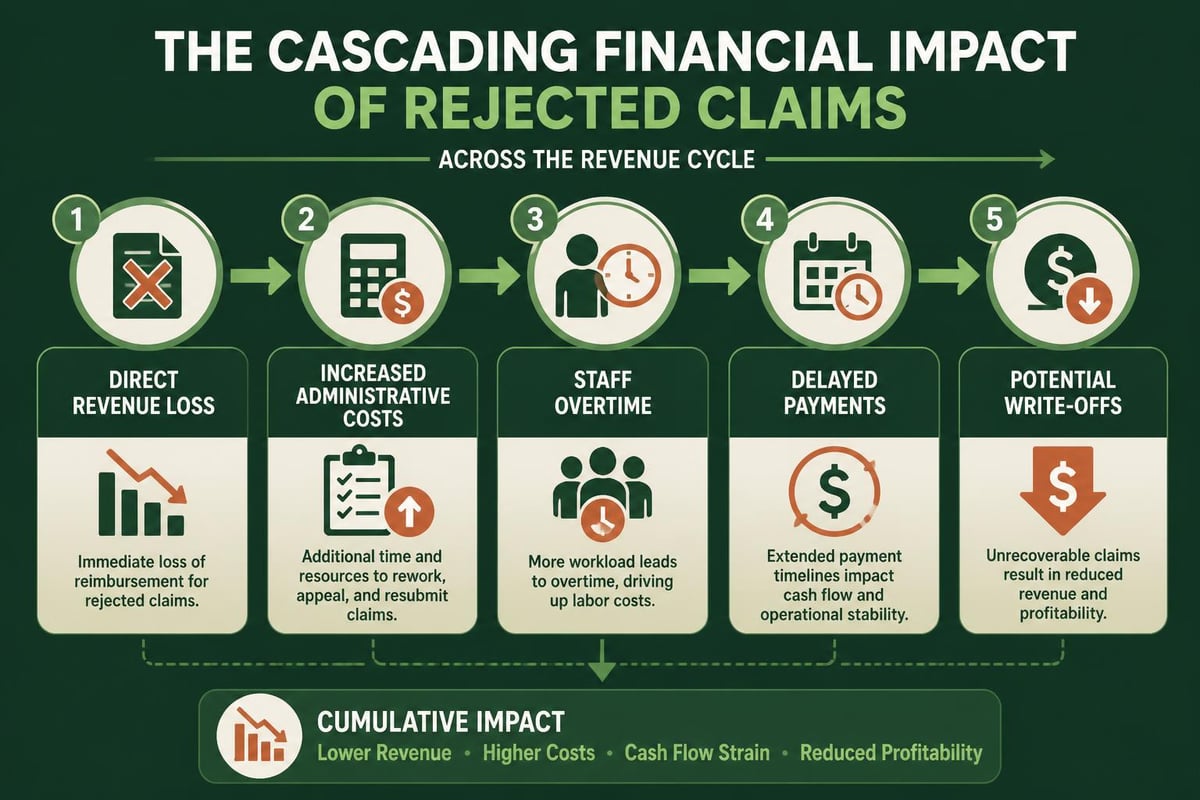
Organizations that implement comprehensive denial management services see dramatic improvements in their bottom line. The revenue cycle pro understands that prevention costs less than correction, making front-end accuracy a top priority.
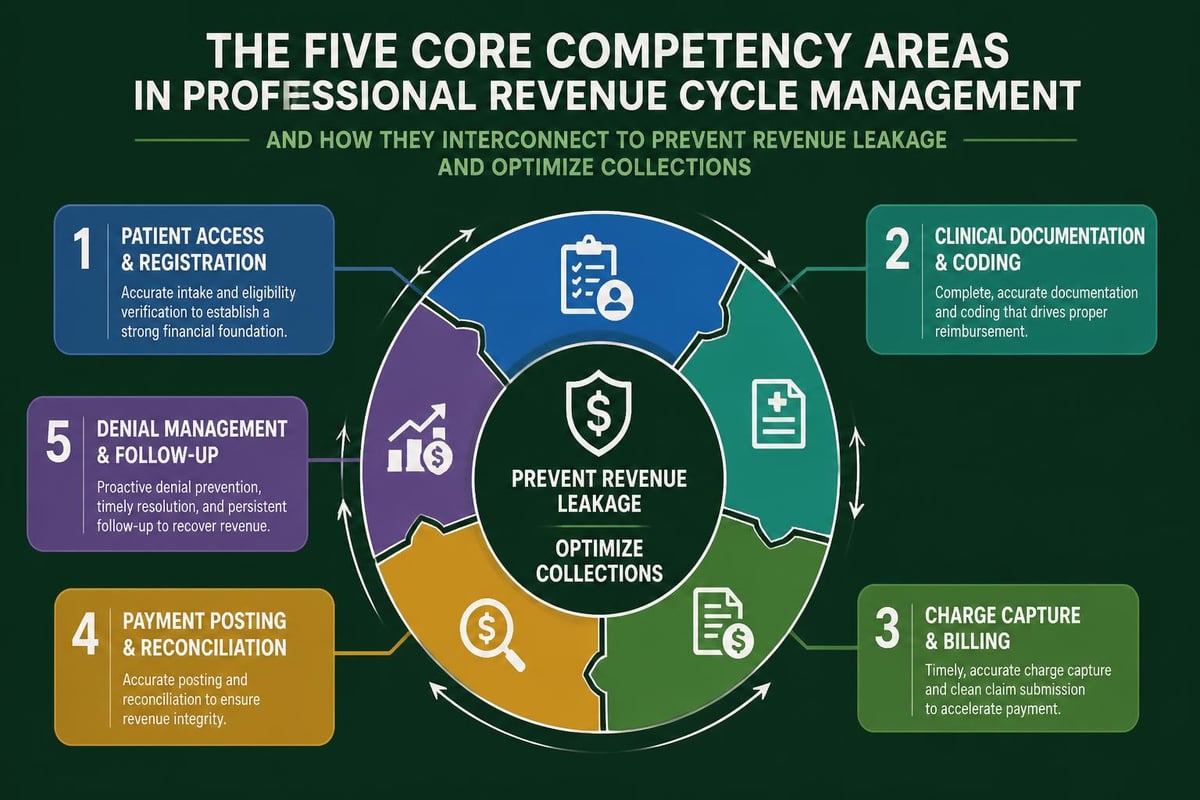
Strategic Patient Access and Registration
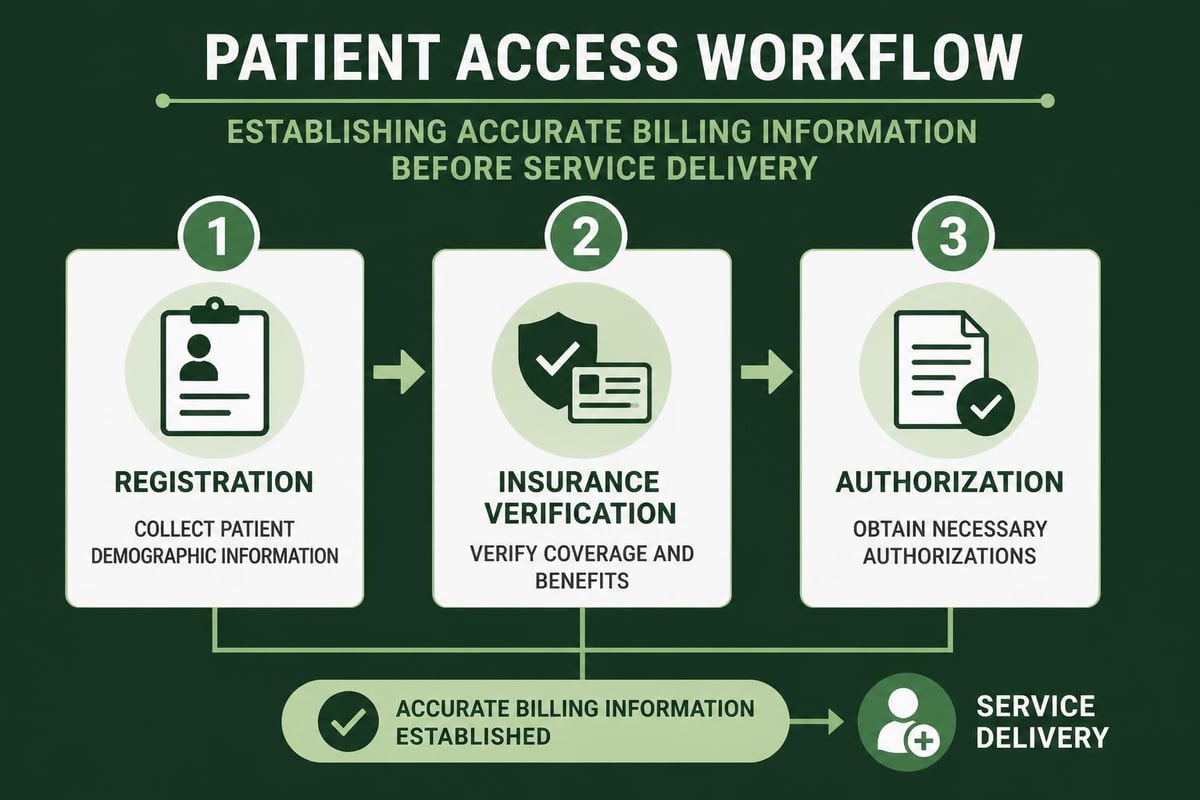
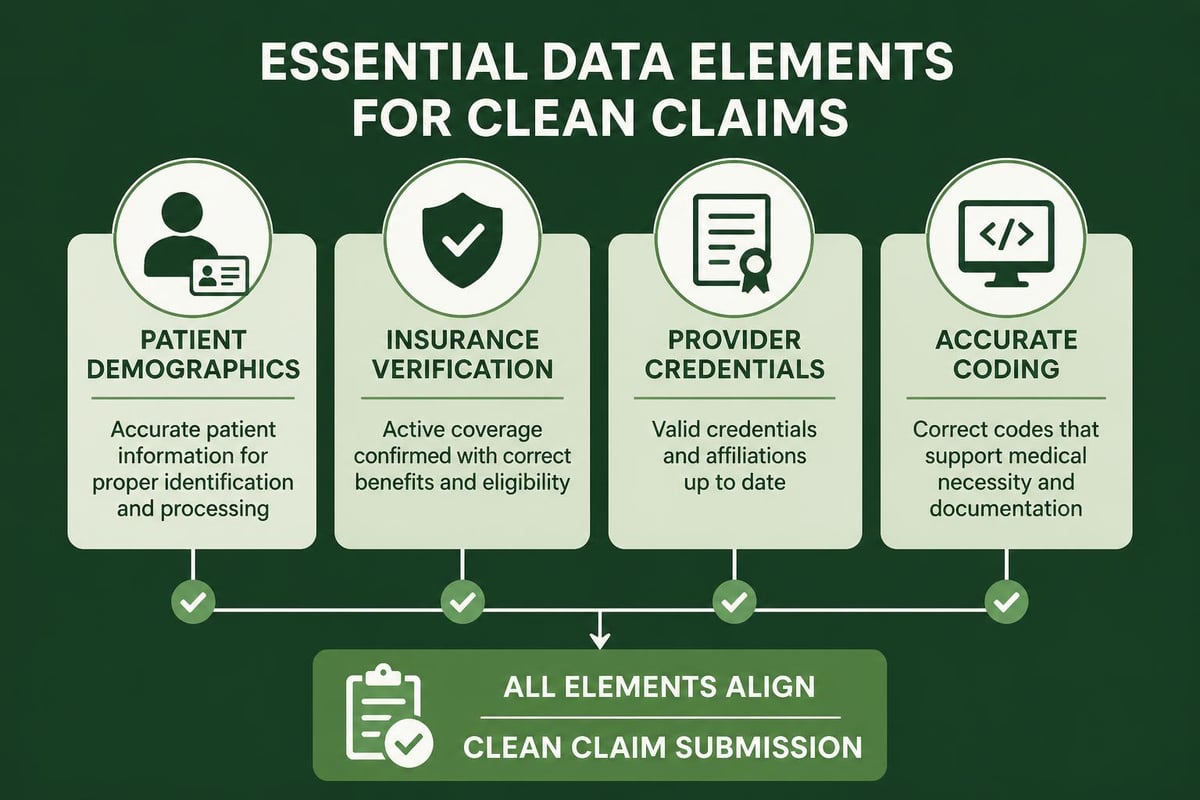
Patient access serves as the foundation for successful revenue cycle outcomes. A revenue cycle pro recognizes that errors introduced during registration cascade through every subsequent process, creating costly complications. Best practices for healthcare providers emphasize the critical importance of capturing accurate demographic and insurance information at first contact.
Five Essential Registration Practices
1. Real-Time Insurance Verification
Every patient encounter should begin with insurance eligibility verification before services are rendered. This practice prevents claim denials related to coverage issues and ensures patients understand their financial responsibility upfront.
2. Complete Demographic Accuracy
Patient name spelling, date of birth, address, and contact information must match insurance records exactly. Even minor discrepancies trigger automated claim rejections.
3. Authorization Management
Services requiring prior authorization demand systematic tracking and documentation. Revenue cycle pro teams implement automated alerts and follow-up protocols to prevent authorization-related denials.
4. Payment Policy Communication
Transparent discussion of payment expectations, copayments, and deductibles reduces confusion and improves patient satisfaction while accelerating collections.
5. Point-of-Service Collections
Collecting patient responsibility amounts at the time of service significantly reduces accounts receivable aging and improves overall collection rates.
Front-end revenue cycle processes directly influence financial outcomes. Organizations investing in robust patient access procedures experience cleaner claims, faster payments, and stronger cash flow throughout the year.
