Healthcare providers face mounting administrative challenges in today's complex reimbursement landscape. Among the most critical yet time-consuming processes is provider credentialing, which directly impacts a practice's ability to bill insurance companies and receive timely payments. Many healthcare organizations turn to a medical credentialing company to navigate this intricate process, ensuring compliance while freeing internal staff to focus on patient care. Understanding the role these specialized partners play in revenue cycle management can help practices make informed decisions about outsourcing this essential function.
Understanding the Scope of Medical Credentialing Services
A medical credentialing company specializes in verifying healthcare providers' qualifications, licenses, certifications, and work history to ensure they meet the standards set by insurance payers, hospitals, and regulatory bodies. This verification process is fundamental to maintaining quality and compliance in healthcare settings, protecting both patients and healthcare organizations from potential liability issues.
Core Verification Components
The credentialing process encompasses multiple verification layers that require meticulous attention to detail:
- Primary source verification of medical degrees and training certificates
- License verification across all states where the provider practices
- Board certification status confirmation through specialty boards
- Work history verification including gaps in employment
- Malpractice insurance coverage and claims history review
- DEA registration and controlled substance prescribing authority
- Hospital privileges and affiliations documentation
These elements form the foundation of a comprehensive credentialing file that insurance companies review before granting network participation.

The Credentialing Timeline and Its Revenue Impact
Provider credentialing is notoriously time-intensive, typically requiring 90 to 120 days for initial enrollment with most insurance carriers. Some payers may extend this timeline to 180 days, creating significant revenue delays for practices adding new providers or expanding into new markets.
| Credentialing Phase | Typical Duration | Key Activities |
|---|---|---|
| Application Preparation | 1-2 weeks | Document gathering, form completion |
| Primary Source Verification | 4-6 weeks | License checks, education confirmation |
| Payer Review | 6-12 weeks | Application processing, committee review |
| Final Approval & Setup | 2-4 weeks | Contract execution, system enrollment |
During this extended period, new providers cannot bill insurance companies for their services, forcing practices to either delay patient appointments or accept the financial burden of uncompensated care. A medical credentialing company can help minimize these delays through proactive application management and follow-up procedures.
Financial Implications of Credentialing Delays
The revenue impact of credentialing delays extends beyond the obvious loss of billable services. Practices face several cascading financial challenges:
Lost revenue opportunities accumulate quickly when providers cannot see insurance-covered patients. A single physician generating $50,000 monthly in collections loses substantial income during credentialing delays.
Patient access limitations force practices to turn away patients or schedule them months in advance, potentially losing them to competitors. This affects both immediate revenue and long-term patient panel development.
Administrative overhead increases as staff spend time explaining delays to frustrated patients and rescheduling appointments, diverting resources from productive revenue cycle activities.
Navigating Insurance Payer Requirements
Each insurance company maintains unique credentialing requirements, application formats, and processing procedures. A medical credentialing company brings expertise in managing these varying standards, ensuring applications meet each payer's specific criteria on the first submission.
Commercial Insurance Credentialing
Commercial payers like Blue Cross Blue Shield, UnitedHealthcare, Aetna, and Cigna each operate distinct credentialing departments with different application portals, documentation requirements, and processing timelines. Understanding these nuances requires dedicated expertise that most practice administrators cannot maintain alongside their other responsibilities.
The credentialing process with commercial insurers involves thorough review by credentialing committees that meet on fixed schedules, often monthly or quarterly. Missing a committee meeting deadline can add weeks or months to the approval timeline.
Government Program Enrollment
Medicare and Medicaid enrollment introduces additional complexity through the PECOS (Provider Enrollment, Chain, and Ownership System) and state-specific Medicaid portals. These government programs require enhanced screening levels, fingerprinting in some cases, and extensive ownership disclosure documentation.
