Healthcare providers face complex financial challenges, and understanding reimbursement in medical billing is critical to maintaining a thriving practice. The reimbursement process determines how quickly and completely providers receive payment for services rendered, directly impacting cash flow and operational sustainability. For medical practices, clinics, and healthcare organizations, mastering the nuances of reimbursement requires knowledge of coding systems, payer contracts, compliance requirements, and claims management strategies. This comprehensive guide explores the essential elements of medical billing reimbursement and provides actionable insights to optimize your revenue cycle.
Understanding the Fundamentals of Medical Billing Reimbursement
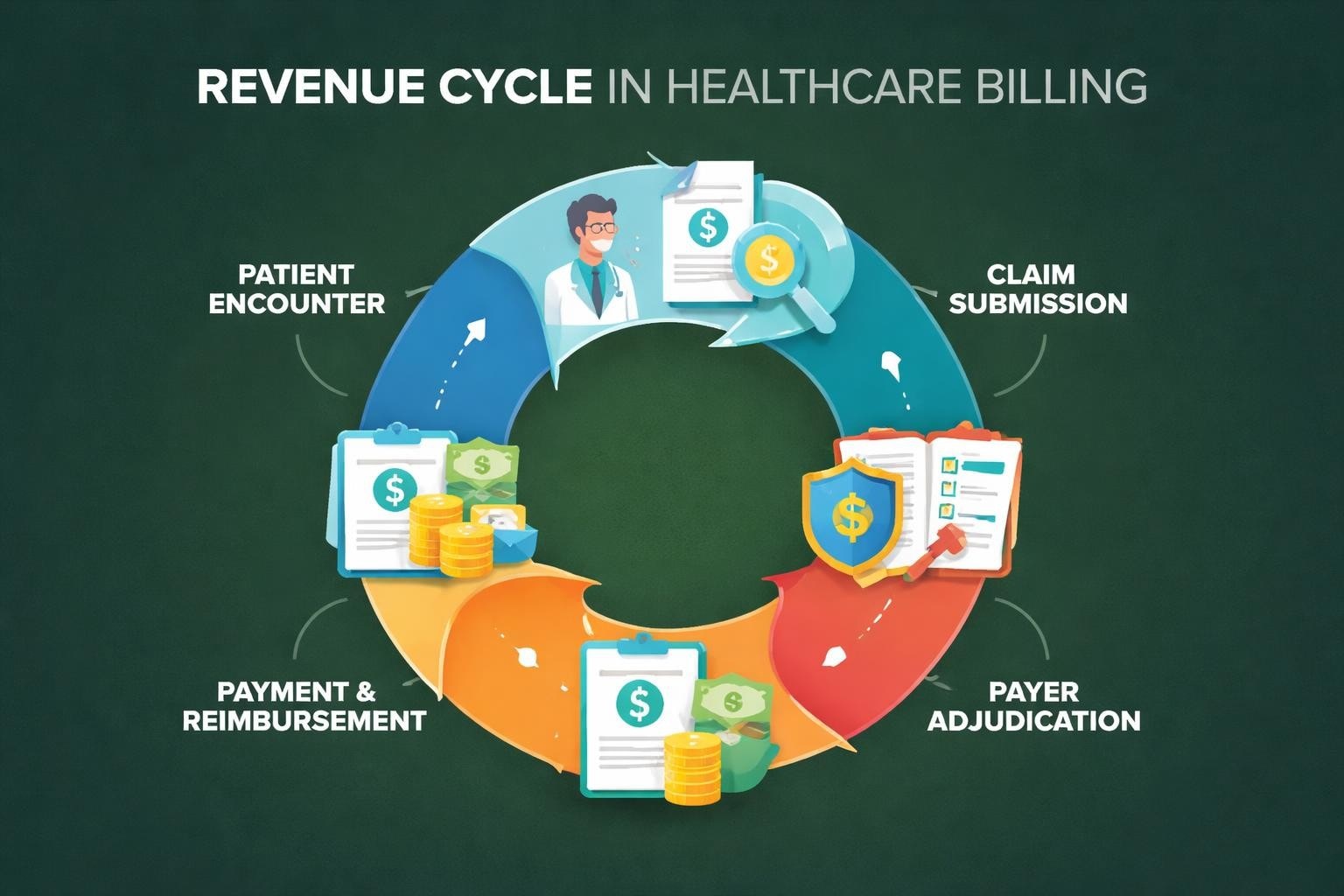
Reimbursement in medical billing represents the payment healthcare providers receive from insurance companies, government programs, and patients for delivered medical services. This process involves multiple stakeholders and requires precise documentation, accurate coding, and timely claim submission.
