Accurate revenue cycle management depends on multiple interconnected processes, with benefit verification in medical billing serving as a critical first step that determines financial outcomes for healthcare practices. When providers verify insurance benefits before delivering services, they establish clear expectations about coverage, reduce claim denials, and ensure patients understand their financial responsibilities. This fundamental administrative process has evolved from simple phone calls to sophisticated verification systems that healthcare organizations must master to maintain healthy cash flow and minimize revenue disruption.
Understanding the Foundation of Benefit Verification
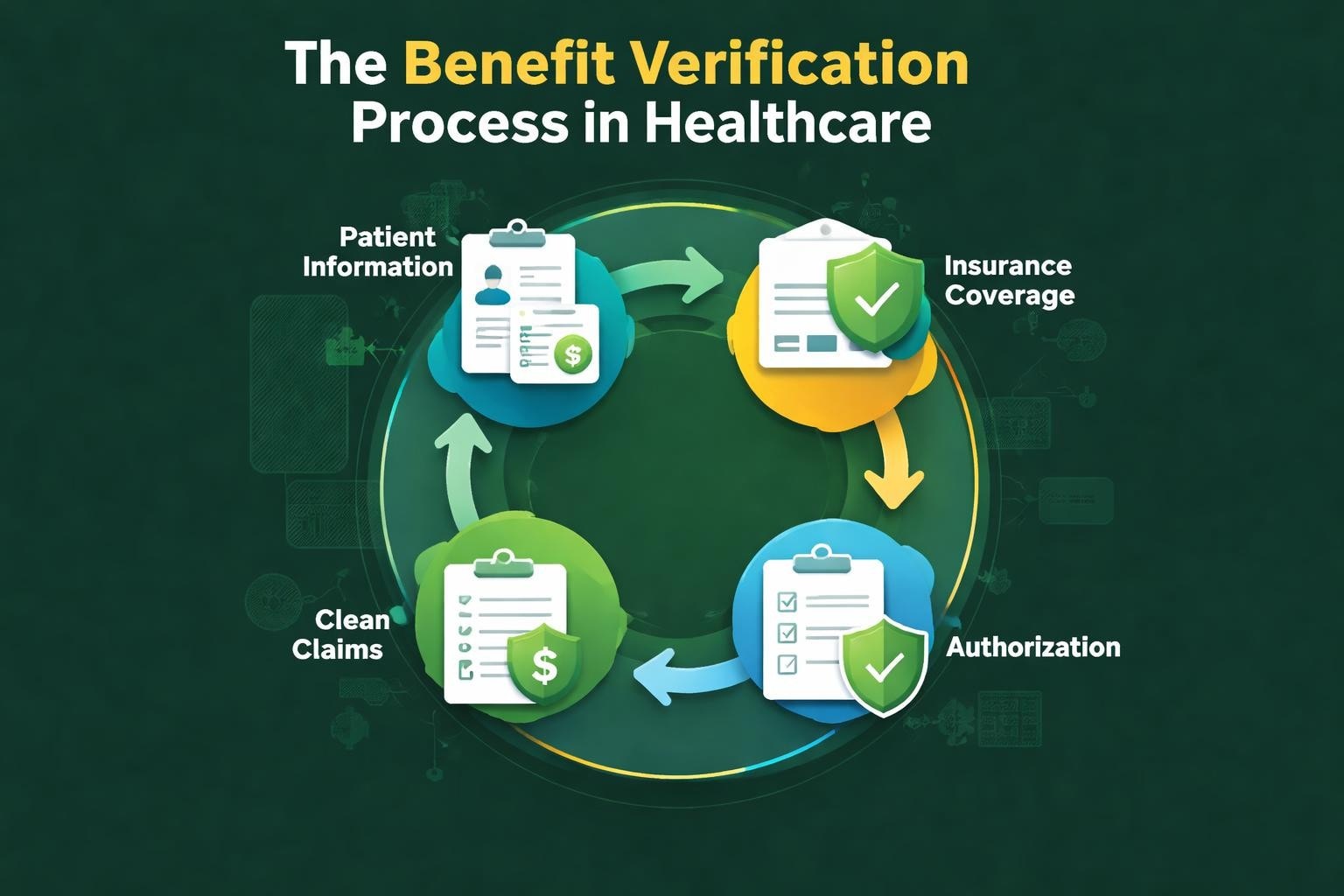
Benefit verification in medical billing represents the systematic process of confirming a patient's insurance coverage, determining what services are covered, and identifying any limitations or requirements before treatment begins. This verification goes far beyond simply checking whether a patient has active insurance coverage.
