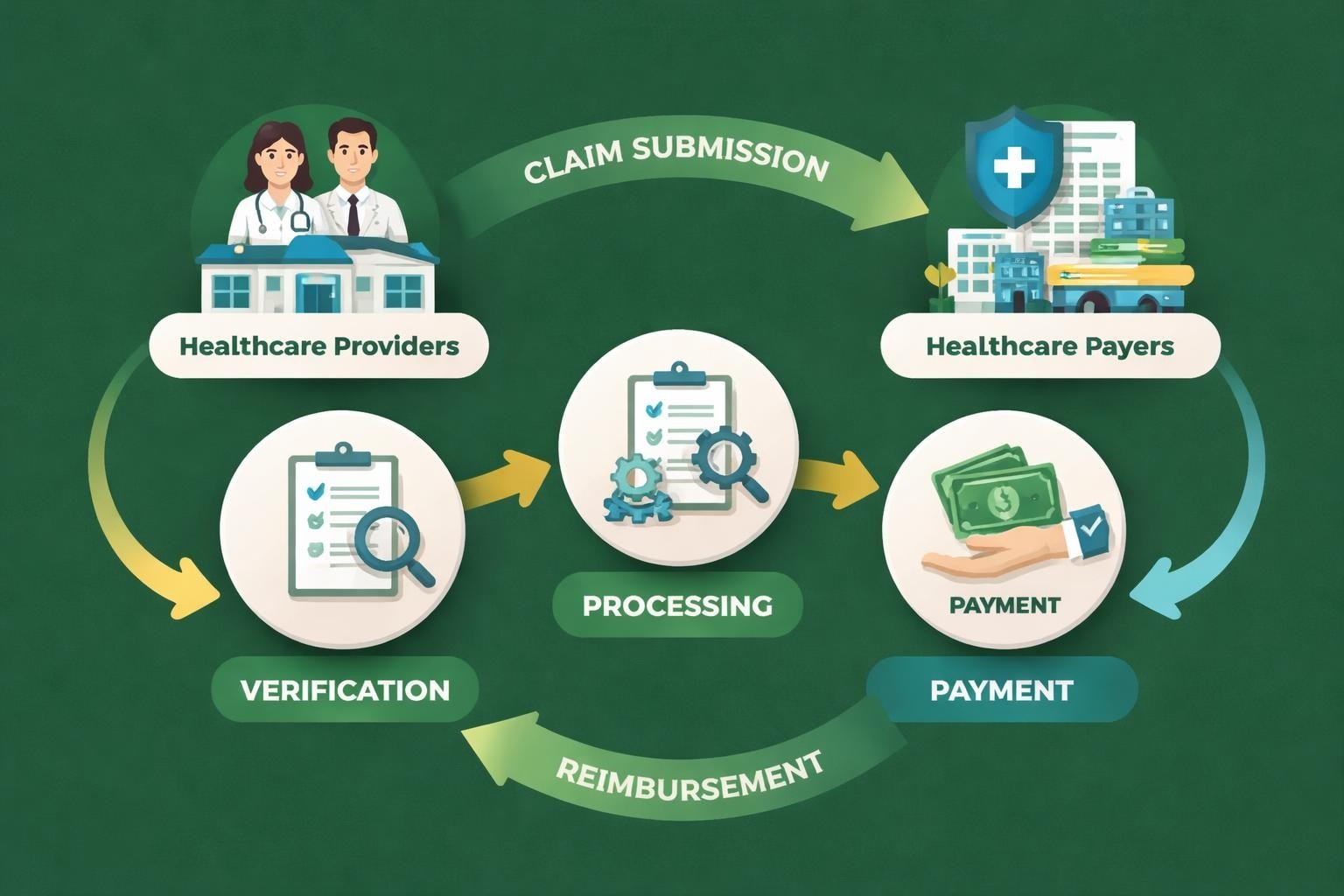
The relationship between healthcare providers and a healthcare payer represents one of the most critical components in maintaining financial stability for medical practices. Understanding how these entities operate, their requirements, and the intricacies of claim processing can significantly impact a practice's bottom line. For healthcare organizations seeking to optimize their revenue cycle management, developing expertise in payer relationships and requirements has become essential for sustainable operations and consistent cash flow.
Understanding Healthcare Payer Categories
A healthcare payer functions as the entity responsible for reimbursing healthcare providers for services rendered to patients. These organizations fall into distinct categories, each with unique characteristics and requirements.
