Healthcare providers face increasing pressure to control costs while maintaining quality patient care. Among the various payment models available, capitation represents a fundamental shift from traditional fee-for-service arrangements. Understanding how this payment structure functions within revenue cycle management can help practices make informed decisions about their financial strategies and operational approaches. As healthcare continues to evolve toward value-based care models, capitation plays an increasingly significant role in how providers receive reimbursement for their services.
Understanding Capitation Payment Models
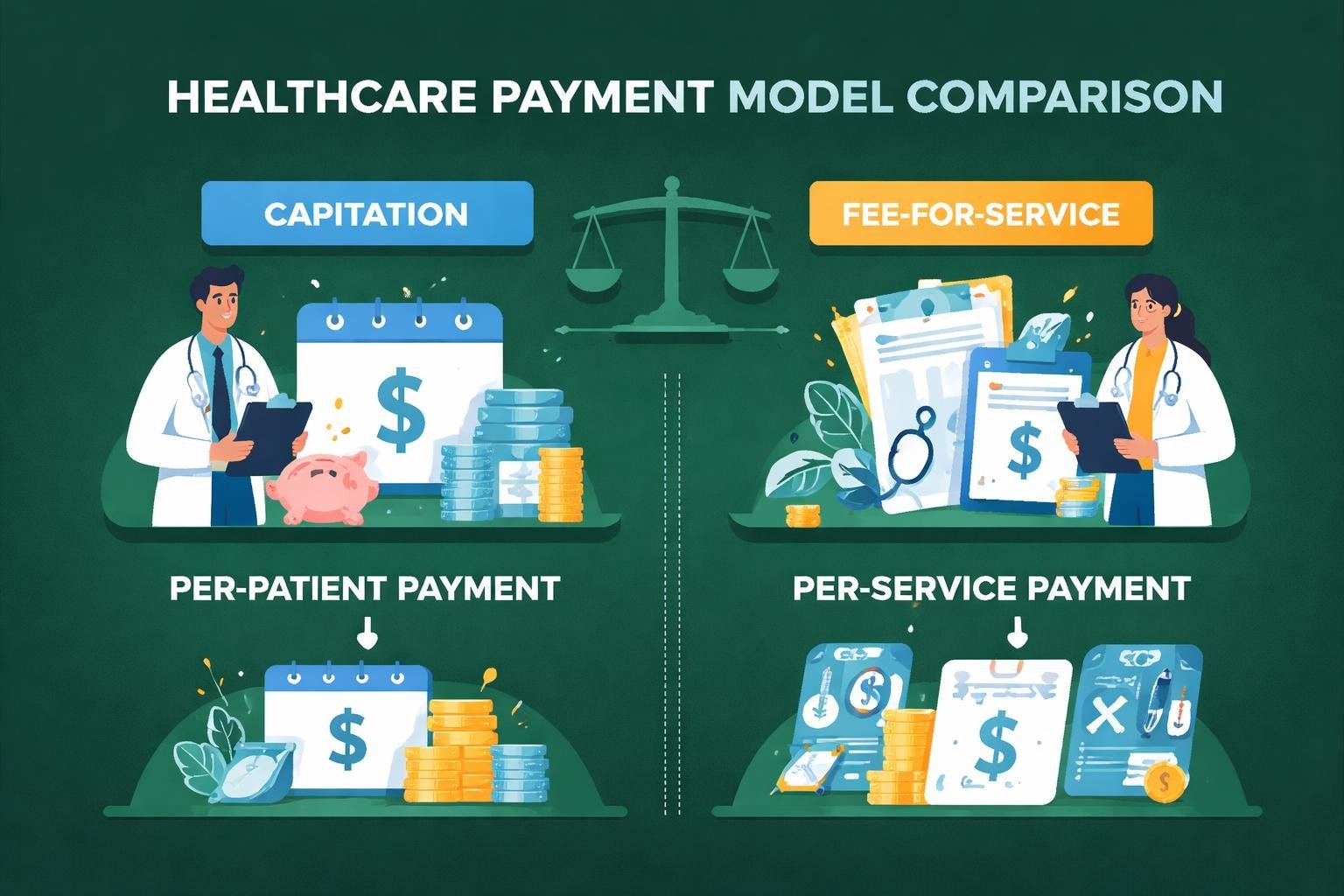
Capitation in medical billing operates on a predetermined, per-patient payment structure where healthcare providers receive a fixed amount for each enrolled individual, regardless of how many services that patient actually receives. This contrasts sharply with fee-for-service models where providers bill for each individual service, procedure, or visit. Capitation transfers financial risk from payers to providers, creating incentives to focus on preventive care and cost-effective treatment strategies.