The process involves gathering comprehensive information about coverage details, including deductibles, copayments, coinsurance amounts, and out-of-pocket maximums. Healthcare providers must also identify any authorization requirements, referral needs, or pre-certification protocols that specific insurance plans mandate. Without this thorough verification, practices risk providing services that may not be reimbursed or discovering coverage limitations only after treatment has been delivered.
Why Verification Matters for Healthcare Providers
Financial stability in healthcare practices depends heavily on accurate upfront information about patient coverage. Accurate eligibility and benefits verification helps reduce claim denials and write-offs that directly impact practice revenue. When verification errors occur, the consequences extend beyond delayed payments to include increased administrative costs, patient satisfaction issues, and potential bad debt.
The relationship between verification accuracy and denial rates is significant. Practices that implement comprehensive verification processes typically experience lower denial rates and faster payment cycles. This correlation exists because proper verification identifies potential coverage issues before services are rendered, allowing staff to address problems proactively rather than reactively managing denied claims.
Key Components of Effective Benefit Verification
Successful benefit verification in medical billing requires attention to multiple data points and careful documentation of findings. Each component plays a specific role in building a complete picture of patient coverage.
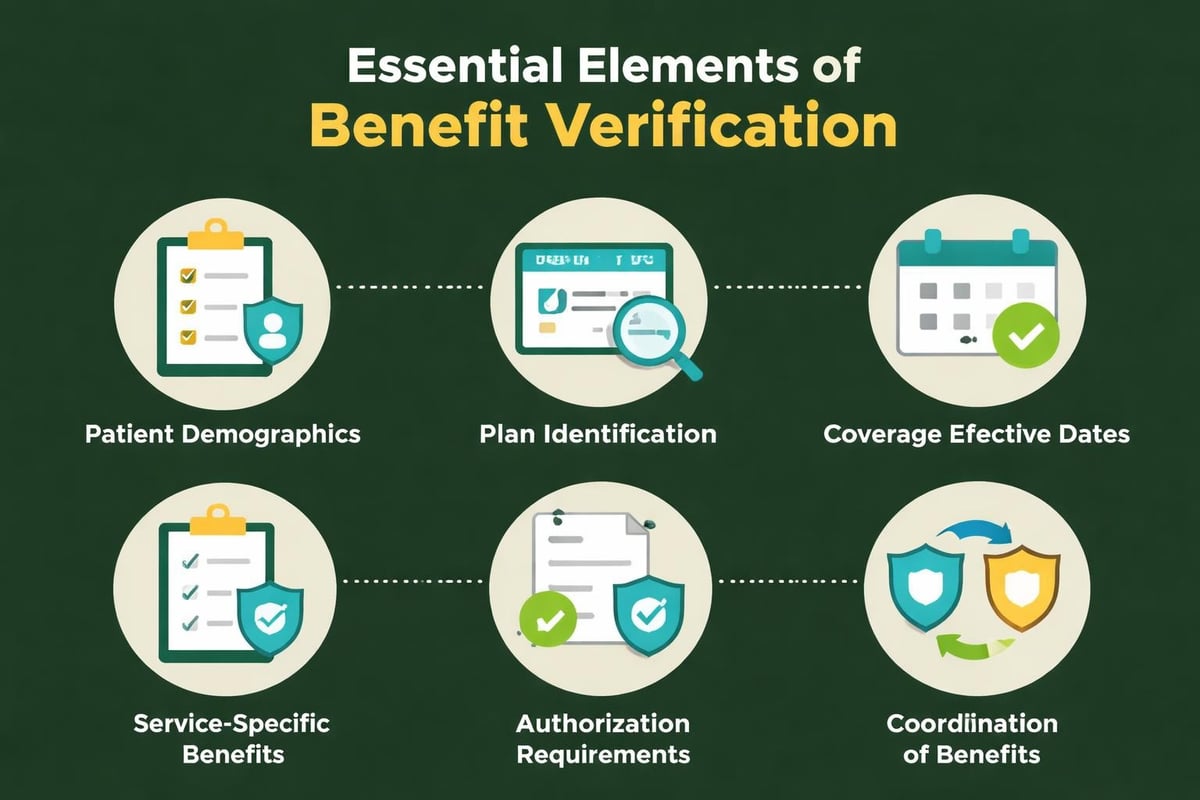
Essential Information to Verify
Healthcare providers must collect and verify specific information categories during the benefits verification process:
- Patient demographics and identification including full legal name, date of birth, and contact information
- Insurance plan details such as policy number, group number, and plan type
- Coverage dates to confirm active status during the anticipated service date
- Deductible status including annual amounts and year-to-date payments
- Copayment and coinsurance requirements for the specific services planned
- Out-of-pocket maximum amounts and current status
- Network status confirming whether the provider is in-network
- Service-specific coverage for the procedures or treatments planned
- Authorization and referral requirements for the planned services
- Coordination of benefits if multiple insurance policies exist
The verification team must document all findings thoroughly, creating a record that billing staff can reference when submitting claims. This documentation protects both the practice and the patient by establishing what information was confirmed before treatment.
Timing Considerations for Verification
The American Psychiatric Association provides detailed guidelines on verifying benefit coverage that emphasize performing verification at optimal times. Different practice types require different timing approaches based on their scheduling patterns and service types.
| Practice Type | Recommended Verification Timing | Rationale |
|---|---|---|