Government-Sponsored Programs
Medicare serves as the federal health insurance program primarily covering individuals aged 65 and older, along with certain younger individuals with disabilities. This healthcare payer operates under strict regulations and standardized billing requirements that demand precise documentation and coding accuracy.
Medicaid functions as a joint federal and state program providing coverage for eligible low-income individuals and families. Each state administers its own Medicaid program, creating variations in coverage policies, reimbursement rates, and documentation requirements across different jurisdictions.
The Medicare and Medicaid landscape continues to evolve with changing spending patterns and strategic considerations that directly affect provider reimbursement.
Commercial Insurance Companies
Private insurance companies represent a significant portion of the healthcare payer landscape. These entities offer various plan types including HMOs, PPOs, and EPOs, each with distinct authorization requirements and reimbursement methodologies.

Commercial payers negotiate contracts with provider networks, establishing fee schedules and claim submission protocols that vary considerably between organizations. Understanding these nuances becomes crucial for effective revenue cycle management.
| Payer Type | Key Characteristics | Primary Consideration |
|---|---|---|
| Medicare | Federal program, standardized requirements | Compliance with CMS guidelines |
| Medicaid | State-administered, varying policies | State-specific regulations |
| Commercial | Contract-based, negotiable rates | Network participation agreements |
| Managed Care | Utilization management focus | Prior authorization protocols |
Critical Components of Healthcare Payer Interactions
Successful navigation of healthcare payer relationships requires attention to multiple operational elements that directly influence reimbursement outcomes.
Insurance Eligibility Verification
Before rendering services, confirming patient coverage status with the healthcare payer prevents claim denials and reduces revenue delays. This process involves:
- Verifying active coverage and policy effective dates
- Identifying plan-specific requirements and limitations
- Confirming patient responsibility including deductibles and copayments
- Checking prior authorization requirements for scheduled procedures
Real-time eligibility verification reduces claim rejections by ensuring accurate information flows from the initial patient encounter through final billing submission.
Prior Authorization Requirements
Many healthcare payer organizations require advance approval for specific services, procedures, or medications. Failure to obtain proper authorization before service delivery typically results in claim denials and lost revenue.
Authorization requirements vary significantly between payers and even between different plans offered by the same organization. Maintaining current knowledge of these requirements and implementing systematic tracking processes helps prevent authorization-related denials.
Healthcare Payer Claim Processing Dynamics
Understanding how a healthcare payer processes claims enables providers to submit clean claims that move efficiently through adjudication, reducing delays and increasing first-pass acceptance rates.
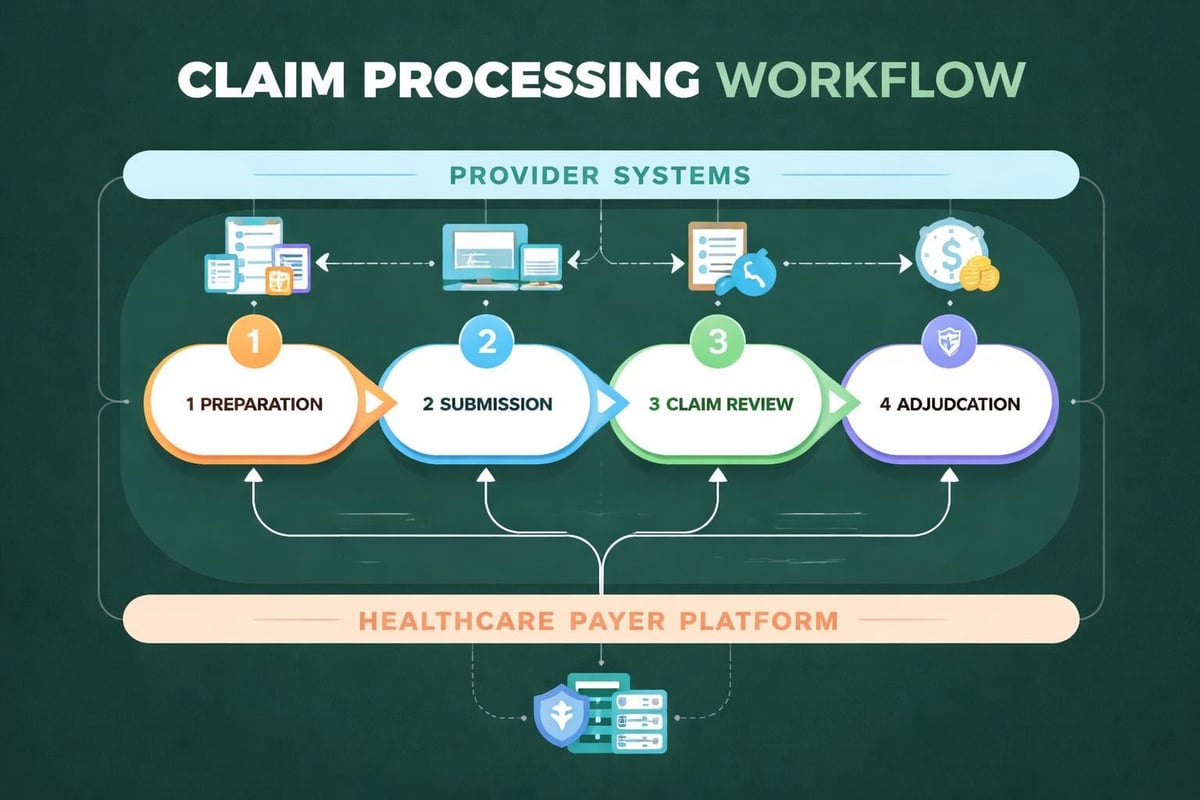
The Claim Submission Process
Step 1: Claim Preparation
Gather complete documentation including patient demographics, insurance information, diagnosis codes, procedure codes, and supporting clinical documentation.
Step 2: Claim Scrubbing