The reimbursement cycle begins when a patient receives care and extends through documentation, coding, claim submission, payer adjudication, and payment posting. Each step presents opportunities for optimization as well as potential pitfalls that can delay or reduce payments.
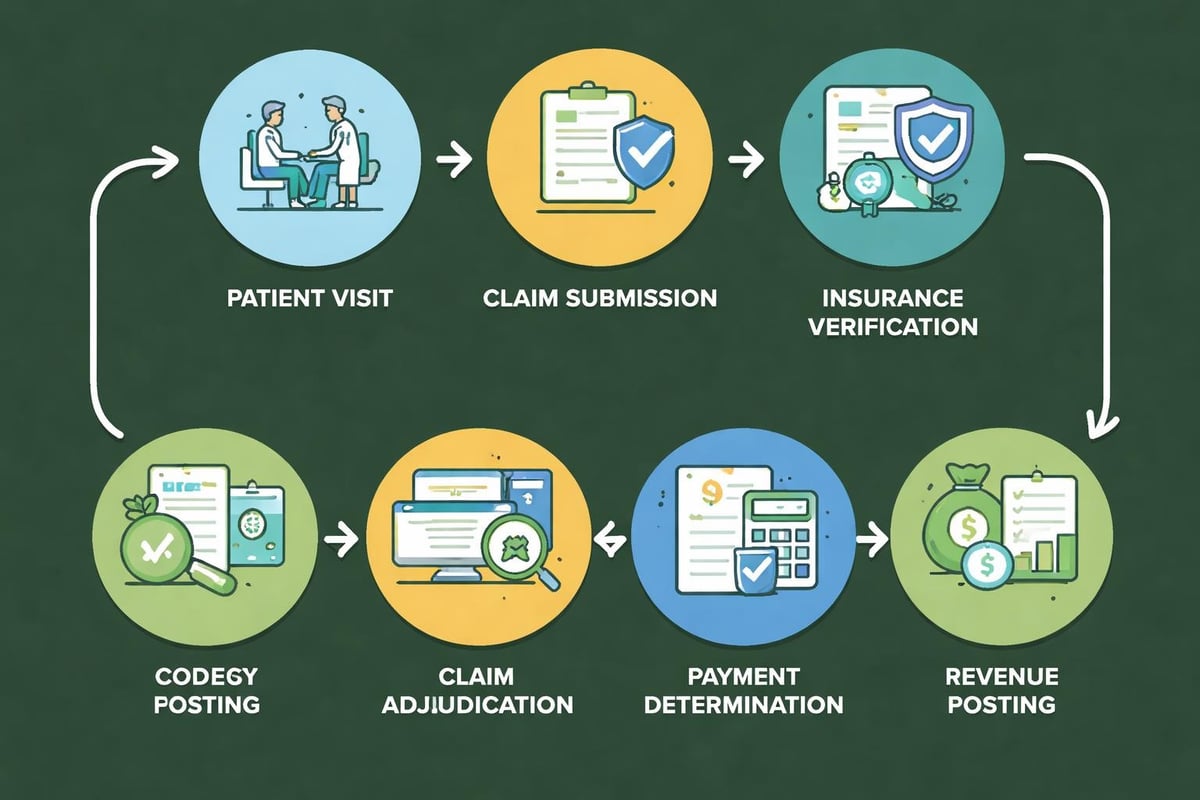
Key Components of the Reimbursement Process
Understanding medical billing fundamentals requires familiarity with several core components:
- Patient registration and insurance verification to confirm coverage and benefits
- Clinical documentation that accurately reflects services provided
- Medical coding using CPT, ICD-10, and HCPCS code sets
- Claim submission through electronic or paper channels
- Payer adjudication where insurers review and process claims
- Payment posting and reconciliation of received reimbursements
- Denial management for rejected or partially paid claims
Each component must function effectively to ensure optimal reimbursement outcomes. When healthcare providers partner with experienced revenue cycle management specialists, they gain access to expertise across all these areas, reducing errors and accelerating payment cycles.