| Primary Care | 1-2 business days before appointment | Allows time to address issues without delaying routine care |
| Surgical Practices | 5-7 business days before procedure | Provides sufficient time for authorization processes |
| Specialty Care | 3-5 business days before visit | Balances thoroughness with scheduling flexibility |
| Emergency Services | Point of service or within 24 hours | Coverage verification follows urgent care delivery |
Proper timing ensures that verification information remains current while providing adequate time to resolve any discovered issues before the patient appointment.
The Step-by-Step Verification Process
Implementing a standardized verification workflow reduces errors and ensures consistency across all patient interactions. The benefit verification process follows a logical sequence that builds upon each previous step.
Step 1: Collect Patient Information
Begin by gathering complete and accurate patient information, including current insurance cards (front and back copies), photo identification, and any referral documentation. Verify that the patient name exactly matches the insurance card to prevent identity mismatches that trigger claim denials.
Step 2: Contact the Insurance Carrier
Reach out to the insurance company through their provider services line, online portal, or electronic verification system. Document the date, time, reference number, and representative name for all verification contacts.
Step 3: Confirm Coverage Details
Systematically verify each coverage element, asking specific questions about the services your practice plans to provide. Generic verification is insufficient; you must confirm coverage for the exact CPT codes and service categories relevant to the planned treatment.
Step 4: Identify Authorization Requirements
Determine whether the planned services require prior authorization, pre-certification, or referrals. If authorizations are needed, initiate the request immediately to avoid delays. Understanding denial management helps practices recognize how authorization oversights contribute to preventable denials.
Step 5: Calculate Patient Financial Responsibility
Based on verified benefit information, calculate the patient's expected out-of-pocket costs, including any applicable copayments, unmet deductible amounts, and coinsurance percentages. This calculation enables transparent financial conversations before service delivery.
Step 6: Document All Findings
Create comprehensive documentation of all verified information, storing it in the patient's record for reference during claim submission and potential appeals. Documentation should include specific benefit details, not just confirmation that verification was completed.
Common Challenges in Benefit Verification
Even well-established verification processes encounter obstacles that can compromise accuracy and efficiency. Recognizing these challenges helps practices develop strategies to overcome them.
Insurance Information Accuracy
Patients frequently provide outdated insurance cards or incorrect policy information, particularly after open enrollment periods or job changes. This fundamental data problem cascades through the entire verification process, producing unreliable results even when verification procedures are followed correctly.