Review claims for common errors including coding inconsistencies, missing information, and policy violations before submission to the healthcare payer.
Step 3: Electronic Submission
Transmit claims through clearinghouses or directly to payers using standardized electronic formats that meet industry requirements.
Step 4: Acknowledgment Receipt
Monitor for acknowledgment reports confirming successful receipt and initial acceptance by the healthcare payer system.
Step 5: Adjudication Tracking
Follow claim status through the payer's processing system, identifying any holds or additional information requests.
The challenges in payment integrity continue to impact how healthcare payer organizations review and process claims, making accurate submission increasingly important.
Common Claim Rejection Scenarios
Healthcare payer systems automatically reject claims containing specific errors or inconsistencies. Understanding these common rejection triggers allows practices to implement preventive measures:
- Demographic mismatches between submitted information and payer records
- Invalid or expired insurance identification numbers not matching active coverage
- Coding errors including incorrect code formats or invalid code combinations
- Missing required information such as referring provider details or place of service
- Duplicate claim submissions for services already processed
Managing Healthcare Payer Denials Effectively
Even with meticulous claim preparation, denials occur. Developing systematic approaches to denial management protects revenue and identifies opportunities for process improvement.
Denial Categories and Response Strategies
| Denial Type | Common Causes | Resolution Approach |
|---|---|---|
| Technical | Missing information, coding errors | Correct and resubmit promptly |
| Clinical | Medical necessity, documentation | Submit clinical appeal with supporting evidence |
| Administrative | Authorization issues, timely filing | Provide proof of compliance or request reconsideration |
| Coverage | Non-covered services, benefit limitations | Educate patient, arrange alternative payment |
A healthcare payer may deny claims for multiple reasons, requiring providers to analyze denial patterns and implement targeted prevention strategies. Emerging payer behavior trends show increasingly sophisticated denial approaches that demand equally sophisticated management responses.
Building an Effective Appeals Process
When addressing healthcare payer denials through appeals, structure matters significantly for success rates.
Organize appeals with clear documentation demonstrating why the claim meets coverage criteria. Include relevant medical records, clinical guidelines supporting medical necessity, and specific policy language supporting the claim. Submit appeals within designated timeframes, as missing deadlines typically eliminates appeal rights.
Track appeal outcomes to identify patterns indicating systemic issues requiring either process changes or payer contract renegotiation.
Optimizing Healthcare Payer Contract Performance
Provider contracts with healthcare payer organizations establish the financial framework for reimbursement. Understanding and monitoring these agreements directly impacts revenue performance.
Key Contract Elements
Fee schedules define payment amounts for specific services and procedures. These may be based on percentage of Medicare rates, negotiated flat fees, or other methodologies depending on the healthcare payer and market dynamics.
Claim submission requirements outline specific protocols for billing, including acceptable formats, required documentation, and submission deadlines that providers must follow.