Recent regulatory changes have increased enrollment scrutiny, particularly around practice location verification and telehealth service delivery. A medical credentialing company stays current with these evolving requirements, preventing application rejections due to regulatory misunderstandings.
Re-Credentialing and Ongoing Maintenance
Credentialing is not a one-time event but an ongoing compliance requirement. Most insurance companies require re-credentialing every two to three years, while professional licenses, DEA registrations, and board certifications have their own renewal cycles.
Critical Expiration Monitoring
Allowing any credential to lapse can result in immediate termination from insurance networks, creating revenue disruption and requiring complete re-enrollment. Maintaining consistent provider quality requires vigilant tracking of multiple expiration dates across numerous credentials.
- Professional medical licenses (renewal cycles vary by state)
- DEA registration (three-year renewal cycle)
- Board certifications (various renewal periods by specialty)
- Malpractice insurance policies (typically annual renewal)
- CLIA certificates for laboratories (two-year renewal)
- State-specific permits and authorizations
A medical credentialing company maintains comprehensive tracking systems that monitor these dates and initiate renewal processes well before expiration, preventing network participation interruptions.
CAQH ProView and Centralized Data Management
The Council for Affordable Quality Healthcare (CAQH) ProView system serves as a centralized database where providers maintain their credentialing information. Most commercial insurance companies pull provider data from CAQH, making accurate profile maintenance essential for efficient credentialing.
Optimizing CAQH Profile Management
A complete and current CAQH profile accelerates credentialing with participating payers. However, providers must update their profiles within specific timeframes and re-attest to information accuracy every 120 days to maintain active status.
Profile incompleteness or attestation lapses trigger automatic status changes that delay credentialing applications. Many practices struggle with consistent CAQH maintenance due to competing priorities, making this a valuable area where a medical credentialing company provides ongoing support.
Delegated Credentialing Arrangements
Some healthcare organizations qualify for delegated credentialing authority, allowing them to credential providers on behalf of insurance companies under established agreements. This arrangement can significantly reduce credentialing timelines but requires substantial infrastructure, policies, and compliance monitoring.
| Credentialing Type | Timeline | Oversight | Best For |
|---|---|---|---|
| Traditional Payer Credentialing | 90-180 days | Insurance company | Small to mid-size practices |
| Delegated Credentialing | 30-60 days | Healthcare organization | Large groups, hospitals, IPAs |
| Hospital Privileging | 60-120 days | Medical staff office | Inpatient providers |
Organizations with delegated credentialing authority must maintain rigorous standards that meet or exceed payer requirements, including regular audits by insurance companies. A medical credentialing company can help organizations establish delegated credentialing programs or work within existing frameworks to optimize provider onboarding.
Common Credentialing Challenges and Solutions
Healthcare practices encounter numerous obstacles during the credentialing process that can extend timelines and delay revenue realization. Understanding these common pitfalls helps organizations implement preventive measures.
Application Errors and Incomplete Documentation
The most frequent cause of credentialing delays stems from incomplete applications or missing documentation. Insurance companies immediately reject applications with gaps, requiring resubmission that adds weeks to the process.
Following practical tips for a smooth credentialing process can help avoid these delays. A medical credentialing company employs quality control procedures that catch errors before submission, ensuring applications meet all requirements on the first attempt.
Gaps in Work History
Providers must account for every period since completing their training. Unexplained gaps in work history trigger additional scrutiny and information requests from credentialing committees. Even legitimate gaps for parental leave, research, or education require proper documentation and explanation.
Step 1: Identify all time periods since completing residency or fellowship training
Step 2: Document employment, practice ownership, or other professional activities for each period
Step 3: Prepare explanations and supporting documentation for any gaps exceeding 30 days
Step 4: Include relevant activities like consulting, locum tenens, volunteer work, or additional training
Step 5: Obtain verification letters from organizations where formal employment records may not exist
Malpractice Claims History Disclosure
Providers must disclose all malpractice claims, settlements, and judgments regardless of fault determination or payment amount. Failure to disclose known claims constitutes misrepresentation and can result in application denial and potential network termination even after approval.