Staff must develop tactful approaches to confirming that patients have provided current insurance information, including asking directly about recent coverage changes and encouraging patients to verify their information with their employers.
Variable Insurance Representative Knowledge
Insurance company representatives possess varying levels of knowledge and may provide inconsistent or incomplete information. Some representatives focus only on active coverage status without proactively sharing important details about authorization requirements or coverage limitations.
Experienced verification staff develop specific question lists that prompt representatives to provide complete information rather than relying on representatives to volunteer all relevant details.
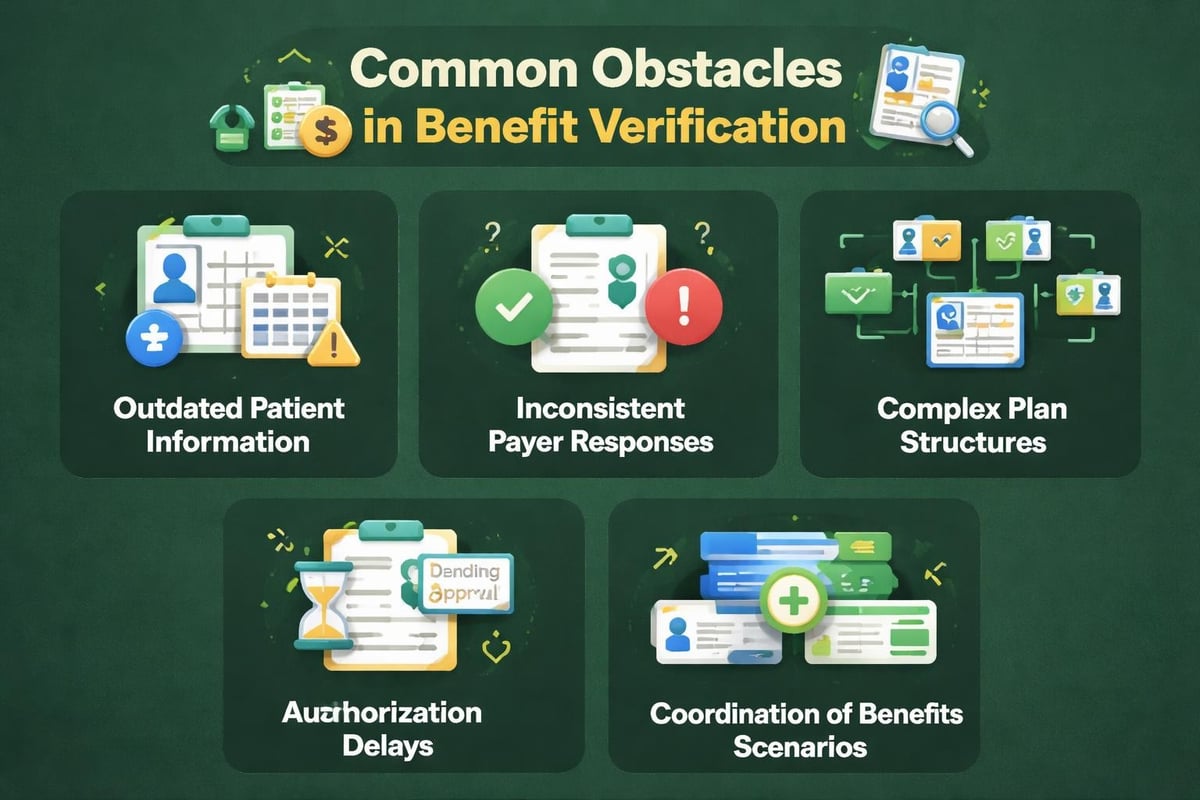
Complex Plan Structures
Modern insurance plans incorporate numerous variables including tiered networks, service-specific deductibles, and complex coinsurance structures that challenge even experienced verification staff. High-deductible health plans with health savings accounts introduce additional complexity requiring careful explanation to patients.
Creating reference guides for commonly encountered plan types helps staff quickly identify which questions to ask and what information to prioritize for different plan categories.