Professional Charge Capture and Coding
The revenue cycle pro approaches charge capture and medical coding with precision and attention to detail. This critical phase transforms clinical documentation into billable claims that accurately reflect the services provided. Understanding what is a CPT code for insurance in healthcare claims represents fundamental knowledge for any revenue cycle professional.
Coding accuracy depends on thorough clinical documentation. When physicians and clinical staff provide complete, specific notes, coders can assign appropriate procedure and diagnosis codes that support medical necessity and maximize legitimate reimbursement.
Optimizing the Coding Process
- Regular Education and Training: Keep coding staff updated on annual code changes, payer policy updates, and specialty-specific requirements
- Quality Assurance Audits: Implement routine internal audits to identify patterns, prevent compliance issues, and improve accuracy
- Documentation Improvement: Work collaboratively with providers to enhance clinical notes and support proper code assignment
- Technology Integration: Utilize computer-assisted coding tools and electronic health record integration to streamline workflows
Healthcare practices that prioritize medical coding services quality see measurable improvements in clean claim rates. The revenue cycle pro recognizes that investing in skilled coders and ongoing education pays dividends through reduced denials and optimized reimbursement.
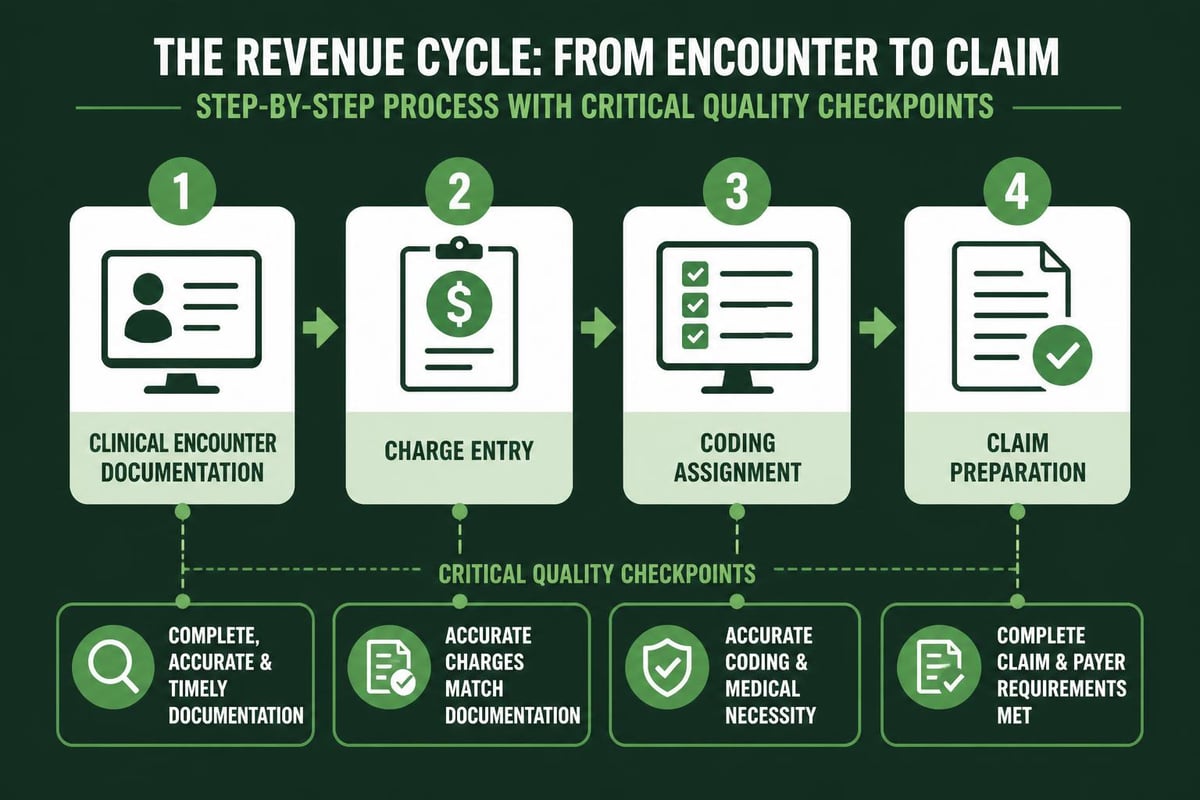
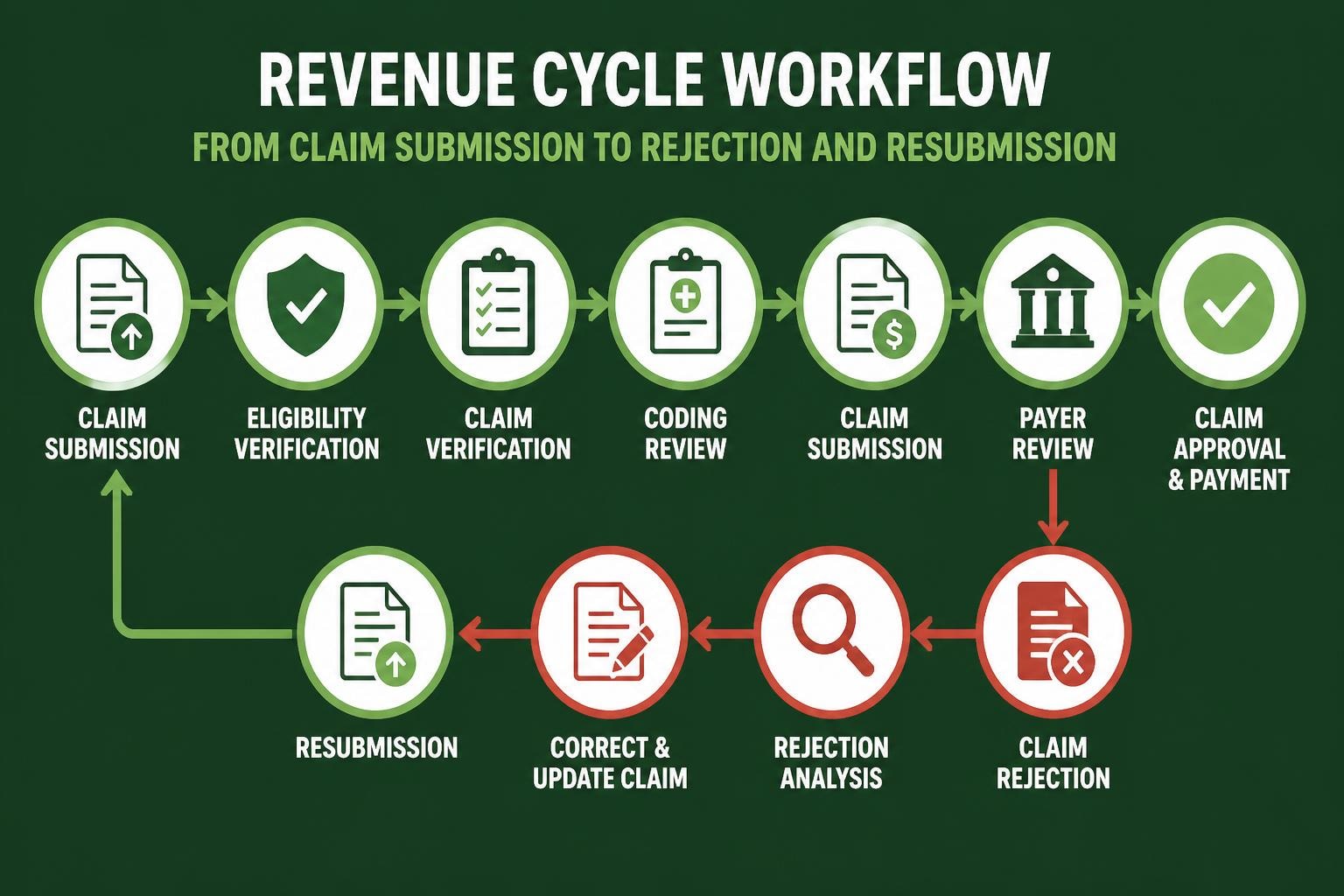
Claims Management and Submission Excellence
Professional claims management represents the moment when preparation meets execution. A revenue cycle pro ensures that every claim submitted meets payer requirements, contains complete information, and positions the practice for first-pass payment. Revenue cycle management best practices emphasize the importance of clean claim submission as a primary performance metric.