A medical credentialing company helps providers navigate sensitive disclosure requirements, ensuring complete transparency while presenting information in the most favorable light permitted by regulations.
Integration with Revenue Cycle Management
Credentialing directly impacts revenue cycle performance, making it an essential component of comprehensive financial management for healthcare practices. The connection between provider enrollment and billing efficiency requires coordinated attention across multiple operational areas.
Insurance Verification Dependencies
Patient insurance verification and benefits confirmation depend on accurate provider credentialing data within payer systems. When credentialing information hasn't properly loaded into insurance databases, claims get rejected even after providers receive approval letters.
This common issue creates claim denials coded as "provider not found" or "provider not eligible," requiring manual intervention and resubmission. Organizations working with Greenhive Billing Solutions benefit from integrated credentialing awareness within the claims processing workflow, allowing faster identification and resolution of enrollment-related rejections.
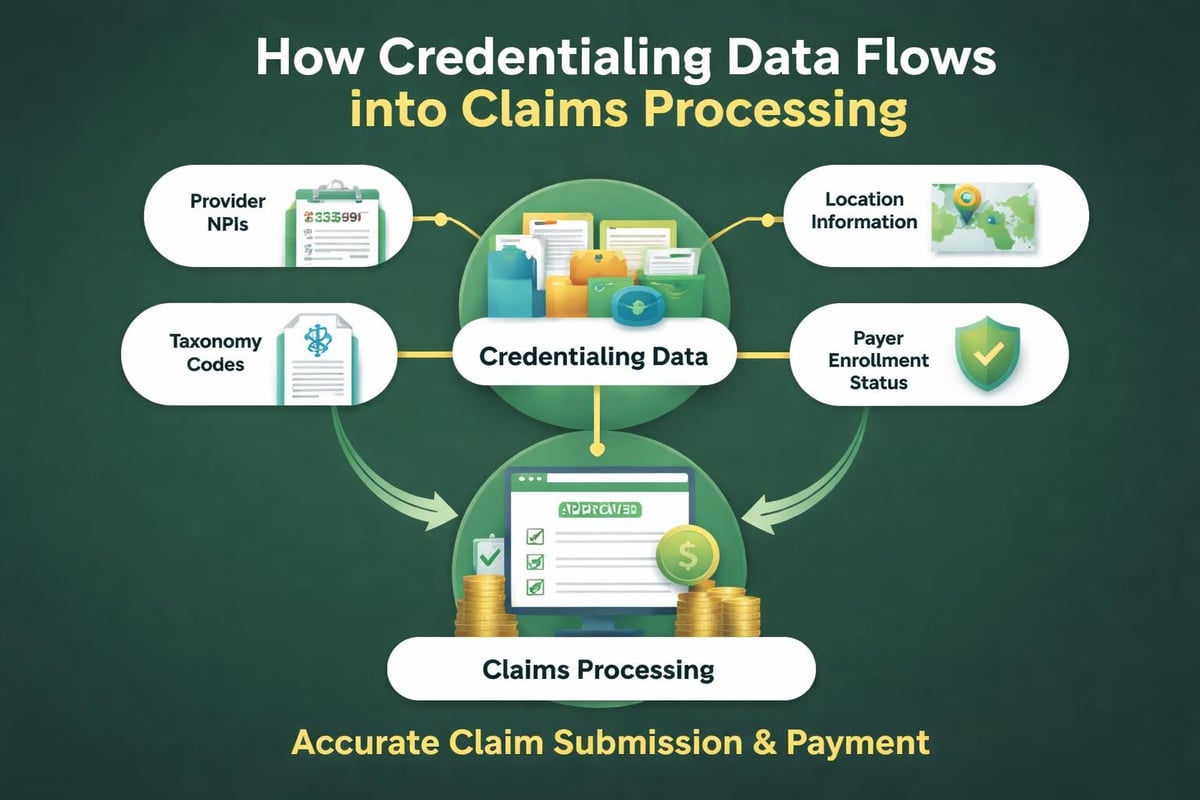
Claims Processing Optimization
Properly completed credentialing establishes the foundation for clean claims submission. Provider NPIs, taxonomy codes, group affiliations, and service locations must match exactly between credentialing records and claim forms.