The Role of Technology in Modern Verification
Healthcare practices increasingly leverage technology to enhance verification accuracy and efficiency. While some providers employ fully automated systems, others use technology to support manual verification processes performed by skilled staff members.
Electronic Verification Systems
Electronic systems query insurance databases in real-time, providing instant access to eligibility and benefit information. Automated benefits verification offers significant advantages including reduced errors and lower claim denials, though these systems work best when combined with human oversight for complex cases.
Revenue cycle management services utilize industry-standard verification platforms that integrate with practice management systems, enabling seamless data transfer and reducing duplicate data entry. These tools support verification teams but do not replace the judgment and problem-solving capabilities that experienced professionals provide.
Integration with Practice Management Systems
Modern verification workflows benefit from systems that automatically populate verified information into billing software, reducing transcription errors and ensuring that claim submission reflects accurate benefit details. This integration supports clean claim submission by embedding verified data directly into the claim creation process.
Financial Impact of Verification Accuracy
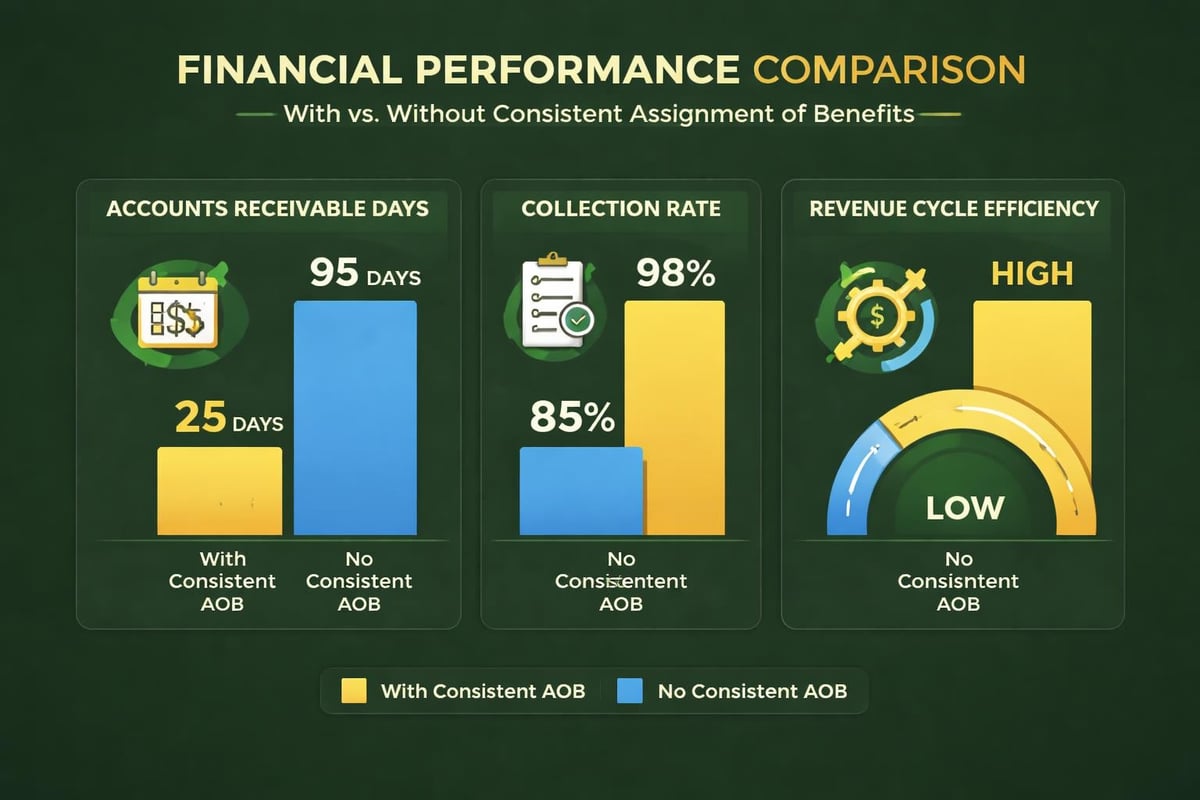
The relationship between thorough benefit verification in medical billing and practice financial performance is direct and measurable. Practices that prioritize verification quality experience tangible benefits across multiple financial metrics.