Quality metrics and performance standards increasingly tie reimbursement to outcome measures, requiring providers to track and report specific clinical and operational indicators.
The pressures facing healthcare payer sustainability influence contract negotiations and reimbursement methodologies, creating evolving expectations for provider performance.
Technology Integration for Healthcare Payer Management
Modern revenue cycle management relies heavily on technology solutions that streamline interactions with healthcare payer systems and improve operational efficiency.
Essential Technology Functions
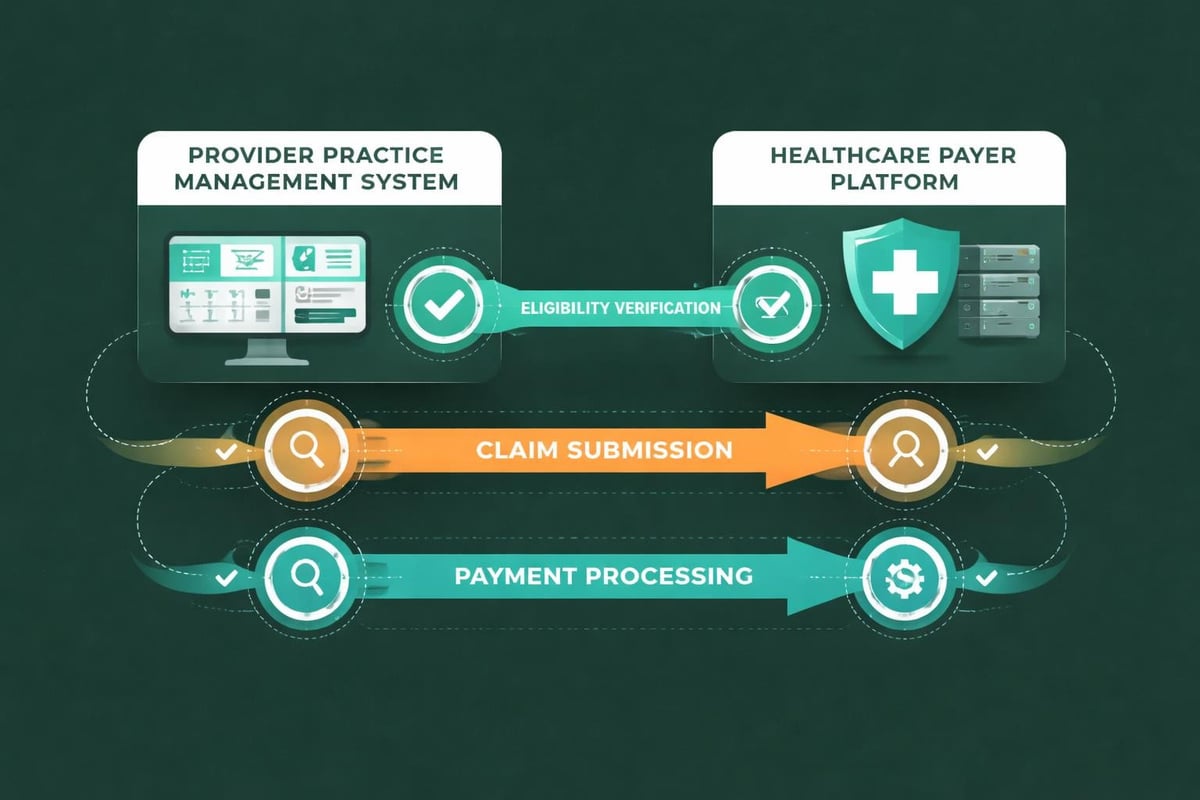
Practice management systems integrate eligibility verification, claim submission, and payment posting in unified platforms. These systems connect directly with healthcare payer networks, enabling real-time information exchange and reducing manual data entry.
Electronic remittance advice (ERA) processing automates payment reconciliation, allowing systems to automatically post payments and adjustments based on payer explanations of benefits.
Automated claim scrubbing identifies potential errors before submission to the healthcare payer, significantly reducing rejection rates and accelerating reimbursement timelines.
Analytics platforms track key performance indicators across different healthcare payer relationships, highlighting opportunities for improvement in areas such as denial rates, days in accounts receivable, and first-pass acceptance rates.
Regulatory Compliance in Healthcare Payer Relationships
Navigating the complex regulatory environment surrounding healthcare payer interactions requires constant vigilance and systematic compliance efforts.