The transition from charge capture to claim submission requires systematic quality controls. Automated claim scrubbers identify common errors before transmission, but human oversight remains essential for complex cases and unusual circumstances.
| Claim Submission Element | Best Practice Standard | Common Pitfall |
|---|---|---|
| Demographic Information | 100% accuracy required | Transposed numbers, misspellings |
| Procedure Codes | Match documentation precisely | Unbundling, lack of medical necessity |
| Diagnosis Codes | Specific to highest level | Using unspecified codes when specific available |
| Modifiers | Applied per payer guidelines | Incorrect modifier 59 usage, missing bilateral modifiers |
| Authorization Numbers | Verified and included | Missing authorization, expired dates |
Organizations should leverage medical claim submission services that employ multiple verification layers. The revenue cycle pro knows that claims rejected at the front door cost significantly more to correct than claims accepted on first submission.
Reducing Common Submission Errors
Electronic claim submission has reduced processing time, but errors still occur. Understanding common mistakes with modifier 59 in medical billing helps prevent one of the most frequent submission problems. Revenue cycle pro teams implement systematic review processes that catch errors before transmission.
Payer-specific requirements add complexity to the submission process. A single practice may work with dozens of different insurance companies, each with unique billing rules and documentation requirements. Maintaining current knowledge of these variations demands dedicated resources and ongoing education.
Advanced Denial Management Strategies
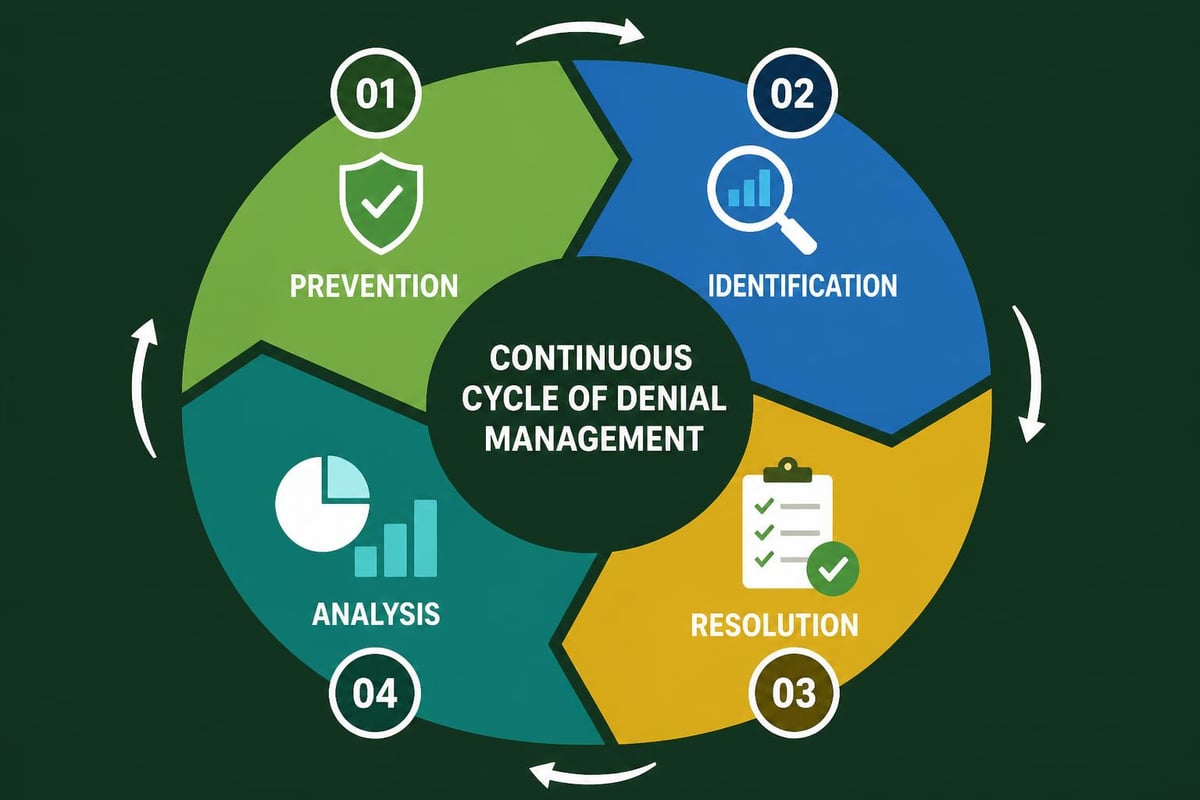
Even with perfect front-end processes, denials occur. The revenue cycle pro distinguishes between preventable denials and those resulting from legitimate coverage issues. Understanding how denial management in medical billing improves cash flow transforms this challenging aspect of revenue cycle management into an opportunity for process improvement.
Effective denial management operates on three levels: prevention, resolution, and analysis. Each level requires different skills and contributes uniquely to overall financial performance.