Denial Rate Reduction
Verification errors frequently appear among the top causes of claim denials. When practices verify benefits accurately, they eliminate a significant category of preventable denials. This reduction translates directly to faster payments and decreased administrative costs associated with denial management.
Practices tracking denial reasons often discover that eligibility and benefit verification issues account for 15-25% of all initial denials. Addressing this category through improved verification processes yields immediate financial returns.
Improved Cash Flow Predictability
Accurate benefit verification enables more reliable revenue forecasting by reducing uncertainty about payment sources and amounts. When practices know in advance which claims may face patient responsibility challenges or require additional documentation, they can plan accordingly and manage accounts receivable more effectively.
Understanding healthcare revenue cycle analytics helps practices measure how verification improvements impact overall financial performance.
Patient Collection Enhancement
Patients who receive clear information about their financial responsibilities before service delivery are more likely to make timely payments. Verification that accurately determines patient responsibility enables meaningful financial conversations that set appropriate expectations and establish payment arrangements when needed.
| Verification Quality | Average Collection Rate | Days in A/R | Patient Satisfaction |
|---|---|---|---|
| Comprehensive | 85-92% | 32-38 days | High |
| Basic | 68-75% | 45-55 days | Moderate |
| Minimal | 52-63% | 60+ days | Low |
Best Practices for Verification Excellence
Healthcare practices that achieve superior verification outcomes share common approaches and priorities that distinguish them from organizations treating verification as a perfunctory administrative task.
Develop Comprehensive Training Programs
Staff performing benefit verification require thorough training that covers insurance fundamentals, common plan types, verification techniques, and documentation requirements. This training should extend beyond initial onboarding to include regular updates about changing insurance requirements and emerging verification challenges.
Working with skilled billing and coding specialists ensures that verification teams understand how their work impacts downstream billing processes and can anticipate potential coding and billing complications.
Establish Quality Assurance Processes
Regular auditing of verification accuracy helps identify training needs, process gaps, and opportunities for improvement. Quality assurance should examine both the completeness of verification documentation and the accuracy of information recorded.
Effective quality assurance programs review a representative sample of verifications, checking that staff asked appropriate questions, documented responses thoroughly, and correctly interpreted benefit information.
Create Specialty-Specific Verification Protocols
Different medical specialties encounter unique verification challenges based on the services they provide. Creating customized verification checklists for various service categories ensures that staff gather all relevant information for specific treatment types.
Surgical practices need detailed information about facility coverage and anesthesia benefits, while behavioral health providers must verify session limits and treatment plan requirements. Generic verification approaches miss these specialty-specific details.
Maintain Updated Insurance Reference Resources
Insurance plans change annually, and mid-year modifications occur with increasing frequency. Verification teams need access to current information about common plans, including contact numbers, portal access, and known coverage quirks.
Building and maintaining an insurance reference database reduces verification time and improves accuracy by providing staff with quick access to plan-specific information.
Communicating Verification Results to Patients
The information gathered through benefit verification in medical billing serves limited purpose if practices fail to communicate findings effectively to patients. Transparent communication about coverage and patient financial responsibility builds trust and improves collection outcomes.
Financial Counseling Conversations
Trained staff should discuss verification findings with patients before service delivery, explaining coverage details in clear, non-technical language. These conversations should address:
- What services are covered and any coverage limitations
- The patient's expected out-of-pocket costs
- Any authorization requirements and their status
- Payment options available through the practice
- What happens if circumstances change after verification
Patients appreciate transparency about costs and coverage, and these conversations prevent surprises that damage patient relationships and complicate collections.
Written Verification Summaries
Providing patients with written summaries of verified benefits and estimated costs creates a reference document that patients can review and share with family members involved in healthcare decisions. Written summaries also document that the practice communicated financial information before treatment.
Managing Verification for Different Payer Categories
Different insurance types require adjusted verification approaches based on their unique characteristics and requirements. Experienced verification teams recognize these distinctions and adapt their processes accordingly.