- NPI (National Provider Identifier) accuracy across all payer files
- Correct taxonomy codes for each provider's specialty and subspecialty
- Accurate service location information and place of service codes
- Proper group versus individual provider designation
- Correct rendering versus billing provider relationships
Selecting the Right Medical Credentialing Partner
Healthcare practices considering outsourcing credentialing services should evaluate potential partners against specific criteria that indicate expertise, reliability, and alignment with practice needs.
Essential Service Capabilities
A comprehensive medical credentialing company should offer services that address the full credentialing lifecycle, not just initial applications. Look for partners providing:
Initial credentialing with all relevant commercial and government payers in your service area
Re-credentialing management with automated tracking and timely renewal processing
CAQH profile maintenance including regular updates and timely attestation
Expiration monitoring for licenses, certifications, and other time-sensitive credentials
Payer enrollment troubleshooting to resolve processing delays and application issues
Roster maintenance ensuring accurate provider information across all payer systems
Industry Standards and Compliance
Credentialing partners should demonstrate familiarity with ideal credentialing standards established by professional organizations like NAMSS (National Association Medical Staff Services). These standards provide framework for essential data elements and verification procedures that ensure thorough, compliant credentialing.
| Evaluation Criteria | Questions to Ask | Red Flags |
|---|---|---|
| Experience | How many providers do you credential annually? What specialties? | Limited experience with your specialty |
| Transparency | How do you communicate status updates? | Vague reporting, poor responsiveness |
| Compliance | What quality control procedures do you follow? | No formal QC process |
| Technology | What systems do you use for tracking and reporting? | Manual processes, no provider portal |
Communication and Reporting Standards
Effective credentialing requires ongoing communication between the credentialing company, healthcare providers, and practice administrators. Evaluate how potential partners handle status updates, documentation requests, and issue resolution.
Look for partners offering provider portals where you can check application status, upload documents, and review credentialing files. Regular status reports should detail progress with each payer, pending items, and projected completion dates.
Specialized Credentialing Scenarios
Certain practice situations introduce additional credentialing complexity requiring specialized expertise. A medical credentialing company with broad experience can navigate these scenarios more efficiently than practices handling them independently.
Multi-State Practice Credentialing
Providers licensed and practicing in multiple states face compounded credentialing requirements. Each state's professional license must be verified, and insurance companies may have different credentialing procedures for different geographic regions.
Telehealth expansion has increased multi-state credentialing needs, as providers must be licensed and credentialed in states where their patients are located during virtual visits. Interstate medical licensure compacts have simplified licensing in some cases, but credentialing requirements remain payer-specific.
Hospital Privileging Coordination
Physicians providing inpatient care must maintain hospital privileges in addition to insurance credentialing. Hospital medical staff offices conduct their own credentialing process, often with more stringent peer reference requirements and clinical competency evaluation.
Coordinating hospital privileging with insurance credentialing ensures providers can deliver comprehensive care across all settings. A medical credentialing company familiar with both processes can streamline document preparation and avoid duplicative verification requests.
Group Practice and Provider Transitions
When providers join or leave group practices, credentialing updates must occur across all payer networks. New providers need enrollment under the group's tax ID, while departing providers require termination processing to prevent claims submission issues.
Mid-contract provider transitions introduce timing challenges, as insurance companies may resist processing changes outside standard credentialing cycles. Understanding the complete credentialing process including contractual aspects helps practices navigate these transitions with minimal revenue disruption.