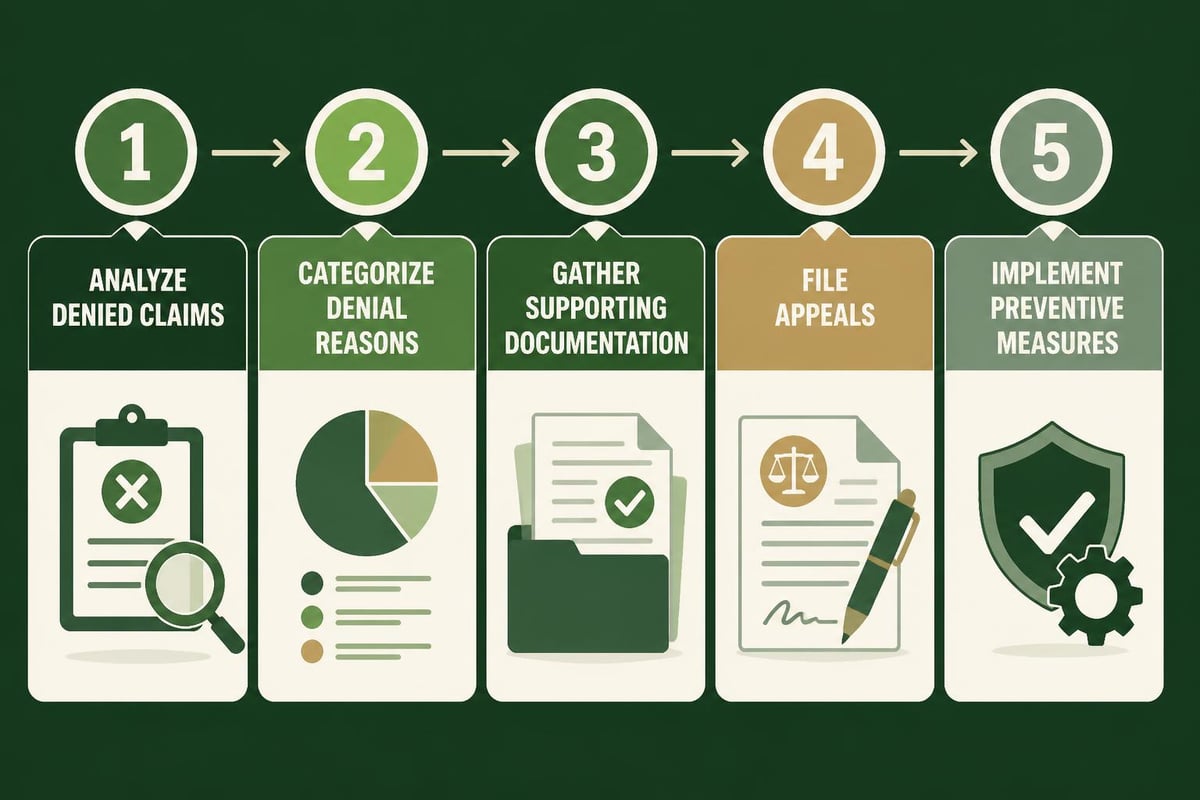
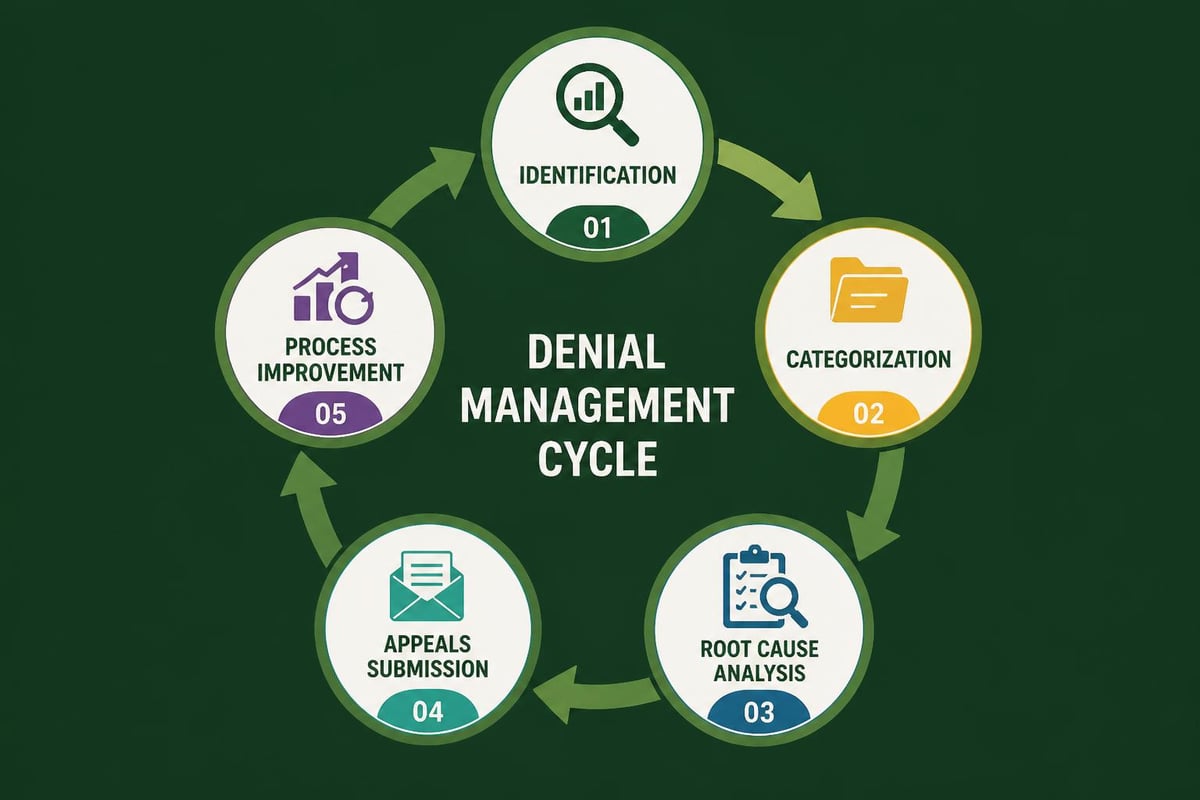
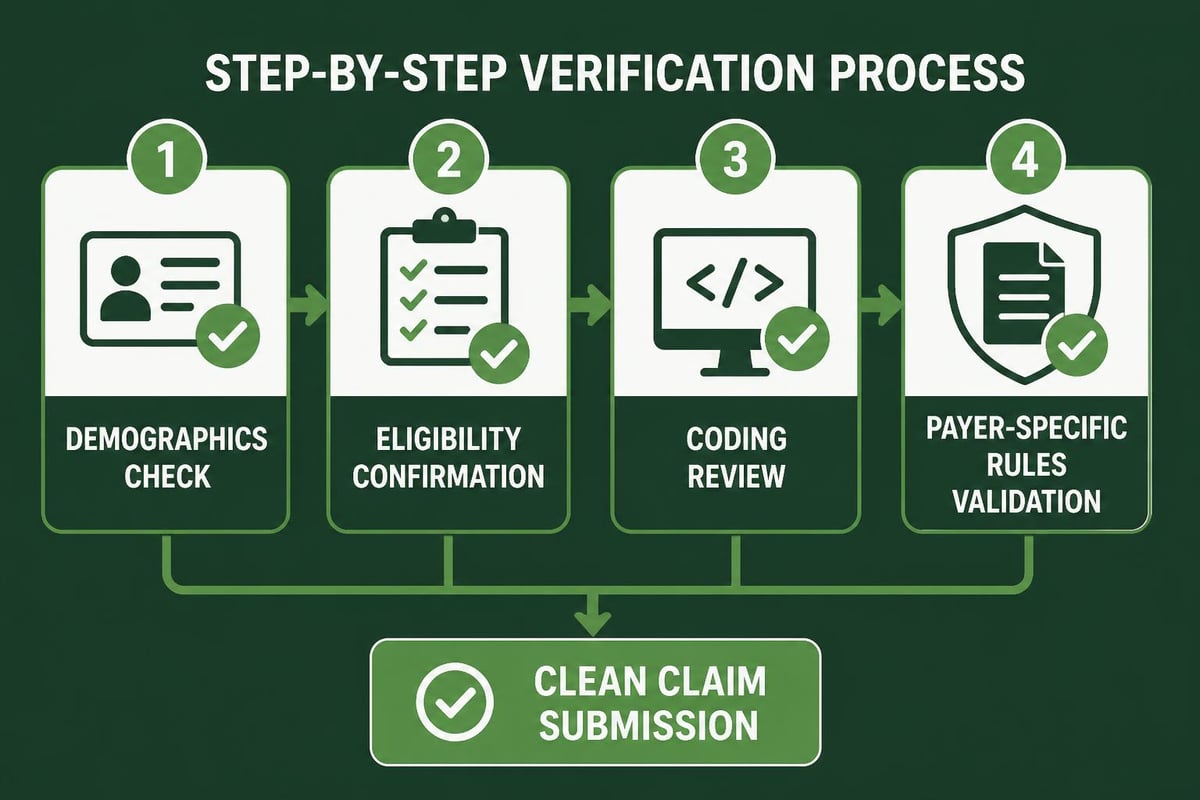
Step-by-Step Denial Resolution Process
Step 1: Immediate Identification and Categorization
Classify denials by reason code, payer, and service type within 24 hours of receipt. This rapid categorization enables prioritization based on revenue impact and resolution complexity.