Commercial Insurance Plans
Commercial payers typically offer the most straightforward verification experiences, with accessible representatives and robust online verification portals. However, commercial plans also present the greatest variety in benefit structures, requiring careful attention to plan-specific details.
Verification of benefits for commercial insurance requires systematic approaches that account for network tiers, varying deductibles, and service-specific coverage rules.
Medicare and Medicare Advantage
Original Medicare follows relatively consistent coverage rules, though verification still requires confirming active Part A and Part B coverage, checking supplement policies, and identifying any assignment restrictions. Medicare Advantage plans function more like commercial insurance with network requirements and authorization protocols.
Medicaid Programs
Medicaid verification presents unique challenges due to program variations across states, managed care organization involvement, and frequent changes in patient eligibility status. Practices serving Medicaid populations benefit from frequent eligibility checks, sometimes at every encounter.
Self-Pay and Uninsured Patients
Even patients without insurance coverage require verification processes that document uninsured status and establish clear financial expectations before service delivery. These conversations should include information about available payment plans and financial assistance programs.
Verification's Role in Revenue Cycle Management
Benefit verification in medical billing functions as a foundational element within comprehensive revenue cycle management strategies. Its impact extends throughout the entire revenue cycle, influencing outcomes at multiple stages.
Front-End Revenue Cycle Impact
Verification quality determines the accuracy of patient registration data, which feeds directly into claim creation. Errors introduced during verification perpetuate through the revenue cycle, ultimately manifesting as denials, delays, or patient balance complications.
Strong front-end processes, including thorough verification, prevent downstream problems that require significantly more resources to resolve than preventing the initial error would have required.
Claim Submission Efficiency
When verification provides complete and accurate benefit information, billing staff can submit cleaner claims that contain all necessary authorizations, correct coding, and appropriate billing details. This efficiency reduces claim rejection rates and accelerates payment cycles.
Appeal and Denial Management
Even with excellent verification, some claims face denials for reasons unrelated to eligibility or benefits. However, documented verification provides essential evidence during the appeal process, demonstrating that the practice performed appropriate due diligence before rendering services.
Outsourcing Verification Functions
Many healthcare practices partner with specialized revenue cycle management service providers to handle benefit verification processes. This approach offers several advantages while requiring careful vendor selection and ongoing oversight.
Benefits of Professional Verification Services
Experienced RCM partners bring dedicated staff trained specifically in verification processes, access to multiple verification platforms, and established relationships with major payers. These providers often achieve higher accuracy rates than practices attempting to manage verification internally alongside competing priorities.
Professional verification services also provide scalability, adjusting staffing levels to match patient volume fluctuations without requiring practices to manage hiring, training, and supervision of verification personnel.
Maintaining Quality Oversight
Practices utilizing external verification services must establish clear quality expectations, regular reporting requirements, and ongoing communication channels. The partnership works best when both parties view verification as a collaborative process rather than a fully delegated function.
Measuring Verification Performance
Healthcare practices should track specific metrics that reveal verification process effectiveness and identify improvement opportunities. Data-driven approaches to verification management support continuous quality enhancement.
Key performance indicators for verification include:
- Verification completion rate: Percentage of scheduled patients with completed verification before appointment
- Verification accuracy rate: Percentage of verifications containing accurate benefit information
- Authorization acquisition rate: Percentage of required authorizations obtained before service delivery
- Time per verification: Average minutes required to complete verification process
- Denial rate for verification-related reasons: Percentage of claims denied due to eligibility or benefit issues
Regular review of these metrics helps practices identify trends, recognize training needs, and celebrate improvements.
Effective benefit verification in medical billing establishes the foundation for successful revenue cycle outcomes by ensuring accurate coverage information before service delivery, reducing denials, and enabling transparent patient communication. Healthcare providers seeking to optimize their verification processes while maintaining focus on patient care can benefit from partnering with experienced revenue cycle management specialists. Greenhive Billing Solutions provides comprehensive verification services performed by skilled professionals who utilize industry-standard platforms to deliver accurate, timely benefit information that supports clean claims and improved financial performance for healthcare practices nationwide.