Types of Reimbursement Models in Healthcare
Healthcare reimbursement operates under various payment models, each with distinct characteristics and requirements. Understanding these models helps providers anticipate payment amounts and structure their billing processes accordingly.
Fee-for-Service Reimbursement
Fee-for-service remains a prevalent model where providers receive payment for each service or procedure performed. This approach requires detailed documentation and precise coding to justify medical necessity and secure appropriate payment levels.
Providers must submit claims with accurate CPT codes that describe the specific services rendered. Payment rates typically follow predetermined fee schedules established by Medicare, Medicaid, or commercial payers.
Value-Based Reimbursement
Value-based care models shift focus from volume to quality outcomes. Providers receive incentives for meeting quality metrics, reducing readmissions, and improving patient satisfaction. These models include bundled payments, accountable care organizations, and pay-for-performance arrangements.
| Reimbursement Model | Payment Basis | Documentation Focus | Risk Level |
|---|---|---|---|
| Fee-for-Service | Per procedure/visit | Service details, medical necessity | Low provider risk |
| Capitation | Per patient per month | Patient panel management | Moderate risk |
| Bundled Payment | Per episode of care | Comprehensive episode documentation | High risk |
| Pay-for-Performance | Quality metrics achieved | Outcome measures, quality data | Variable risk |
Capitation and Per Diem Models
Capitation provides fixed monthly payments per enrolled patient regardless of service utilization. Per diem models pay a set daily rate for inpatient care. Both require robust population health management and careful monitoring of service costs relative to fixed payments.
Critical Factors Affecting Reimbursement Rates
Multiple variables influence how much providers ultimately receive for their services. Reimbursement in medical billing depends on payer mix, contract negotiations, coding accuracy, and compliance with billing regulations.
Payer Contract Terms
Commercial insurance contracts establish allowed amounts for each service code. Negotiating favorable contract terms directly impacts revenue potential. Providers should regularly review payer contracts to identify opportunities for renegotiation, especially when demonstrating quality outcomes or serving essential patient populations.
Medicare and Medicaid rates follow government-established fee schedules that vary by geographic location and service type. Understanding these schedules helps providers anticipate revenue and make informed decisions about service offerings.
Coding Accuracy and Specificity
Proper coding ensures providers receive appropriate reimbursement for services rendered. Physician coding and reimbursement practices have evolved significantly, with increased emphasis on documentation specificity and accurate code assignment.
Undercoding leaves money on the table by not capturing the full complexity of services provided. Overcoding risks compliance violations and payer audits. The solution lies in comprehensive documentation that supports the assigned codes and regular training for clinical and billing staff.

Common Challenges in Medical Billing Reimbursement
Healthcare providers encounter numerous obstacles in securing timely and complete reimbursement. Identifying these challenges allows practices to implement preventive strategies and improve overall revenue cycle performance.
Claim Denials and Rejections
Denials represent one of the most significant threats to healthy revenue cycles. Common denial reasons include:
- Missing or incorrect patient information
- Lack of prior authorization
- Coding errors or mismatches
- Services deemed not medically necessary
- Timely filing limit violations
- Coordination of benefits issues
Effective denial management requires systematic tracking, root cause analysis, and process improvements to prevent recurring issues. Reimbursement coding strategies emphasize proactive approaches to minimize denials before they occur.