The payment amount in capitation arrangements typically arrives monthly and gets calculated based on the number of patients assigned to a provider's panel. These rates factor in various elements including patient demographics, age groups, geographic location, and historical utilization patterns. Providers must deliver all agreed-upon services within the scope of the capitation agreement without additional compensation per service rendered.
How Capitation Payments Are Calculated
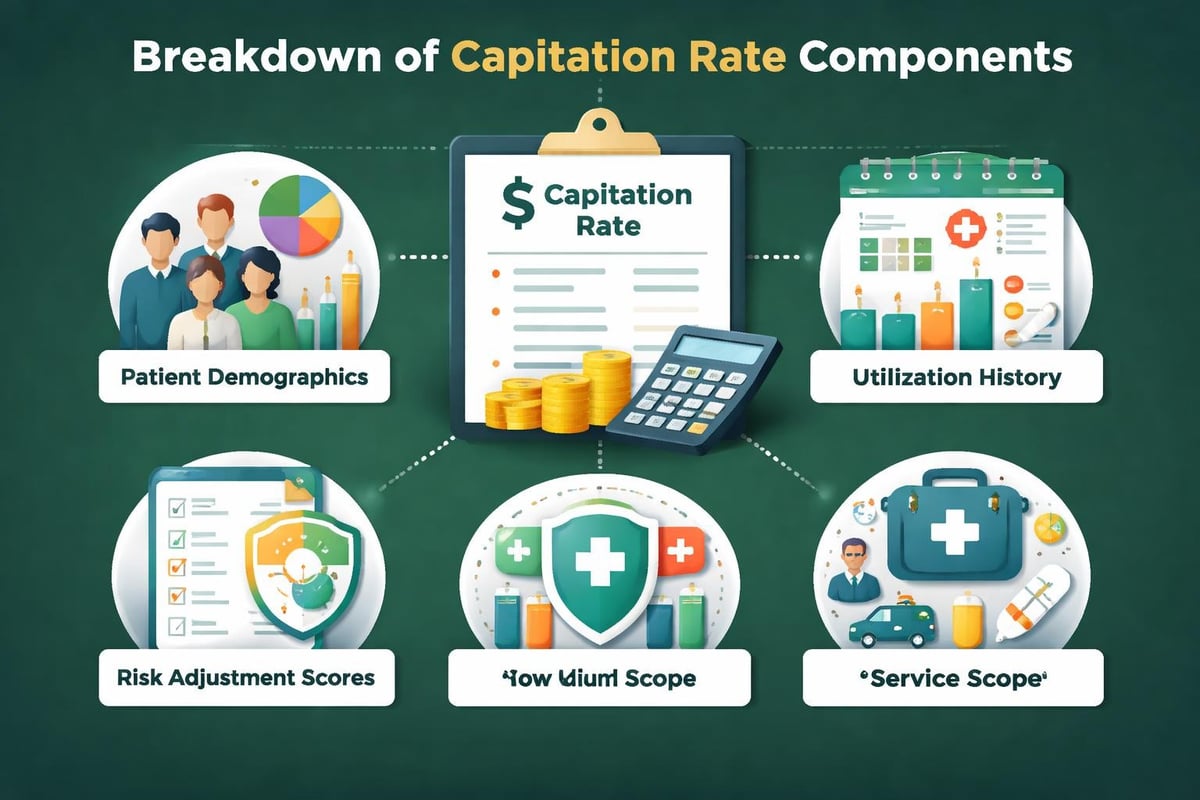
Healthcare organizations use several factors when determining capitation rates for different patient populations:
- Patient age and gender demographics
- Historical healthcare utilization data
- Geographic cost variations
- Scope of covered services
- Risk adjustment factors for chronic conditions
- Specialty care requirements
Insurance companies and managed care organizations analyze actuarial data to project expected healthcare costs for specific patient populations. They then set capitation rates that ideally cover anticipated expenses while building in margins for administrative costs and profit. Providers accepting capitation arrangements must carefully evaluate these rates against their own cost structures and patient population characteristics.
Types of Capitation Arrangements
Different capitation structures exist to accommodate various healthcare delivery scenarios and organizational relationships. Understanding these variations helps providers select appropriate arrangements for their practice models.