HIPAA Requirements
All communications and data exchanges with a healthcare payer must comply with HIPAA privacy and security regulations. This includes proper handling of protected health information during eligibility verification, claim submission, and appeals processes.
Implementing appropriate technical safeguards, administrative policies, and physical security measures protects patient information while enabling necessary business functions with payer organizations.
Billing Compliance Standards
Accurate coding and billing practices prevent compliance violations that could trigger audits or penalties. This includes:
- Using current code sets and following official coding guidelines
- Documenting medical necessity for all billed services
- Avoiding upcoding, unbundling, or other improper billing practices
- Maintaining complete and accurate medical records supporting all claims
Understanding that each healthcare payer may conduct audits to verify compliance with billing regulations and contract terms makes maintaining meticulous documentation practices essential for protecting revenue and avoiding penalties.
Healthcare Payer Communication Strategies
Effective communication with healthcare payer representatives resolves issues efficiently and builds productive working relationships that benefit long-term revenue cycle performance.
Establishing Productive Payer Relationships
Identify key contacts within each healthcare payer organization for different functions such as provider relations, claims processing, and appeals. Building relationships with these individuals creates channels for efficient problem resolution.
Document all communications with payer representatives including dates, names, reference numbers, and outcomes. This documentation proves invaluable when addressing disputed claims or authorization issues.
Regular review meetings with major healthcare payer partners provide opportunities to address systemic issues, clarify policy changes, and improve operational workflows between organizations.
Financial Impact of Healthcare Payer Mix
The composition of a practice's payer mix significantly influences financial performance and operational strategy. Understanding these dynamics enables better business planning and resource allocation.
Different healthcare payer categories reimburse at varying rates for identical services. Government programs typically reimburse at lower rates than commercial payers, making payer mix analysis crucial for financial forecasting.
Monitoring payer mix trends identifies shifts that may impact revenue, allowing practices to adjust operations proactively. For example, increasing Medicare patient volume might require operational adjustments to maintain profitability given different reimbursement rates.
The financial and regulatory challenges facing healthcare payer organizations create ripple effects that impact provider reimbursement and require strategic adaptation.
| Performance Metric | Target Range | Impact on Revenue |
|---|---|---|
| Days in A/R | 30-40 days | Cash flow management |
| First-pass acceptance rate | 95%+ | Reduced rework costs |
| Denial rate | <5% | Revenue preservation |
| Collection rate | 95%+ | Financial performance |
Credentialing and Network Participation
Maintaining current credentialing status with healthcare payer networks ensures uninterrupted claim processing and prevents unexpected denials due to credentialing lapses.
Credentialing Maintenance Requirements
Healthcare payer organizations require providers to maintain current credentials including licenses, certifications, and malpractice insurance. Allowing credentials to lapse results in claims denials until credentialing status is restored.
Primary source verification and re-credentialing cycles vary between payers but typically occur every two to three years. Tracking these timelines and submitting renewal applications proactively prevents coverage gaps.
Changes in practice information such as addresses, tax identification numbers, or provider rosters require prompt notification to each healthcare payer to ensure accurate claim processing and payment delivery.
Emerging Trends in Healthcare Payer Operations
The healthcare payer landscape continues evolving with technological advances, regulatory changes, and market pressures shaping future interactions between payers and providers.
Value-based payment models increasingly replace traditional fee-for-service arrangements. These models tie reimbursement to quality metrics and patient outcomes rather than service volume, requiring providers to track and report additional performance data.
Artificial intelligence and machine learning enable healthcare payer organizations to identify billing patterns and potential fraud more effectively. This technological advancement demands even greater accuracy and consistency in billing practices.
Price transparency requirements mandate that healthcare payer organizations disclose negotiated rates and coverage information publicly. This increased transparency creates opportunities for providers to benchmark their contracted rates and negotiate more effectively.
Understanding how to work effectively with comprehensive revenue cycle management services helps practices navigate these complex relationships while maintaining financial stability.
Successfully managing healthcare payer relationships requires expertise across multiple domains including regulatory compliance, technology integration, and strategic communication. Understanding payer-specific requirements and implementing systematic processes for eligibility verification, claim submission, and denial management directly impacts financial performance and operational efficiency. Greenhive Billing Solutions provides comprehensive revenue cycle management services designed to optimize healthcare payer interactions, reduce denials, and maximize reimbursements while allowing your practice to focus on delivering exceptional patient care.