Insurance Verification Failures
Verifying coverage before service delivery prevents claim rejections due to inactive policies or inaccurate patient information. Real-time eligibility verification has become essential for reducing front-end revenue cycle issues.
When verification processes fail, providers may deliver services to patients with lapsed coverage or incorrect benefit information, leading to unpaid claims and difficult patient collection scenarios.
Documentation Deficiencies
Incomplete or unclear clinical documentation undermines coding accuracy and claim justification. Payers increasingly scrutinize medical necessity, requiring detailed notes that explain why specific services were provided and how they benefited the patient.
Regular documentation audits help identify common deficiencies and create targeted improvement initiatives. Training physicians and clinical staff on documentation requirements bridges the gap between clinical care and billing requirements.
Best Practices for Optimizing Reimbursement
Successful reimbursement in medical billing requires strategic approaches across the entire revenue cycle. Implementing these best practices helps healthcare organizations maximize legitimate revenue while maintaining compliance.
1. Implement Robust Front-End Processes
Collecting accurate patient information and verifying insurance eligibility at registration prevents downstream issues. Train front-desk staff on proper data collection techniques and use technology to automate verification processes when possible.
2. Enhance Clinical Documentation
Partner with clinical teams to improve documentation quality and completeness. Use templates and prompts within electronic health records to capture necessary details for accurate coding. Conduct regular feedback sessions to address documentation gaps.
3. Invest in Coding Excellence
Ensure coders receive ongoing education on coding updates, payer-specific requirements, and specialty-specific nuances. Consider specialty-focused coding expertise for complex service lines. Regular coding audits identify improvement opportunities and reduce compliance risks.
4. Accelerate Claim Submission
Submit clean claims promptly to maximize cash flow and avoid timely filing denials. Electronic claim submission reduces processing time and allows for immediate error identification. Establish workflows that move claims from charge capture to submission within 24-48 hours.
5. Monitor Key Performance Indicators
Track metrics that reveal revenue cycle health and reimbursement efficiency:
| Metric | Target Range | Significance |
|---|---|---|
| Days in A/R | 30-40 days | Speed of payment collection |
| Clean Claim Rate | >95% | First-pass claim acceptance |
| Denial Rate | <5% | Claim quality and payer issues |
| Collection Rate | >95% | Overall revenue capture |
| Coding Accuracy | >98% | Compliance and revenue integrity |
Regular review of these indicators allows for early intervention when performance declines.