Step 2: Root Cause Analysis
Investigate why the denial occurred. Was it a registration error, coding mistake, missing authorization, or payer policy issue? Understanding the source guides the correction approach.
Step 3: Timely Appeal Preparation
Gather supporting documentation, compose clear appeal letters citing specific policy language, and submit within payer-specified timeframes. Many practices lose thousands in revenue simply by missing appeal deadlines.
Step 4: Tracking and Follow-Up
Monitor appeal status systematically. Revenue cycle pro organizations maintain detailed logs showing appeal submission dates, payer response deadlines, and final outcomes.
Step 5: Pattern Recognition and Prevention
Analyze denial trends monthly to identify systemic issues. If a particular service, provider, or payer generates recurring denials, implement targeted corrections to prevent future occurrences.
The back-end revenue cycle processes often determine whether practices achieve their financial targets. Revenue cycle pro professionals dedicate substantial resources to denial management because successful appeals directly increase net collections.
Payment Posting and Reconciliation
Accurate payment posting ensures that accounts reflect true patient balances and practice financial reports contain reliable data. The revenue cycle pro approaches this task with the same rigor applied to claim submission. Payment posting services require attention to detail and understanding of complex explanation of benefits documents.
When insurance companies remit payment, they include detailed information about how they calculated reimbursement. Revenue cycle professionals must interpret these explanations, post payments correctly, and identify any discrepancies between expected and actual reimbursement. Understanding what are adjustments on medical bills helps explain why billed amounts differ from collected amounts.
Critical Payment Posting Elements
- Contractual Adjustments: Apply payer-specific contracted rates accurately to avoid patient billing errors
- Denial Posting: Route denied claims to appropriate work queues for timely follow-up
- Patient Responsibility: Calculate accurate patient balances after insurance payments
- Coordination of Benefits: Handle secondary and tertiary payer claims systematically
- Unapplied Payments: Research and resolve payments received without clear claim identification
Electronic remittance advice (ERA) has streamlined payment posting, but exceptions still require manual review. The revenue cycle pro ensures that automated posting rules align with payer contracts and that unusual payments receive appropriate scrutiny.
Accounts Receivable Management
Effective accounts receivable management separates high-performing practices from those struggling with cash flow challenges. A revenue cycle pro monitors aging reports closely, implementing strategies to accelerate collections while maintaining positive patient relationships. The goal is minimizing days in accounts receivable without compromising patient satisfaction.
| AR Category | Target Percentage | Action Required |
|---|---|---|
| 0-30 Days | 60-70% | Standard follow-up protocols |
| 31-60 Days | 15-20% | Intensive follow-up, patient outreach |
| 61-90 Days | 10-15% | Appeals, payment plans, collections consideration |
| 90+ Days | 5-10% | Aggressive collections, write-off evaluation |
Organizations maintaining these benchmarks demonstrate revenue cycle pro capabilities. They implement systematic follow-up protocols, leverage technology for automated workflows, and maintain adequate staffing for collections activities.
Optimizing Collections Processes
Patient collections present unique challenges compared to insurance follow-up. Revenue cycle pro teams balance assertive collection efforts with compassionate communication. Offering payment plans, providing clear billing statements, and maintaining multiple contact channels all contribute to improved patient collections.
Insurance follow-up requires different tactics. Revenue cycle professionals develop relationships with payer representatives, understand escalation procedures, and know when persistence yields results versus when appeals or other strategies prove more effective. Revenue cycle management challenges and best practices provide guidance for navigating complex collection scenarios.