Primary Care Capitation
In primary care capitation, physicians receive fixed payments for providing comprehensive primary care services to assigned patients. This includes routine office visits, preventive care, basic diagnostic services, and care coordination. Primary care practices serve as gatekeepers, managing patient health while controlling referrals to specialists.
Specialty Care Capitation
Specialty providers may enter capitation contracts covering specific types of care within their expertise. Cardiologists, orthopedists, or other specialists receive predetermined payments for managing all care needs within their specialty for enrolled patients. This model requires careful consideration of patient acuity and expected service utilization.
Global Capitation
The most comprehensive form, global capitation encompasses all healthcare services including primary care, specialty services, hospital care, and ancillary services. Provider organizations assuming global capitation bear the greatest financial risk but also gain maximum control over care delivery and resource allocation.
| Capitation Type | Services Covered | Risk Level | Typical Users |
|---|---|---|---|
| Primary Care | Basic office visits, preventive care, coordination | Moderate | Family practices, internists |
| Specialty | Specific specialty services only | Moderate-High | Cardiologists, orthopedists |
| Global | All healthcare services across continuum | Very High | Large health systems, ACOs |
| Partial | Limited service categories | Low-Moderate | Group practices, IPAs |
Benefits of Capitation in Medical Billing
Healthcare providers implementing capitation arrangements can realize several strategic advantages that extend beyond simple payment mechanics. These benefits align with broader healthcare industry trends toward value-based care and population health management.
Revenue Predictability and Cash Flow Stability
Capitation provides consistent, predictable monthly revenue streams independent of patient visit volumes. This financial stability enables better budgeting, resource planning, and investment in infrastructure improvements. Practices can forecast revenue with greater accuracy and reduce administrative burden associated with individual claim submissions.
Incentives for Preventive Care
Since providers receive the same payment regardless of service volume, capitation in medical billing naturally encourages preventive care strategies. Keeping patients healthy reduces costly interventions and improves population health outcomes. Providers can invest in wellness programs, patient education, and chronic disease management without concern about billable services.
Reduced Administrative Burden
Capitation arrangements dramatically decrease the number of individual claims requiring submission, processing, and follow-up. Rather than billing for each service, providers receive predetermined payments, freeing staff resources for patient care activities. This administrative efficiency can offset some financial risks associated with the payment model.
Enhanced Care Coordination
Capitated payment structures motivate providers to coordinate care effectively across the healthcare continuum. Better communication between primary care providers and specialists, proactive discharge planning, and comprehensive care management all contribute to improved outcomes and controlled costs.
Challenges and Risks in Capitation Models
While capitation offers benefits, healthcare providers must carefully consider potential challenges before entering these arrangements. Understanding these risks enables better contract negotiation and operational planning.
Financial Risk Exposure
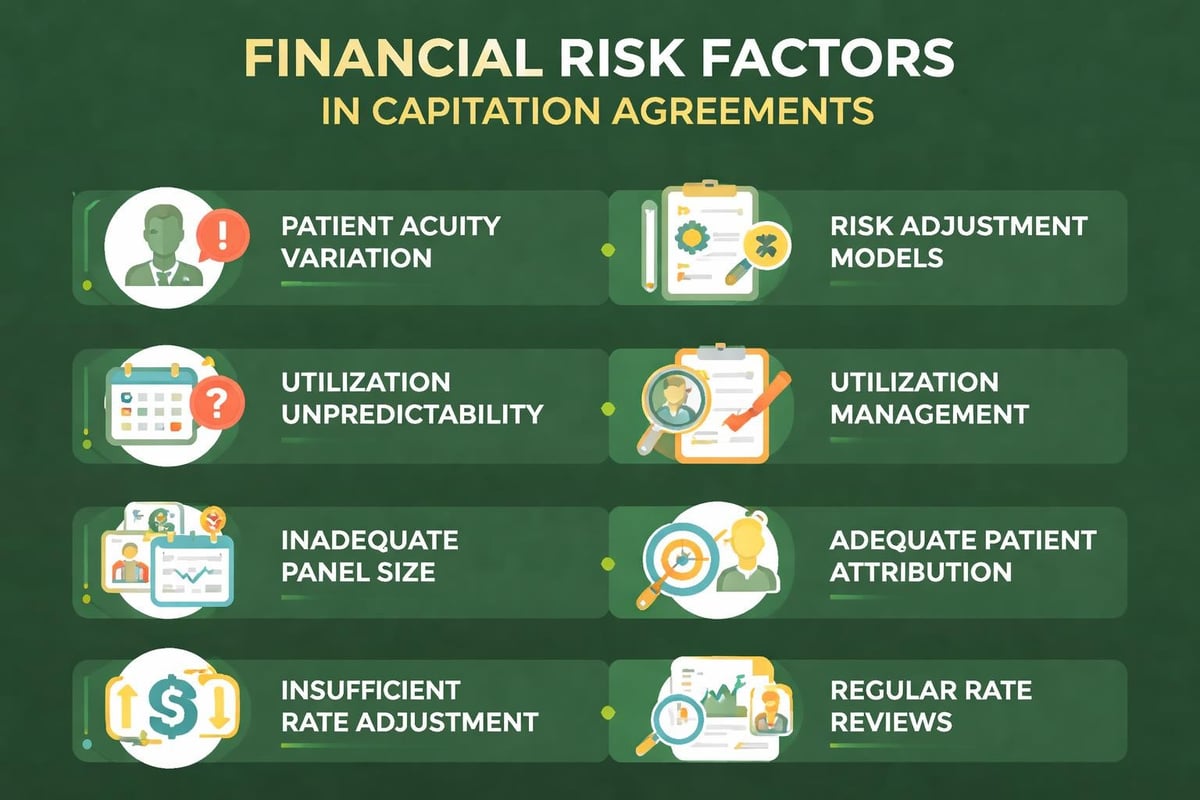
Providers accepting capitation assume financial responsibility for patient care costs. If actual utilization exceeds projected rates used to calculate capitation payments, providers bear the loss. This risk increases with:
- High-acuity patient populations
- Unpredictable service utilization patterns
- Inadequate risk adjustment in payment calculations
- Limited patient panel sizes that prevent risk pooling
Organizations must conduct thorough financial analysis before accepting capitation contracts, ensuring rates adequately cover anticipated costs with appropriate reserves for variation.
Potential Quality Concerns
Critics argue capitation may incentivize providers to withhold necessary services to control costs. While this represents a theoretical concern, professional ethics, quality metrics, and regulatory oversight generally prevent such practices. However, providers must implement robust quality monitoring to ensure care standards remain high under capitation arrangements.
Complex Patient Attribution
Determining which patients belong to a provider's capitated panel can create administrative challenges. Patient movement between providers, changing insurance coverage, and unclear attribution rules complicate accurate panel management. Revenue cycle management teams must maintain accurate patient rosters to ensure appropriate capitation payments.
Best Practices for Managing Capitation Contracts
Successful capitation management requires strategic planning, robust systems, and ongoing monitoring. Healthcare providers can implement several best practices to optimize performance under these arrangements.
Step 1: Conduct Thorough Financial Analysis
Before accepting any capitation arrangement, perform comprehensive analysis of proposed rates against your practice's cost structure and patient population characteristics. Evaluate historical utilization data, patient demographics, and expected service patterns. Ensure rates provide adequate coverage with appropriate margins for variation.
Step 2: Implement Strong Utilization Management
Develop systems to monitor and manage patient utilization effectively. Track service patterns, identify high-utilizing patients, and implement care management programs for complex cases. Regular utilization review helps identify trends and opportunities for intervention before costs escalate.
Step 3: Build Adequate Patient Panel Size
Larger patient panels allow better risk distribution across the population. Small panels create vulnerability to high-cost outlier patients who can significantly impact financial performance. Work with payers to ensure panel sizes support sustainable operations.
Step 4: Invest in Care Coordination Infrastructure
Effective care coordination represents a cornerstone of successful capitation management. Implement systems supporting:
- Care team communication
- Transition management
- Chronic disease programs
- Patient engagement tools
- Preventive care tracking
Step 5: Monitor Quality Metrics Continuously
Maintain robust quality monitoring programs to ensure care standards remain high while managing costs. Track clinical outcomes, patient satisfaction, preventive care measures, and other relevant metrics. Quality performance often ties to contract retention and rate negotiations.
Revenue Cycle Management Considerations
Capitation fundamentally changes revenue cycle workflows compared to traditional fee-for-service billing. Healthcare providers must adapt their revenue cycle management processes to accommodate this payment model effectively.
Modified Billing and Claims Processes
While capitation reduces individual claim volume, revenue cycle teams must still manage capitation-specific processes including:
- Panel enrollment verification
- Monthly capitation payment reconciliation
- Carve-out service billing for non-covered items
- Risk adjustment documentation and submission
- Stop-loss claim filing when applicable
Professional revenue cycle management services understand these nuanced requirements and implement appropriate workflows supporting capitation arrangements alongside traditional billing.