Technology and Automation in Modern Credentialing
While credentialing remains fundamentally a verification-intensive process requiring human expertise, technology has introduced efficiencies in tracking, document management, and payer communication.
Credentialing Software Platforms
Modern credentialing management platforms centralize provider information, automate expiration tracking, and facilitate electronic document submission to payers. These systems generate alerts for upcoming deadlines and maintain audit trails of all credentialing activities.
A medical credentialing company utilizing robust technology platforms can offer practices visibility into the credentialing process through web portals, reducing the need for status inquiry emails and phone calls. Real-time access to application status helps practices plan provider schedules and patient access more effectively.
Electronic Verification Processes
Many verification sources now offer electronic queries that reduce verification turnaround time. The National Practitioner Data Bank, state licensing boards, and specialty certifying boards provide online verification tools that credentialing specialists can access directly.
However, primary source verification still requires contacting medical schools, residency programs, and previous employers directly. These manual processes remain time-consuming and represent the primary bottleneck in credentialing timelines.
The Business Value of Professional Credentialing Services
Outsourcing credentialing to a specialized medical credentialing company delivers measurable business value beyond simply freeing staff time. Practices should evaluate credentialing partners as strategic revenue cycle partners rather than administrative vendors.
Quantifiable Benefits
Faster time to revenue when new providers can begin seeing insured patients weeks earlier due to efficient application processing and payer follow-up.
Reduced administrative burden allowing practice staff to focus on patient scheduling, clinical support, and other high-value activities instead of credentialing paperwork.
Improved accuracy through specialized expertise and quality control processes that prevent application errors and subsequent delays.
Compliance assurance with regulatory requirements and payer standards that protect practices from potential sanctions or network termination.
Return on Investment Considerations
The cost of credentialing services must be weighed against the revenue impact of doing credentialing internally or delaying provider productivity. Consider that a single physician generating $400,000 annually in collections produces approximately $33,000 monthly in revenue.
Reducing credentialing time by even four weeks through professional services creates $33,000 in additional revenue for that provider. When compared to typical credentialing service fees of $500-$2,000 per provider per payer, the return on investment becomes immediately apparent.
Credentialing's Role in Practice Growth Strategies
Healthcare organizations expanding through provider recruitment, service line development, or geographic growth must incorporate credentialing timelines into their strategic planning. A medical credentialing company becomes an essential partner in executing growth initiatives successfully.
New Provider Onboarding
Physician recruitment represents significant investment in search fees, signing bonuses, and compensation guarantees. Maximizing return on this investment requires getting new providers productive as quickly as possible, making credentialing a critical path item in the onboarding process.
Start credentialing immediately upon contract signing, ideally during the recruitment process itself when possible
Prioritize payers based on patient volume and reimbursement rates to focus on highest-value networks first
Plan provider start dates accounting for realistic credentialing timelines rather than optimistic projections
Prepare contingency plans for cash-pay services or hospital employment arrangements during credentialing completion
Service Line Expansion
Adding new service lines often requires additional credentialing for existing providers, such as obtaining new taxonomy codes or facility-based privileges. Insurance companies may require separate applications for new specialties or subspecialties even when providers are already in-network for their primary specialty.
A medical credentialing company helps practices navigate these expansion credentialing requirements, ensuring new services can be billed appropriately from their launch date.
Effective credentialing management forms the foundation of successful revenue cycle performance, directly impacting provider productivity and practice financial health. Healthcare organizations benefit significantly from partnering with specialists who navigate this complex process efficiently while maintaining compliance with evolving regulatory requirements. Greenhive Billing Solutions understands the critical connection between credentialing, enrollment, and revenue optimization, offering comprehensive support that ensures providers can focus on patient care while maintaining seamless financial operations. Our revenue cycle management services integrate credentialing awareness with claims processing, denial management, and reimbursement optimization to deliver maximum financial performance for practices across the United States.