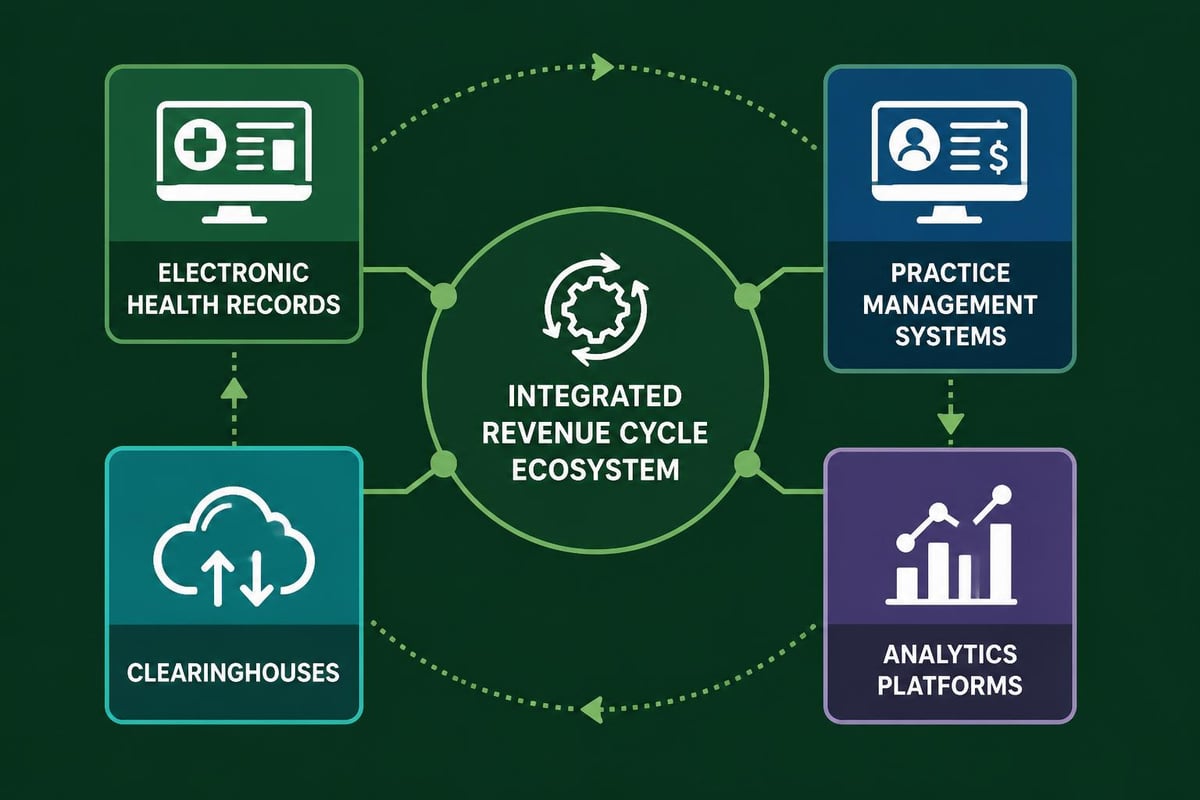
Technology and Analytics in Modern Revenue Cycle Management
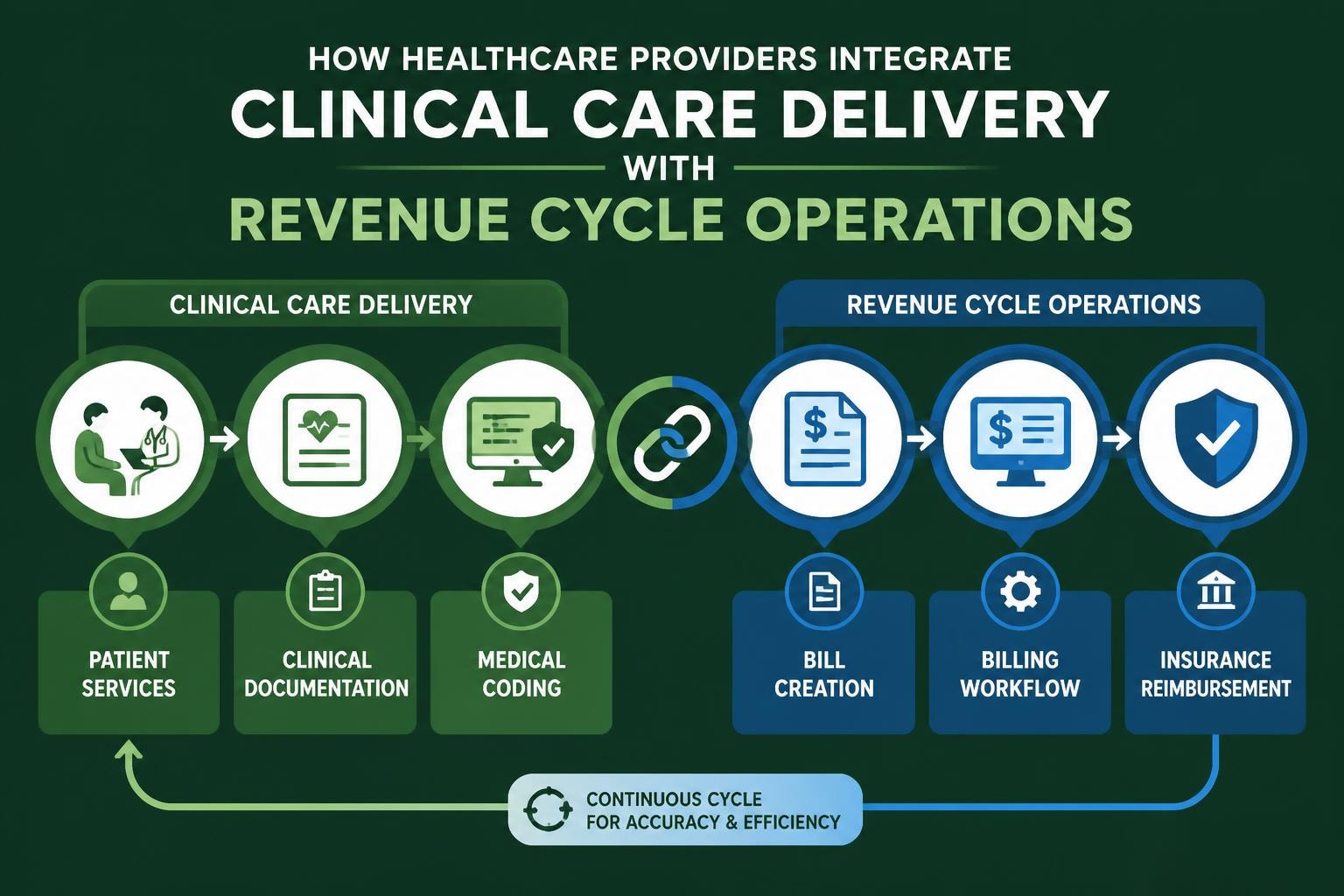
The revenue cycle pro leverages technology to enhance efficiency, accuracy, and insight. Practice management systems, electronic health records, clearinghouses, and specialized revenue cycle software create an integrated ecosystem that supports optimal financial performance. However, technology alone cannot solve revenue cycle challenges without skilled professionals who understand how to utilize these tools effectively.
Advanced analytics transform raw data into actionable intelligence. Revenue cycle pro organizations track key performance indicators daily, identify trends before they become problems, and make data-driven decisions about resource allocation and process improvements.
Essential Revenue Cycle Metrics
Clean Claim Rate: Percentage of claims accepted on first submission without errors or additional information requests. Target: 95% or higher.
Days in Accounts Receivable: Average number of days between service date and payment receipt. Target: 30-40 days for most specialties.
Collection Rate: Net collections divided by net charges after contractual adjustments. Target: 95-98%.
Denial Rate: Percentage of claims denied on first submission. Target: Less than 5%.
Point-of-Service Collection Rate: Percentage of patient responsibility collected at time of service. Target: 50% or higher.
Organizations serious about revenue cycle excellence implement reporting and analytics dashboards that provide real-time visibility into these metrics. The revenue cycle pro uses this information to guide continuous improvement initiatives.
Building a Revenue Cycle Pro Team
Revenue cycle excellence requires more than processes and technology. It demands skilled professionals who bring expertise, attention to detail, and commitment to continuous improvement. Whether building an internal team or partnering with specialized service providers, healthcare organizations must prioritize revenue cycle competency.