Financial Reporting and Analysis
Capitation requires different financial reporting approaches than fee-for-service models. Rather than tracking revenue per service, organizations must monitor metrics including:
| Metric | Purpose | Target |
|---|---|---|
| Per-Member-Per-Month (PMPM) costs | Track average patient care costs | Below capitation rate |
| Medical loss ratio | Measure clinical costs vs. revenue | 80-90% |
| Patient panel size | Ensure adequate risk distribution | Provider-specific |
| Utilization rates | Monitor service consumption patterns | Benchmark comparison |
Risk Adjustment and Documentation
Many capitation arrangements include risk adjustment components where payments increase for patients with chronic conditions or higher expected costs. Proper documentation of patient conditions, diagnoses, and risk factors directly impacts capitation revenue. Revenue cycle teams must ensure comprehensive documentation supporting accurate risk scoring.
Integrating Capitation with Fee-for-Service Revenue
Most healthcare providers maintain mixed payment models, receiving both capitation payments and fee-for-service reimbursement from different payers. This complexity requires sophisticated revenue cycle management capabilities to track, optimize, and reconcile diverse payment streams.
Practices must maintain systems distinguishing capitated from non-capitated patients at the point of service. Staff need clear protocols for identifying which services fall under capitation agreements versus those requiring separate billing. Definitive guidance on capitation structures helps revenue cycle teams implement appropriate workflows.
Contract Management Systems
Effective capitation management requires robust contract tracking systems documenting:
- Covered services under each capitation agreement
- Carve-out services requiring separate billing
- Patient attribution and panel rosters
- Rate schedules and adjustment provisions
- Quality metric requirements
- Reporting obligations
Revenue cycle management professionals leverage these systems to ensure appropriate billing, prevent revenue leakage, and maintain compliance with contractual obligations.
Technology and Capitation Management
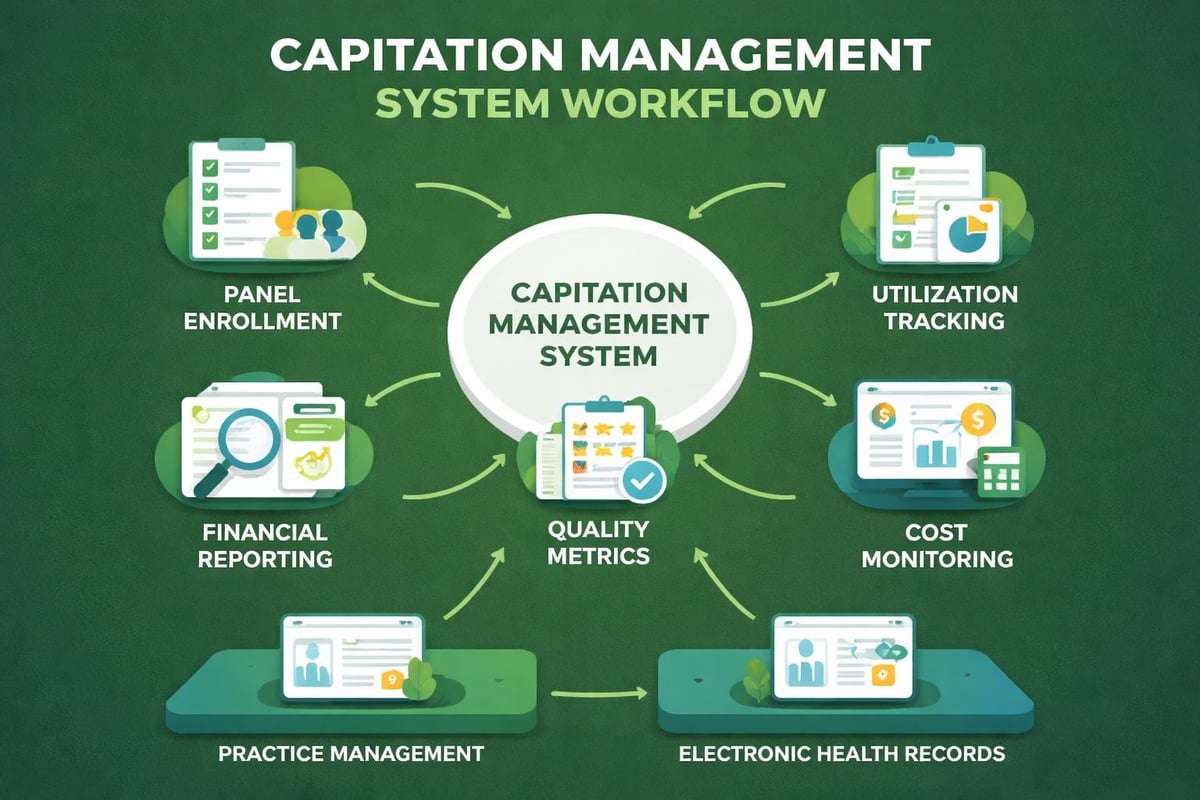
Modern practice management and electronic health record systems increasingly incorporate functionality supporting capitation arrangements. These tools enable better tracking, reporting, and financial management under capitated payment models.