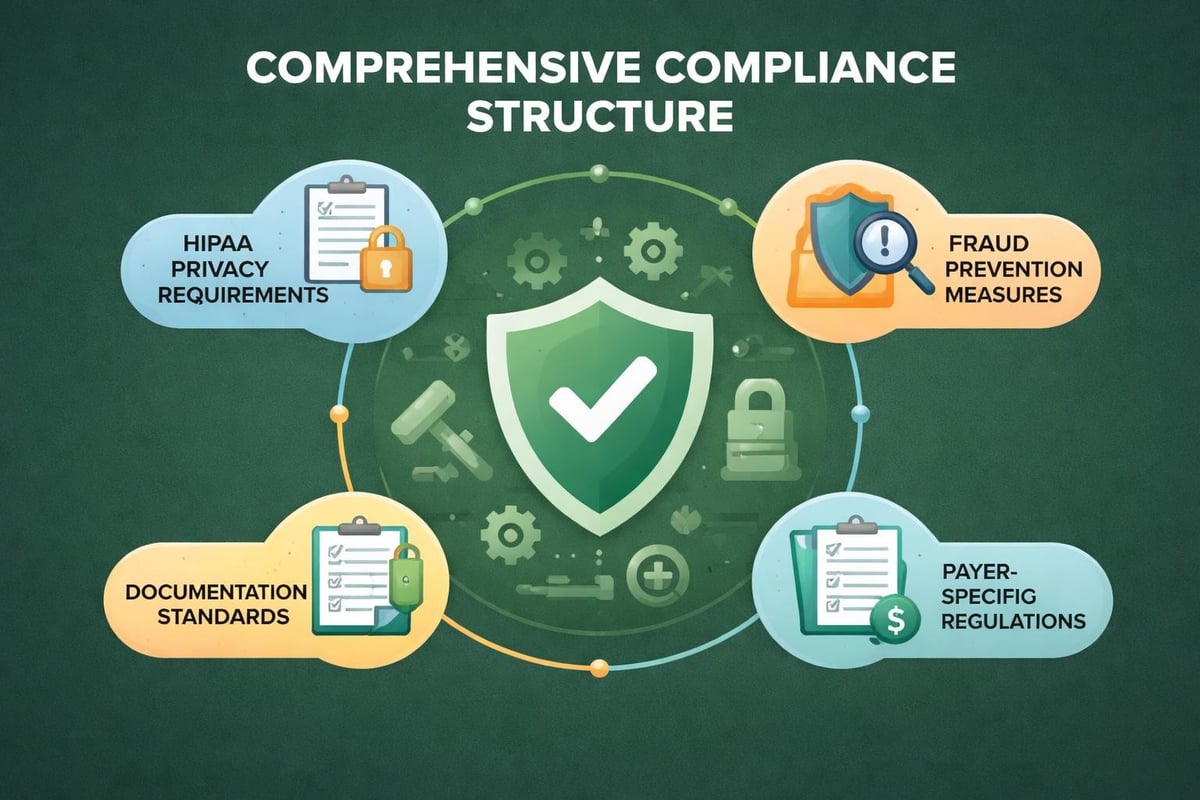
Regulatory Compliance and Reimbursement
Maintaining compliance with healthcare regulations protects providers from audits, penalties, and revenue disruptions. Healthcare regulations impact medical billing practices through changing coding requirements, documentation standards, and reimbursement policies.
HIPAA and Privacy Requirements
All billing activities must comply with HIPAA privacy and security regulations. Billing staff need access to protected health information to process claims, but this access must be limited to the minimum necessary and protected through appropriate safeguards.
Business associate agreements ensure third-party billing companies maintain the same privacy standards as covered entities. Regular training keeps staff current on privacy requirements and breach prevention.
Fraud and Abuse Prevention
Healthcare providers must avoid practices that constitute fraud or abuse, including billing for services not rendered, upcoding, unbundling, and duplicate billing. Compliance programs should include:
- Regular internal audits
- Clear policies and procedures
- Staff education on billing compliance
- Monitoring of coding and billing patterns
- Procedures for reporting and addressing compliance concerns
Medicare and Medicaid Requirements
Government payers impose specific documentation and billing requirements that often exceed commercial payer standards. Understanding Medicare conditions of participation, coverage determinations, and local coverage decisions prevents claim denials and audit exposure.
Technology's Role in Reimbursement Optimization
Modern revenue cycle management leverages technology to improve accuracy, efficiency, and reimbursement outcomes. While many solutions exist in the marketplace, the key lies in effective utilization of these tools by skilled professionals.
Practice Management and Billing Systems
Comprehensive practice management systems integrate scheduling, registration, charge capture, claims processing, and payment posting. These platforms enable workflow automation, reduce manual data entry errors, and provide real-time visibility into revenue cycle status.
Clearinghouses and Electronic Claims
Electronic claim submission through clearinghouses allows for pre-submission claim scrubbing that identifies errors before payers receive claims. This front-end error detection dramatically improves clean claim rates and reduces processing time.
Analytics and Reporting Tools
Data analytics reveal patterns in denials, payer performance, procedure profitability, and productivity metrics. Advanced reporting capabilities enable revenue cycle teams to make data-driven decisions about process improvements and resource allocation.
Experienced revenue cycle management professionals utilize these technological platforms to deliver superior results for healthcare providers, combining system capabilities with human expertise and judgment.