Staff training represents an ongoing investment rather than a one-time event. Annual coding updates, changing regulations, and evolving payer policies require continuous education. The revenue cycle pro commits to professional development through certifications, continuing education, and participation in industry organizations.
Selecting the Right Revenue Cycle Partner
Many healthcare providers choose to outsource revenue cycle functions to specialized organizations. This decision allows clinical staff to focus on patient care while revenue cycle professionals handle the complex financial operations. When evaluating potential partners, consider these factors:
- Industry Experience: Look for providers with demonstrated expertise in your specialty and familiarity with your specific challenges
- Technology Capabilities: Ensure the partner uses current systems and can integrate with your existing platforms
- Transparency: Request detailed reporting and regular performance reviews that show measurable results
- Compliance Standards: Verify HIPAA compliance, data security protocols, and adherence to industry regulations
- Scalability: Choose partners who can adjust to your practice growth and changing needs
Healthcare providers exploring options should review top medical billing companies to understand the range of services and specializations available in the market.
Compliance and Regulatory Considerations
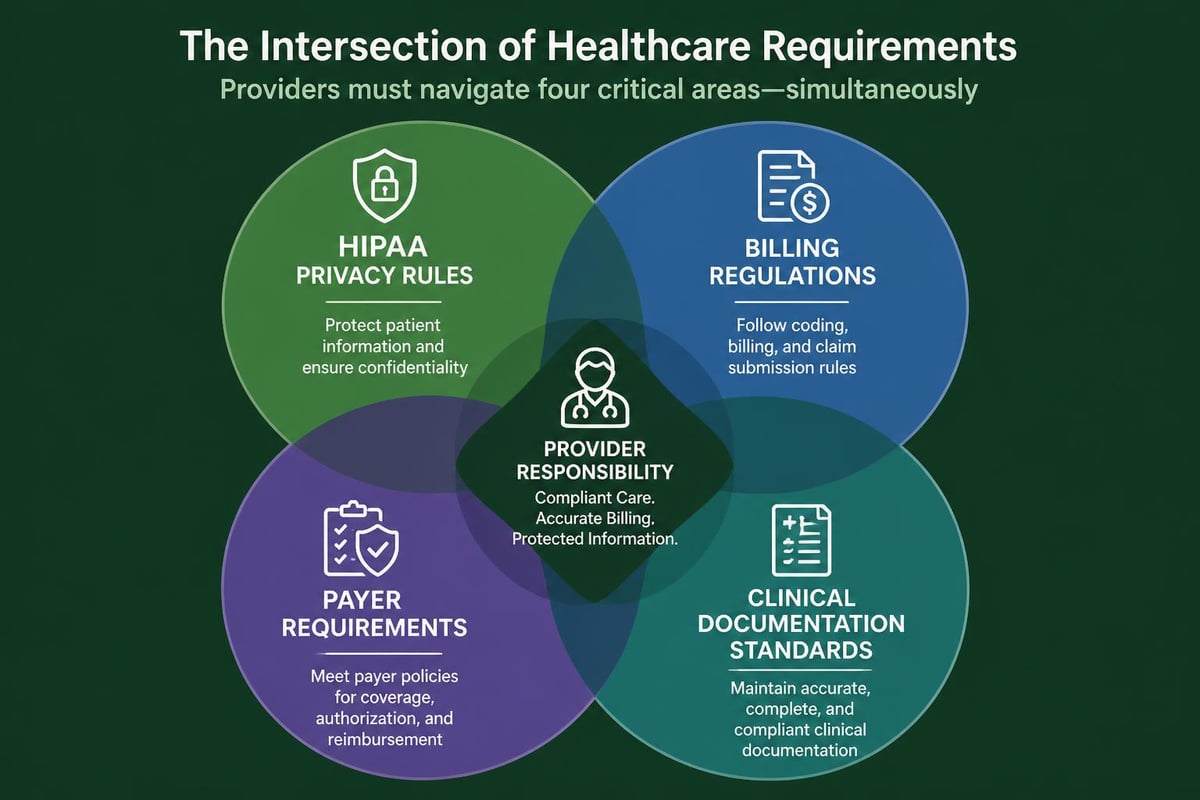
The revenue cycle pro maintains constant vigilance regarding compliance requirements. Federal regulations, state laws, and payer-specific policies create a complex regulatory environment that demands expertise and ongoing attention. Violations can result in substantial penalties, making compliance a critical component of revenue cycle management.
Understanding what revenue codes in medical billing represent and how they differ from procedure codes illustrates the complexity of billing requirements. Revenue cycle professionals must navigate these technical details while ensuring every claim meets regulatory standards.
HIPAA privacy and security rules govern how patient information is handled throughout the revenue cycle. From registration through final payment, every process must protect patient confidentiality while enabling necessary information exchange with payers and other authorized parties.
Specialty-Specific Revenue Cycle Considerations
Different medical specialties face unique revenue cycle challenges. A revenue cycle pro recognizes these variations and adapts strategies accordingly. High-volume primary care practices require different approaches than surgical specialties or diagnostic facilities.
Specialties requiring frequent authorizations, such as cardiology or oncology, benefit from prior authorization services that prevent treatment delays and payment denials. Each specialty has specific coding challenges, documentation requirements, and payer policies that influence revenue cycle performance.
Understanding the different types of medical coding helps practices appreciate the specialized knowledge required for accurate billing. Revenue cycle pro teams either develop deep specialty expertise or partner with organizations that possess the necessary knowledge.
Continuous Improvement and Innovation
Revenue cycle management is not static. Payer policies change, regulations evolve, and new technologies emerge. The revenue cycle pro embraces continuous improvement, regularly assessing performance and seeking opportunities for enhancement. This mindset separates organizations that maintain consistent financial performance from those that struggle with declining collections.
Benchmarking against industry standards provides context for performance evaluation. While every practice has unique characteristics, comparing key metrics to specialty-specific averages reveals improvement opportunities. Organizations should review their revenue cycle management processes quarterly to identify areas requiring attention.
Process documentation ensures consistency and facilitates training. When procedures exist only in individuals' heads rather than written protocols, organizations face vulnerability to staff turnover and inconsistent execution. The revenue cycle pro maintains comprehensive documentation that supports quality control and continuous improvement.
Innovation in revenue cycle management often comes from technology adoption, but also from creative problem-solving and process redesign. Organizations should encourage team members to suggest improvements and test new approaches in controlled environments before full implementation.
Mastering revenue cycle management requires expertise, systematic processes, and unwavering attention to detail across every phase of the financial workflow. Healthcare providers who elevate their revenue cycle capabilities through professional management practices position themselves for sustainable financial success. Greenhive Billing Solutions delivers comprehensive revenue cycle management services designed specifically for healthcare providers seeking to optimize their financial performance. Our team of experienced professionals handles every aspect of the revenue cycle, from eligibility verification through final payment, ensuring maximum reimbursements while maintaining full HIPAA compliance. Discover how Greenhive Billing Solutions can transform your practice's financial operations and free your staff to focus on exceptional patient care.