Advanced systems provide capabilities including automated panel management, utilization tracking, financial forecasting, and quality metric reporting. Organizations accepting significant capitation revenue should ensure their technology infrastructure adequately supports these requirements.
For practices lacking internal expertise in capitation management, partnering with specialized revenue cycle management providers offers access to experienced professionals and proven systems without significant capital investment.
Regulatory and Compliance Considerations
Capitation arrangements operate within complex regulatory frameworks at federal and state levels. Healthcare providers must maintain compliance with applicable regulations while managing these contracts.
Medicare Advantage and Medicaid Managed Care
Government payer programs increasingly use capitation models through Medicare Advantage plans and Medicaid managed care organizations. These programs include specific requirements regarding quality reporting, risk adjustment, and patient protections that providers must understand and fulfill.
State Insurance Regulations
State insurance departments regulate capitation arrangements, often requiring specific contractual provisions, financial reserves, and consumer protections. Providers should understand applicable state requirements before finalizing capitation contracts.
Anti-Kickback and Stark Considerations
Healthcare providers must ensure capitation arrangements comply with federal anti-kickback and Stark law requirements. Properly structured capitation contracts generally satisfy safe harbor provisions, but legal review ensures compliance.
Negotiating Favorable Capitation Contracts
Healthcare organizations can take proactive steps during contract negotiations to secure favorable terms supporting financial stability and quality care delivery.
Key Negotiation Points:
- Adequate capitation rates based on realistic utilization projections and cost analysis
- Clear service definitions specifying exactly which services the capitation rate covers
- Risk corridor provisions limiting provider downside exposure during initial contract periods
- Stop-loss protection covering catastrophic individual patient costs above defined thresholds
- Timely payment provisions ensuring predictable cash flow
- Termination clauses allowing exit under specified circumstances
- Quality metric alignment with achievable, evidence-based performance standards
Organizations should approach capitation negotiations with comprehensive data supporting their position, including historical utilization patterns, cost structures, and patient demographics. Professional revenue cycle management expertise provides valuable support during these negotiations.
Future Trends in Capitation Payment Models
Healthcare payment continues evolving toward value-based arrangements, with capitation representing one component of this broader transformation. Several trends suggest capitation in medical billing will play an expanding role in healthcare finance.
Increased Prevalence in Commercial Insurance
While capitation traditionally focused on government programs and managed care organizations, commercial insurers increasingly experiment with capitated arrangements. This expansion creates new opportunities and challenges for healthcare providers across specialties.
Enhanced Risk Adjustment Sophistication
Payers continue refining risk adjustment methodologies to more accurately align capitation payments with patient acuity and expected costs. This sophistication should improve the fairness and sustainability of capitation arrangements while requiring enhanced documentation from providers.
Integration with Value-Based Payment Models
Capitation increasingly integrates with other value-based payment approaches including shared savings, quality incentives, and bundled payments. These hybrid models attempt to balance payment predictability with performance accountability.
The trajectory toward value-based care positions capitation as an important payment mechanism for healthcare providers. Organizations developing capabilities around capitation management position themselves advantageously for future market conditions.
Capitation in medical billing represents a fundamental shift from traditional fee-for-service models, offering revenue predictability while requiring sophisticated management of financial risk and care delivery. Success under capitation arrangements demands thorough analysis, robust systems, and ongoing monitoring to balance cost control with quality care. Greenhive Billing Solutions provides comprehensive revenue cycle management services supporting healthcare providers navigating capitation contracts alongside traditional billing models, delivering the expertise and systems necessary to optimize financial performance across diverse payment structures.