Strategies for Denial Management and Appeals
Even with optimal processes, some claims will face denials. Effective denial management recovers revenue that might otherwise be lost and identifies systemic issues requiring correction.
Step-by-Step Denial Resolution Process
Step 1: Categorize denials by reason code to identify patterns and prioritize high-value appeals.
Step 2: Review clinical documentation and payer policies to determine appeal viability.
Step 3: Gather supporting documentation including medical records, payer guidelines, and coverage policies.
Step 4: Submit appeals with clear explanations addressing the specific denial reason.
Step 5: Track appeal outcomes and timelines to ensure follow-through and measure success rates.
Preventive Approaches
While appeals recover denied revenue, prevention proves more cost-effective. Root cause analysis of denial trends identifies opportunities for process improvements, staff education, or payer communication that eliminates recurring denial reasons.
Working with experienced billing professionals provides access to extensive knowledge of payer-specific requirements and effective appeal strategies across multiple insurance companies and government programs.
Patient Responsibility and Collections
As high-deductible health plans become more common, patient responsibility represents a growing portion of practice revenue. Reimbursement in medical billing now includes strategies for collecting patient portions efficiently and respectfully.
Upfront Collections
Estimate patient responsibility before service delivery and collect applicable copays, deductibles, and coinsurance at the time of service. Point-of-service collections prove far more successful than attempting to collect after patients leave the office.
Payment Plans and Financial Policies
Clear financial policies help patients understand their obligations and available payment options. Offering payment plans for larger balances improves collection rates while maintaining positive patient relationships.
Technology solutions enable automated payment reminders, online payment portals, and text-based payment options that align with patient preferences and increase collection efficiency.
Working with Revenue Cycle Management Partners
Many healthcare providers recognize that maximizing reimbursement requires specialized expertise and dedicated resources. Partnering with professional revenue cycle management services allows practices to focus on patient care while ensuring optimal financial performance.
Professional RCM teams bring extensive knowledge of medical billing procedures and submission guidelines, payer-specific requirements, and industry best practices. These specialists work with existing systems and adapt to each provider's unique needs and workflows.
Benefits of Professional RCM Services
- Access to certified medical coders and billing specialists
- Reduced overhead costs compared to in-house billing departments
- Expertise in complex specialty billing requirements
- Dedicated denial management and appeals resources
- Compliance monitoring and audit support
- Advanced analytics and performance reporting
Selecting the Right Partner
When evaluating potential RCM partners, healthcare providers should consider track record, industry experience, technology capabilities, transparency in reporting, and alignment with practice values and goals.
The most effective partnerships involve collaborative relationships where RCM teams function as extensions of the provider's own organization, maintaining regular communication and shared commitment to patient satisfaction alongside financial performance.
Staying Current with Payer Policy Changes
Insurance companies regularly update coverage policies, billing requirements, and reimbursement rates. Staying informed about these changes prevents claim denials and ensures appropriate payment for services rendered.
Monitoring updates from major payers, participating in provider education sessions, and reviewing payer bulletins helps billing teams maintain current knowledge. Professional associations and industry publications also provide valuable information about policy changes affecting reimbursement.
Quarterly reviews of top payer policies and reimbursement rates allow practices to adjust workflows, update fee schedules, and educate staff on new requirements before they impact revenue.
Understanding Evaluation and Management coding updates is particularly important, as E/M services represent a significant portion of reimbursement for many specialties and frequently undergo guideline revisions.
Mastering reimbursement in medical billing requires attention to detail, ongoing education, and systematic processes across the entire revenue cycle. By implementing best practices in coding, documentation, claims processing, and denial management, healthcare providers can significantly improve their financial performance while maintaining compliance with regulatory requirements. Greenhive Billing Solutions delivers comprehensive revenue cycle management services that help healthcare providers maximize legitimate reimbursements through expert billing, coding, claims processing, and denial management, allowing you to focus on delivering exceptional patient care while we optimize your financial operations.